DIFFERENTIAL DIAGNOSIS OF HIP PAIN
Do you sometimes struggle with differential diagnosis of hip pain?
You are not alone! This is a common problem, so I’ve developed some great resources here for you, to help you on your way to becoming a skilled diagnostician.
DIFFERENTIAL DIAGNOSIS OF HIP PAIN
Do you sometimes struggle with differential diagnosis of hip pain?
You are not alone! This is a common problem, so I’ve developed some great resources here for you, to help you on your way to becoming a skilled diagnostician.
The differential diagnosis of hip pain can be a challenging task due to the number of potential local sources of nociception and relative complexity in anatomical relationships within structures of the anterior hip, groin, lateral hip and buttock. This is compounded by more remote sources within the lumbar spine and non-musculoskeletal sources within the pelvis.
While it's not always important to put a diagnostic label on a patient's presenting condition, the patient usually wants to know: What, Why and How? 'What is causing this pain?' ; 'Why do I have this problem'; 'How can you help/how can I help myself?' Your differential diagnosis process forms an important part of your clinical reasoning, helping you determine what structures may be responsible for local nociception or referral (for those who still have nociceptive pain) and which mechanisms might be at play.
One of the most common questions I get from physiotherapists and other health professionals is:
Where do I start with differential diagnosis of hip pain?
It really helps to have a framework that contains a virtual directory of the potential sources of local nociception and more remote sources of pain referral, and a road map for how we might recognise these conditions.
Do we rush through chatting with the patient and jump straight into physical testing? No! The patient interview is absolutely filled with GOLD! By the time you have finished your patient interview, you should have narrowed down the possibilities to a few main options. This makes the physical assessment then much more targeted and manageable.
So far within my how-to video library, I have recorded over 70 diagnostic tests for the hip and pelvic region!! This is separate from the many other videos on range of motion assessments or other physical impairment tests. It is simply not possible to apply all the available physical tests for a region within one session, due to 1. Time limitations and 2. Risk of really provoking the patient’s pain. Furthermore, you end up with a whole heap of irrelevant data that you need to record and mentally sift through. Time wasting and exhausting!
The aim of this page and the detailed free ebook you can access here, is to guide you through the initial and arguably most important phases of the differential diagnosis. This information will:

Main Sources of Hip Pain
The flowchart below outlines the primary musculoskeletal sources of hip pain and a starting point for your differential diagnosis. It helps to start with an area of pain. If your patient’s area of pain is very broad, ill-defined or changeable, consider central mechanisms and referred or nerve-related pain. Keep in mind that particularly in older individuals or more chronic and/or severe conditions, there are often multiple co-existing sources of nociception, so there may be 2 or more different areas of pain or multiple sources of nociception underlying pain in one focal area. Being able to differentiate for example between tendon and bursal-related pain over the greater trochanter is unlikely to influence your ultimate treatment direction in most situations. However, it’s good to start with a framework of possibilities, so you don’t miss things in the culling process, where we aim to ‘rule out’ as many diagnoses as possible.
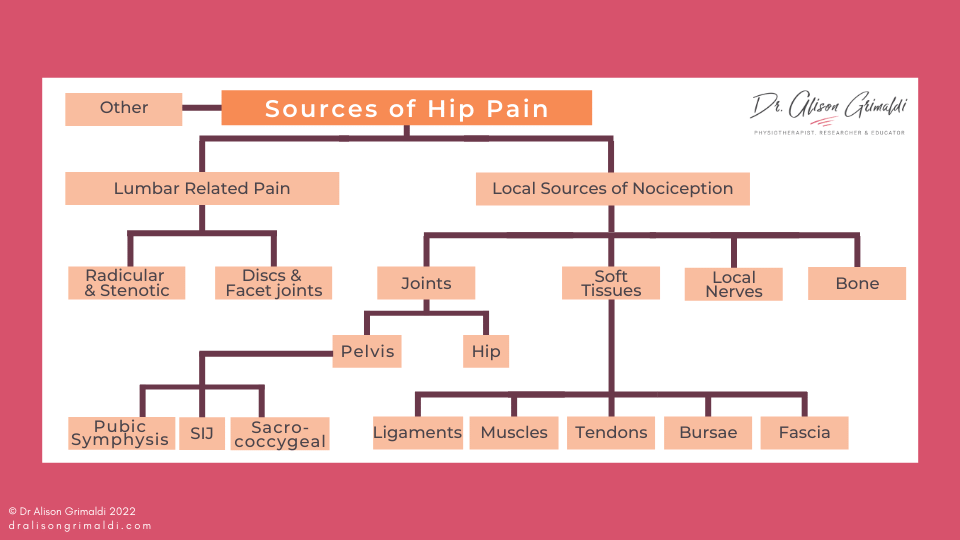
Using the flowchart above, start with the area of pain, visualise what structures are within or refer to the region. Breaking local sources of nociception into Joints, Soft Tissues, Nerves and Bone can help you consider all structures in the region.
Let’s take a closer look at each region, at the local structures …
Main Sources of Nociception, Referral and Common Diagnoses for Buttock Pain
Buttock pain often poses a diagnostic dilemma. The buttock is a large region, so it can be useful for your differential diagnosis to break the region down into segments - the parasacral, upper buttock, mid-buttock and lower buttock regions. Don't expect all patients to describe a focal region of pain in the buttock. The longer someone has had pain, the less distinct pain location often becomes. If someone's pain is much more global, your first 2 considerations would be pain referral e.g., lumbar spine or some central mechanisms at play. However, if the patient can identify a 'worse area' or the initial area - where it first started, that might give you some really helpful clues, together with your wider questioning in the patient interview. The table below will give you some ideas of diagnoses and main sources of local nociception and referral for each region. For further detail about other patient interview features that will help you in your differential diagnosis of hip pain, download the free ebook on this page.
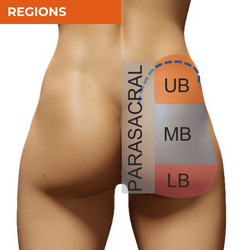
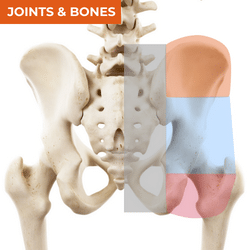
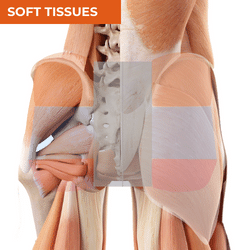
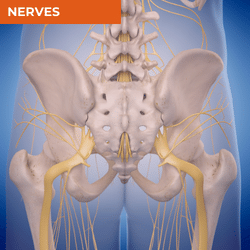
PARASACRAL PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Sacroiliac joint related pain
- Coccydynia
- Neuralgia - Sciatic/ Pudendal
LESS COMMON DIAGNOSES
- Enthesopathy
- Sacral bone stress injury
- Middle Cluneal Neuralgia
JOINTS & BONES
- Low lumbar vertebrae,
- L4-S1 intervertebral joints, discs and facet joints
- Sacrum and sacroiliac joint
- Coccyx and sacrococcygeal joint
- Medial ilium
SOFT TISSUES
- Ligaments – iliolumbar, long dorsal, sacrotuberous & sacrospinous
- Thoracodorsal fascia
- Multifidus, erector spinae, coccygeus/posterior pelvic floor
- Gluteus maximus & fascia
NERVES
- Lumbosacral nerve roots
- Sciatic nerve
- Middle cluneal nerves
- Pudendal nerve
- Perineal ramus
UPPER BUTTOCK PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
LESS COMMON DIAGNOSES
- Superior Cluneal Neuralgia
- Enthesopathy
JOINTS & BONES
- Ilium
SOFT TISSUES
- Insertions of quadratus lumborum & abdominal wall onto iliac crest
- Upper gluteus maximus
- Gluteal fascia
- Posterior aspects of gluteus medius & minimus
NERVES
- Superior cluneal nerves
- Superior gluteal nerve
MID BUTTOCK PAIN
COMMON DIAGNOSES
- Lx radicular or somatic pain
- Hip Joint Related Pain e.g., OA, FAIS, dysplasia, instability
- Musculotendinous injury
LESS COMMON DIAGNOSES
- Deep Gluteal Syndrome
- Mid/Sup Cluneal Neuralgia
JOINTS & BONES
- Hip Joint
- Acetabular column
- Femoral head & upper neck
SOFT TISSUES
- Gluteus maximus & fascia
- Posterolateral aspects of gluteus medius & minimus
- Piriformis, obturator internus, gemelli
- Obturator internus, obturator externus & trochanteric bursae
- Vascular structures of the deep gluteal space
NERVES
- Middle & superior cluneal nerves
- Deep gluteal space – sciatic, posterior femoral cutaneous, superior & inferior gluteal, pudendal, nerves to obturator internus, quadratus femoris & biceps femoris
LOWER BUTTOCK PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Proximal hamstring tendinopathy
- Ischial apophysitis
LESS COMMON DIAGNOSES
- Ischiofemoral Impingement
- Deep Gluteal Syndrome
- Inferior Cluneal Neuralgia
- Ischial avulsion
JOINTS & BONES
- Ischial tuberosity & ischiopubic ramus
- Proximal femur – femoral neck, lesser trochanter, posterior aspect of greater trochanter
SOFT TISSUES
- Gluteus maximus & fascia
- Quadratus femoris
- Obturator externus
- Proximal hamstring origins
- Adductor magnus origin
- Ischiogluteal bursa
NERVES
- Sciatic nerve
- Posterior femoral cutaneous nerve
- Inferior cluneal nerves
Local Sources of Nociception, Referral and Common Diagnoses for Lateral Hip Pain
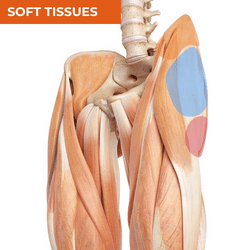
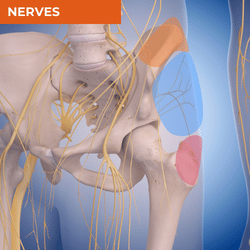
Lateral hip pain has almost become synonymous with gluteal tendinopathy or 'trochanteric bursitis,' however not all lateral hip pain can be attributed to soft tissue pathology at the greater trochanter. Location of pain in the lateral hip region can give you important clues about possible sources of local nociception or referral in your differential diagnosis process. While pain locally over the greater trochanter is more likely to be related to a soft tissue source such as gluteal tendinopathy, pain in the mid-zone between the greater trochanter and iliac crest is more likely to be related to the hip joint or acute myofascial injury. Iliac crest pain is most commonly related to enthesopathy or local neuralgia. The other major source will be the lumbar spine - either radicular or somatic pain which can present in any of these zones. The table below will provide you with the most common diagnoses in this region and structures that should be considered as potential sources of local nociception or referral.
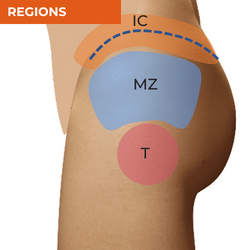
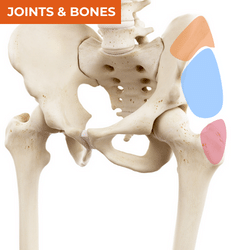
ILIAC CREST PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Enthesopathy - Abdominal wall, Tensor Fascia Lata Tendinopathy
LESS COMMON DIAGNOSES
- Neuralgia - Iliohypogastric, Subcostal
- Inflammatory enthesitis e.g. associated with spondyloarthropathy
JOINTS & BONES
- Neuralgia - Iliohypogastric, Subcostal
- Inflammatory enthesitis e.g. associated with spondyloarthropathy
SOFT TISSUES
- Abdominal wall enthesis - insertion of transversus abdominis, internal & external oblique
- Abdominal wall fascia, fascia lata & iliotibial band
- Gluteus medius (just below iliac crest) and Tensor Fascia Lata
NERVES
- Subcostal nerve
- Iliohypogastric nerve
MID ZONE PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Hip joint related pain
- Acute myofascial injury
LESS COMMON DIAGNOSES
- Greater Trochanter – Pelvic Impingement
- Iliohypogastric Neuralgia
JOINTS & BONES
- Lumbar joint structures & nerve roots
- Hip joint
- Ilium
- Acetabular column
- Femoral head/neck
SOFT TISSUES
- Gluteus medius, minimus and anterior portions of maximus & fascia
- Tensor Fascia Lata
- Reflected head of rectus femoris
- Fascia lata & iliotibial band
NERVES
- Iliohypogastric nerve - lateral cutaneous branch
- Subcostal nerve
- Superior gluteal nerve
- Superior cluneal nerves - lateral branches
TROCHANTERIC PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Gluteal tendinopathy (GTPS, trochanteric bursitis)
- Hip joint related pain
LESS COMMON DIAGNOSES
- Myotendinous or myofascial injury - abductors/rotators
- Bone stress injury or fracture
- Inflammatory enthesitis e.g. associated with spondyloarthropathy
- Iliohypogastric neuralgia
JOINTS & BONES
- Lumbar joint structures & nerve roots
- Hip Joint
- Greater trochanter
- Femoral head & neck
- Acetabular column
SOFT TISSUES
- Gluteus medius & minimus, piriformis, obturator, gemelli & quadratus femoris tendons
- Iliotibial band & gluteus maximus & Tensor Fascia Lata insertions
- Trochanteric bursae
NERVES
- Iliohypogastric nerve - lateral cutaneous branch
- Inferior gluteal nerve
- Lateral femoral cutaneous nerve

LEARNING RESOURCES
to Help you Master Differential Diagnosis of
LATERAL HIP & BUTTOCK PAIN
Online Course
Includes 3 months access to 6 hours of online lectures
Downloadable PDF notes
Downloadable professional development certificate (upon completion of course)
Online Workshop
Includes 3 months access to 6 hours of online lectures & pdf handouts
+
2 x 3 hours of live zoom workshops with Dr Alison Grimaldi & 6 weeks access to workshop recordings
Face to Face Workshop
Includes 3 months access to 6 hours of online lectures & pdf handouts + 8 hours of practical workshop.
Brisbane only at this stage. International venues will resume as the pandemic allows
Hip Academy
Hip Academy: The Ultimate Learning Experience - Current membership includes ongoing access to:
- All Online Hip Courses
- eBook Series
- How-to Video Library
- PDF Resource Library
- Live Zoom Meetings
- Hip Academy Forum
Local Sources of Nociception, Referral and Common Diagnoses for Anterior Hip Pain
Pain in the anterior hip region is too commonly attributed to the hip flexors. Overactivity or tightness in these muscles is often cited as a major cause of anterior hip pain. However, there is so much more to consider. Identification of joint-related pain is often delayed when there is excessive focus on the hip flexors. When the hip flexors are the source of the symptoms, the iliopsoas is often the primary muscle considered even though there are a number of other hip flexor muscles and tendons that should be considered. The specific area of pain and behaviour of that pain can give you valuable information in your differential diagnosis, even prior to your physical assessment. The individual before you and the activities they engage in will also be important to consider, for example, pain in the anterior hip region in endurance athletes should always raise suspicion of bone stress injury, while pain in an adolescent should raise suspicion of childhood bone conditions including apophysitis or slipped capital femoral epiphysis. There is lots of further information available in the free ebook available here, to help you recognise different conditions within your differential diagnosis of anterior hip pain.
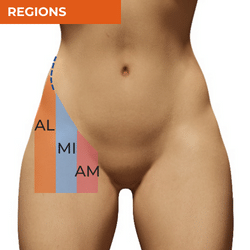
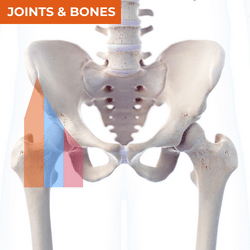
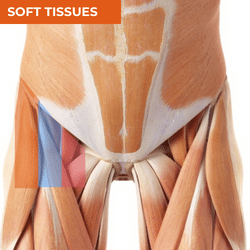
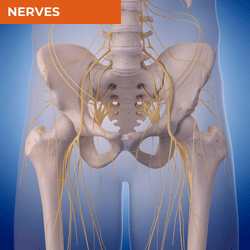
ANTEROMEDIAL HIP PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Hip joint related pain
- Musculotendinous pain/injury - pectineus, obturators & gemelli, iliopsoas
LESS COMMON DIAGNOSES
- Sacroiliac referred/related
- Bone stress injury, fracture or childhood bone conditions
- External iliac artery endofibrosis
- Neuralgia - femoral, obturator
JOINTS & BONES
- Lumbar joint structures - L3 - S1
- Sacroiliac joint referred
- Superior & inferior pubic rami
- Hip Joint - medial aspect
- Medial pole femoral head
SOFT TISSUES
- Ligamentum teres & pulvinar fat pad
- Pectineus
- Adductor brevis
- Adductor magnus
- Obturator externus
- Obturator internus & gemelli
- Femoral triangle with vascular structures
NERVES
- Lumbar nerve roots T12 – L2
- Femoral nerve
- Anterior femoral cutaneous nerve
- Possible overlap from inguinal, obturator & femoral branch of genitofemoral nerve
MID INGUINAL PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Hip joint related pain
- Labral tear (+/- Femoroacetabular Impingement Syndrome or Acetabular Dysplasia)
- Iliopsoas related pain
LESS COMMON DIAGNOSES
- Bone stress injury, fracture, or childhood bone conditions such as Perthes disease or Slipped Capital Femoral Epiphysis
- Neuralgia - femoral, obturator
JOINTS & BONES
- Lumbar joint structures - L3 - S1
- Hip joint
- Superior pubic ramus
- Acetabulum
- Femoral head/neck
SOFT TISSUES
- Iliopsoas - predominantly iliacus muscle belly
- Iliopsoas tendon
- Iliopectineal/psoas bursa
NERVES
- Lumbar nerve roots T12 – L2
- Femoral nerve
- femoral branch of genitofemoral nerve
- Possible overlap from anterior femoral cutaneous & inguinal nerves
ANTEROLATERAL HIP PAIN
COMMON DIAGNOSES
- Lumbar radicular or somatic pain
- Hip joint related pain
- Labral tear (+/- Femoroacetabular Impingement Syndrome or Acetabular Dysplasia)
- Rectus femoris tendinopathy
- ASIS/AIIS apophysitis
LESS COMMON DIAGNOSES
- ASIS/AIIS avulsion
- Subspine or AIIS Impingement
- Myofascial pain or injury of Rectus Femoris, Sartorius, TFL
- Bone Stress Injury or fracture
- Neuralgia - lateral femoral cutaneous nerve
JOINTS & BONES
- Lumbar joint structures - L3 - S1
- Hip joint
- Superior pubic ramus
- Acetabulum
- Anterior superior and anterior inferior iliac spines
- Femoral neck
SOFT TISSUES
- Sartorius
- Rectus femoris
- Iliocapsularis
- Tensor Fascia Lata (TFL)
- Anterior aspects of gluteus minimus and medius
NERVES
- Lx nerve roots T12 – L3
- Lateral femoral cutaneous nerve
- Possible overlap from inguinal, subcostal nerve or iliohypogastric nerves
Local Sources of Nociception, Referral and Common Diagnoses for Groin Pain
Groin pain has been one of those regions that has been plagued by multiple different diagnostic terms for the same conditions. This is confusing for patients, for health professionals in their inter-professional communication and makes it extremely difficult for researchers to bring together research in systematic reviews and meta-analyses. For this reason, an international consensus of experts agreed that diagnosis of groin pain should be simplified to 4 major conditions - adductor-related groin pain, pubic-related groin pain, inguinal-related groin pain and iliopsoas-related groin pain, with hip-related groin pain also recognised as a consideration in the differential diagnosis of groin pain. Iliopsoas and hip-related pain have been addressed in the anterior hip pain table above, so this table will focus on adductor, pubic and inguinal regions and what conditions, sources of nociception and referral should be considered for each region.
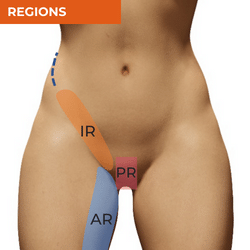
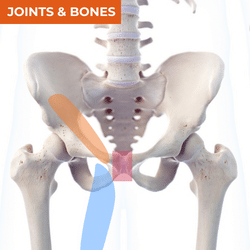
ADDUCTOR PAIN
COMMON DIAGNOSES
- Adductor Related Groin Pain
- adductor tendinopathy
- adductor myotendinous pain or injury
- adductor guarding
- Hip joint related pain
LESS COMMON DIAGNOSES
- Lumbar radicular or somatic pain
JOINTS & BONES
- Inferior pubic ramus
- Hip joint
- Lumbar joint structures - L3 - S1
SOFT TISSUES
- Adductor longus
- Adductor brevis
- Gracilis
- Pectineus
- Obturator externus
- Adductor magnus
NERVES
- Nerve roots T12-L3
- Ilioinguinal nerve
- Obturator nerve
PUBIC PAIN
COMMON DIAGNOSES
- Pubic related groin pain
- Pubic symphysis pain
- Pubic bone stress injury
- Pubic aponeurosis tear
- Pelvic girdle pain, pregnancy related pelvic girdle pain
LESS COMMON DIAGNOSES
- Neuralgia - iliohypogastric, genitofemoral, iliohypogastric
JOINTS & BONES
- Pubic symphysis
- Superior & inferior pubic rami
- Lumbar joint structures - L3 - S1
SOFT TISSUES
- Pubic disc
- Pubic aponeurosis - adductor-abdominal aponeurotic plate
- Inguinal ligament - medial
- Rectus abdominis
- Pyramidalis
- Levator Ani
NERVES
- Nerve roots T12-L2;S2-4
- Ilioinguinal nerves
- Iliohypogastric nerve
- Genitofemoral nerve
INGUINAL PAIN
COMMON DIAGNOSES
- Inguinal related groin pain
- Abdominal wall injury
- Inguinal ligament injury
- Inguinal hernia
- Iliopsoas related pain
- Hip joint related pain
LESS COMMON DIAGNOSES
- Lx radicular or somatic pain
- Neuralgia - local nerves
- External iliac artery endofibrosis
JOINTS & BONES
- Superior pubic ramus
- Lumbar joint structures - L3 - S1
SOFT TISSUES
- Inguinal ligament
- Abdominal muscles & their aponeuroses
- Transversus abdominis
- Internal & external obliques
- Rectus abdominis
- Deep & superficial inguinal rings
- Iliacus & psoas muscles & iliopsoas tendon
NERVES
- Nerve roots T12-L2
- Ilioinguinal nerve
- Transiting nerves
- Femoral nerve
- Iliohypogastric,
- Genitofemoral
ADDITIONAL SOURCES OF PAIN
Iliopsoas related groin pain has been included in the anterior hip pain table.
The tables on this page have highlighted the main musculoskeletal sources of hip, groin and buttock pain. Other causes of pain may include orthopaedic, neurological, rheumatological, urological, gastrointestinal, dermatological, oncological, or surgical conditions.

LEARNING RESOURCES
to Help you Master Differential Diagnosis of
ANTERIOR HIP & GROIN PAIN
Online Course
Includes 3 months access to 5 hours of online lectures
Downloadable PDF notes
Downloadable professional development certificate (upon completion of course)
Online Workshop
Includes 3 months access to 5 hours of online lectures & pdf handouts
+
2 x 3 hours of live zoom workshops with Dr Alison Grimaldi & 6 weeks access to workshop recordings
Face to Face Workshop
Includes 3 months access to 5 hours of online lectures & pdf handouts + 8 hours of practical workshop.
Brisbane only at this stage. International venues will resume as the pandemic allows
Hip Academy
Hip Academy: The Ultimate Learning Experience - Current membership includes ongoing access to:
- All Online Hip Courses
- eBook Series
- How-to Video Library
- PDF Resource Library
- Live Zoom Meetings
- Hip Academy Forum

Not a Health or Exercise Professional?
If you are not a health or exercise professional but someone with hip pain looking for answers, you might like to head over to Hip Pain Help.