Differential Diagnosis of Anterior Hip Pain – Nerve

Our exploration of differential diagnosis of anterior hip pain draws to a close this month. So far we've examined joint related anterior hip pain, bone related anterior hip pain, soft tissue related anterior hip pain and now finally this month, we take a look at nerve related anterior hip pain. While radicular pain and sciatic nerve related pain are well recognised in the differential diagnosis of buttock and posterior thigh pain, nerve structures are often overlooked as a source of symptoms at the anterior hip and thigh. Nature and behaviour of pain and patient history are key in recognising nerve related anterior hip pain.
Nerve Sources of Anterior Hip Pain
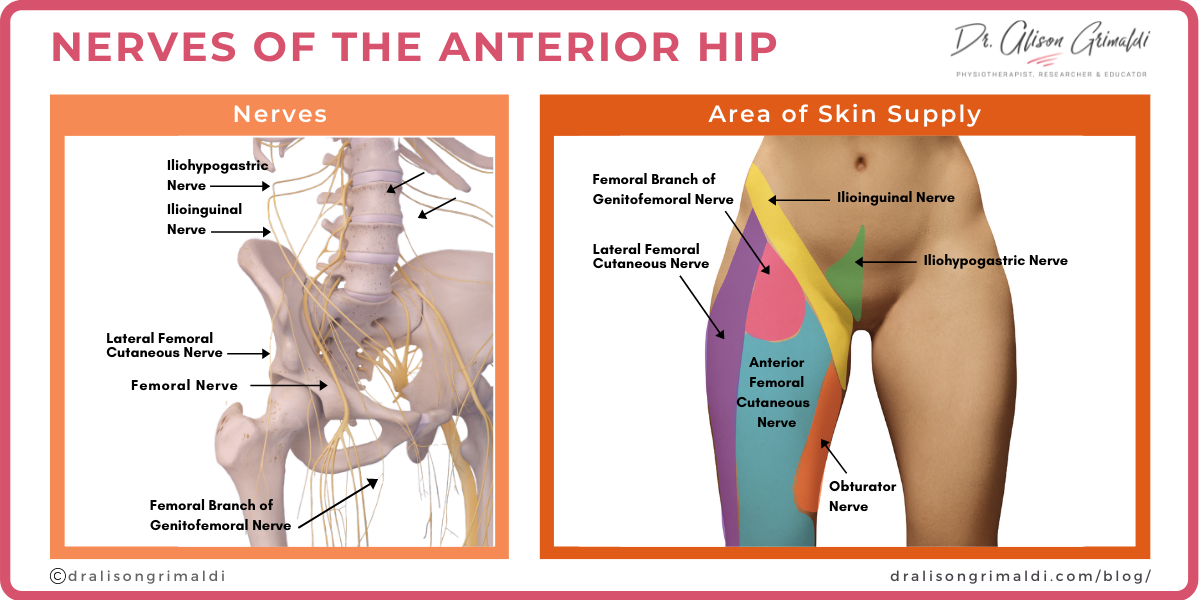
While the femoral nerve is the most familiar nerve of the anterior hip region, there are a number of other smaller nerves that transit and/or provide cutaneous innervation to the anterior hip. These include the ilioinguinal, genitofemoral and iliohypogastric nerves in the inguinal/anterior hip region, with the lateral and anterior femoral cutaneous nerves transiting through the hip and serving the lateral and anterior thigh respectively (see infographic below). Any of these nerves can be a source of local nociception or neuropathic pain.
Nerve related conditions associated with anterior hip pain
The nerves that serve the anterior hip and thigh can be responsible for nociceptive pain in the region of any local entrapment and/or neuropathic pain that extends to the area of nerve supply. Once leaving the spine, these nerves need to travel between or through paraspinal and abdominal muscles, the pelvis and then exit through or beneath ligamentous structures, before piercing the fascia to reach the skin. There are many sites of potential entrapment or irritation of these nerves along their pathways and mechanisms of injury that may be local or distant to the anterior hip region itself.
Possible entrapment or injury zones associated with nerve related anterior hip pain1,2
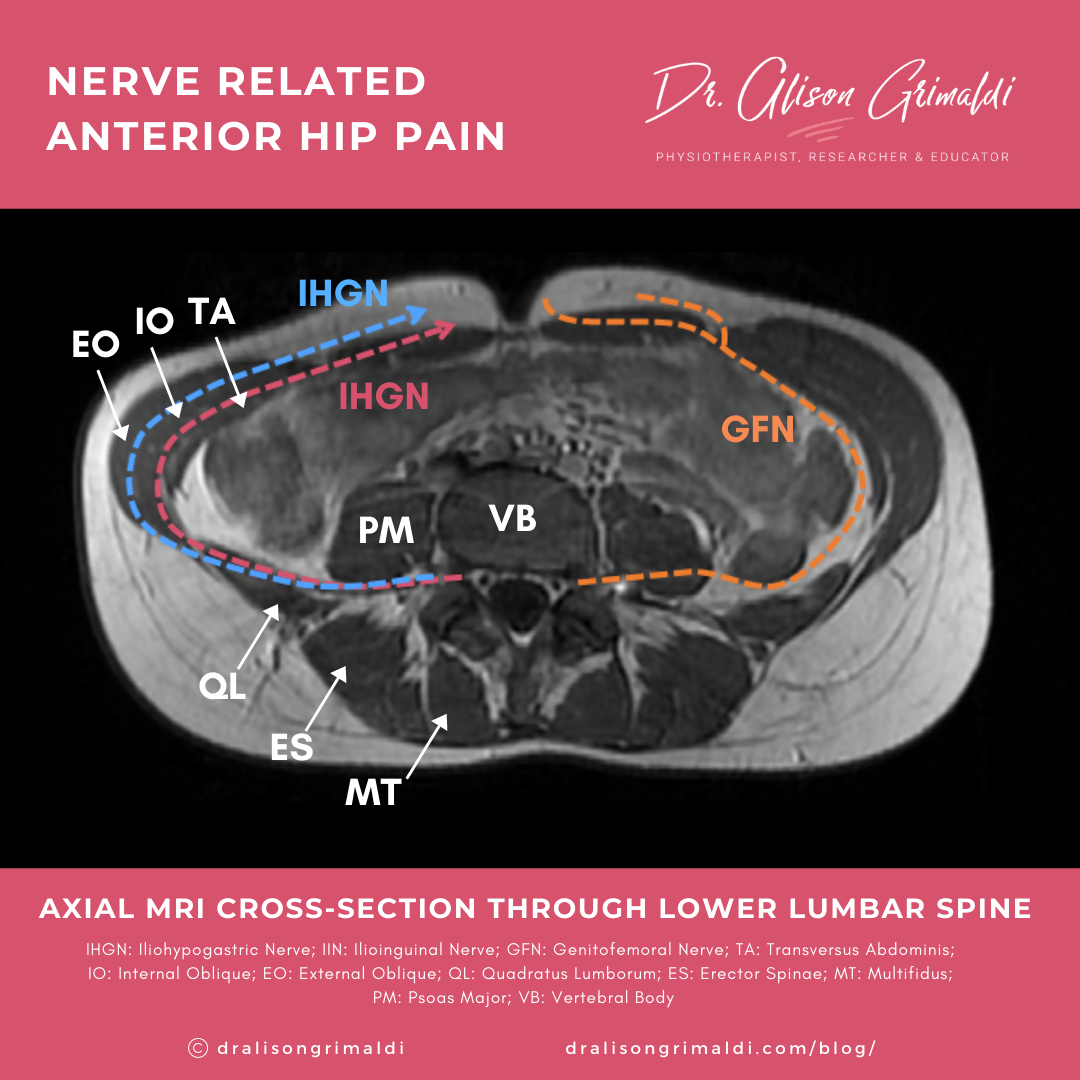
- Paraspinal region - The iliohypogastric and ilioinguinal nerves arise from T12 and L1 nerve roots and exit through or between the psoas major and the quadratus lumborum muscles, while the genitofemoral nerve, arising from L1 and 2, usually develops within the psoas muscle, exiting on its anterior surface.
- Through the abdominal wall - The iliohypogastric and ilioinguinal nerves enter the abdominal wall and travel between the layers of muscles to the anterior pelvis.
- Within the pelvis – The genitofemoral and femoral nerves transit from the upper lumbar region, through the pelvis to the inguinal region.
- Through the inguinal canal: The ilioinguinal nerve and the genital branch of the genitofemoral nerve travel along the inguinal canal.
- Exiting the pelvis: The femoral nerve and femoral branch of the genitofemoral nerve exit the pelvis beneath the inguinal ligament in the region of the femoral triangle. The lateral femoral cutaneous nerve exits the pelvis either underneath or through the lateral aspect of the inguinal ligament, just inside the anterior superior iliac spine.
Possible mechanisms for entrapment or injury of nerves supplying the anterior hip1,2,3
The most common mechanisms for entrapment or injuries related to nerve related anterior hip pain are iatrogenic mechanisms, indicating the importance of exploring any surgical history in the patient interview. Pregnancy, childbirth and endometriosis are also potential mechanisms in females. Trauma, and external compression are less common but possible mechanisms, and tumours and cysts should always be considered.
- Iatrogenic mechanisms
- Gynaecological surgery either due to direct injury or due to positioning – prolonged full hip flexion causing compression, or extremes of hip abduction and external rotation placing high tension on the inguinal ligament may impact on the nerves and/or their blood supply when sustained. Reports of femoral nerve injury related to a surgical assistant leaning on the femoral region also exist.
- Other abdominal wall incisions including appendectomy, hysterectomy, inguinal hernia repair, and caesarean section.
- Hip arthroscopy may result in direct injury to the lateral femoral cutaneous nerve in the placement of the portals or traction injury to the femoral nerve.
- Lumbar surgery, particularly anterior trans-psoas approach.
- Pregnancy and childbirth mechanisms may be related to pressure within the pelvis and during childbirth if the hips are sustained in stirrups (extreme hip abduction/external rotation) or full flexion for prolonged periods. Direct nerve injury or scar tissue entrapment may occur during/following caesarean section as mentioned above.
- Endometriosis may affect nerves transiting through the pelvis but endometriosis spread can be extensive, including through the inguinal canal, influencing those local nerves. Surgical excision of endometriosis also poses significant risks for direct injury or scar tissue entrapment of these nerves and subsequent nerve related anterior hip pain.
- Trauma or external compression may occur through a direct injury to the abdominal wall or anterior pelvis. External compression can also be imposed by tight clothing, belts or adiposity and associated abdominal overhang, compressing the inguinal ligament and associated nerves.
- Severe or prolonged muscle dysfunction or hypertonicity of the paraspinal or abdominal musculature may contribute to nerve related anterior hip pain.
- Tumours and cysts, usually within the pelvic cavity or the psoas muscle or bursa may lead to compression of adjacent nerves.
Features of nerve related anterior hip pain
- Area of pain:
- Area of nerve entrapment (nociceptive pain) and area of nerve supply (neuropathic pain). See infographic above outlining area of cutaneous innervation. Please note that the infographic provides typical distributions but there is much interindividual variability, with territorial overlap and lack of distinct territories.
- The femoral branch of the genitofemoral nerve serves the skin of the femoral triangle while the ilioinguinal and iliohypogastric nerves may give rise to symptoms in the inguinal and suprapubic regions.
- Injury or entrapment of the lateral femoral cutaneous nerve usually results in symptoms in the anterolateral thigh region – referred to as Meralgia Paraesthetica. It is also possible for patients to experience nociceptive pain in the most common area of entrapment – as it exits the pelvis just inside the Anterior Superior Iliac Spine.
- Femoral nerve symptoms are likely to arise in the areas of cutaneous innervation in the thigh.
- Extra-territorial spread of symptoms may occur due to remote immune-inflammatory responses in the dorsal root ganglia and dorsal horn.
- Nature of pain:
- Often described as burning with sharp or shooting pain
- Also, may experience an aching pain, often related with nociceptive stimuli at the region of entrapment
- Associated Symptoms:
- Dysaesthesia/paraesthesia – tingling, change in sensation, itching/crawling sensations, sensitivity to touch or temperature
- Weakness – Femoral nerve injury will result in weakness of the hip flexors and knee extensors, while the iliohypogastric and ilioinguinal nerves provide motor supply to the muscles of the abdominal wall.
- Aggravating Factors: This varies depending on the area and mechanism of nerve entrapment or irritation.
- Sitting – may be aggravating for any of these anterior nerves due to potential compression in hip flexion, particularly in lower seats/higher ranges of hip flexion.
- Hip extension and combinations of hip extension and abduction or rotation – for example end stance phase or changing direction while walking or running – these joint positions place tension on the nerve structures and/or the soft tissues through which they transit.
- Sustained or repetitive hip abduction/external rotation combinations – side lunges or stretching.
- Hip flexor, abdominal/trunk exercise or functional activity that loads these muscles, due to direct compression or traction on transiting nerves.
- Easing Factors:
- Getting up and moving – from sitting and at night.
- History of Onset:
- Ensure any history of surgery is explored.
- May have a history of abdominal or pelvic trauma.
- In females, consider pregnancy, childbirth, gynaecological procedures, endometriosis.
- Possible history of trunk or hip flexor muscle overload.
- Patient Characteristics:
- Variable.
- Presentation may be influenced by psychological stressors.
- Neuralgia more common in those with connective tissue disorders.
KEY IDENTIFIERS OF NERVE RELATED ANTERIOR HIP PAIN
Anterior hip pain is more likely to be related to peripheral nerves if:
- the patient reports burning, sharp or shooting pain and/or itching/crawling skin sensations
- pain is associated with paraesthesia or numbness
- pain is irritated by deep or sustained hip flexion, and/or
- pain is irritated by hip extension, abduction, external rotation and combinations of those actions
- pain response is often cumulative and delayed
- the patient has a history of abdominal, gynaecological or anterior approach lumbar surgery or hip arthroscopy
- the pain developed during/following pregnancy
- the patient has known endometriosis, or
- the patient has a history of trauma or overload of the abdominal wall, paraspinal muscles or inguinal soft tissues.
That concludes our series on differential diagnosis of anterior hip pain where we have explored sources, mechanisms and features of joint related anterior hip pain, bone related anterior hip pain, soft tissue related anterior hip pain and now peripheral nerve related anterior hip pain. Of course it is always important to consider somatic referral and radicular pain, so a full assessment should always include the lumbar spine and pelvis. And normal caution and questioning around red flags is always warranted.
Another great Anterior Hip Pain blog

Anterior Hip Pain: Causes & Contributing Factors
Adequate consideration of individual causes and contributing factors is important for best outcomes.
Sign up to our newsletter to receive updates on upcoming courses, news and special offers.
References
- Kale, A., Aytuluk, H., Aytuluk, H., Cam, I., Basol, G. and Sunnetci, B., 2018. Selective spinal nerve block in ilioinguinal, iliohypogastric and genitofemoral neuralgia. Turkish Neurosurgery, 29(4), pp 530-237.
- Elkins, N., Hunt, J. and Scott, K., 2017. Neurogenic Pelvic Pain. Physical Medicine and Rehabilitation Clinics of North America, 28(3), pp.551-569.
- Abdalmageed, O., Bedaiwy, M. and Falcone, T., 2017. Nerve Injuries in Gynecologic Laparoscopy. Journal of Minimally Invasive Gynecology, 24(1), pp.16-27.