Patient predictors of failed hip arthroscopy

How many times have you had a patient ask after their hip arthroscopy: ‘But the surgeon said my hip would be fixed, why do I still have pain?’ The literature tells us that while a majority of patients undergoing arthroscopy will gain benefit in terms of reduced pain and improved function, surgery for most is not a ‘cure’ that returns full painfree function.1,2 Education and setting realistic expectations preoperatively are key and should be the primary responsibility of the surgeon, with consistent information provided by the wider multidisciplinary team. In addition to those that improve but are disappointed in the limits to their recovery, there is another group who unfortunately experience no meaningful benefit1,2 (see the graphic below) and may have considerably worse pain following hip arthroscopy. There are many possible reasons for persistent hip pain following hip arthroscopy.3-6 In the next 2 blogs, I'll be exploring factors that have been reported to be predictors of failed hip arthroscopy. In this blog we'll cover patient predictors and next month we'll explore surgical and rehabilitation predictors of failed hip arthroscopy.
Discover our Anterior Hip & Groin Pain Course
If you enjoyed this blog, you might like to take the online course on Anterior Hip & Groin Pain - 5 hours of guided online video content. Better your skills and understanding of the anterior hip and groin and become equipped with the knowledge to administer clinical diagnostic tests and management strategies.
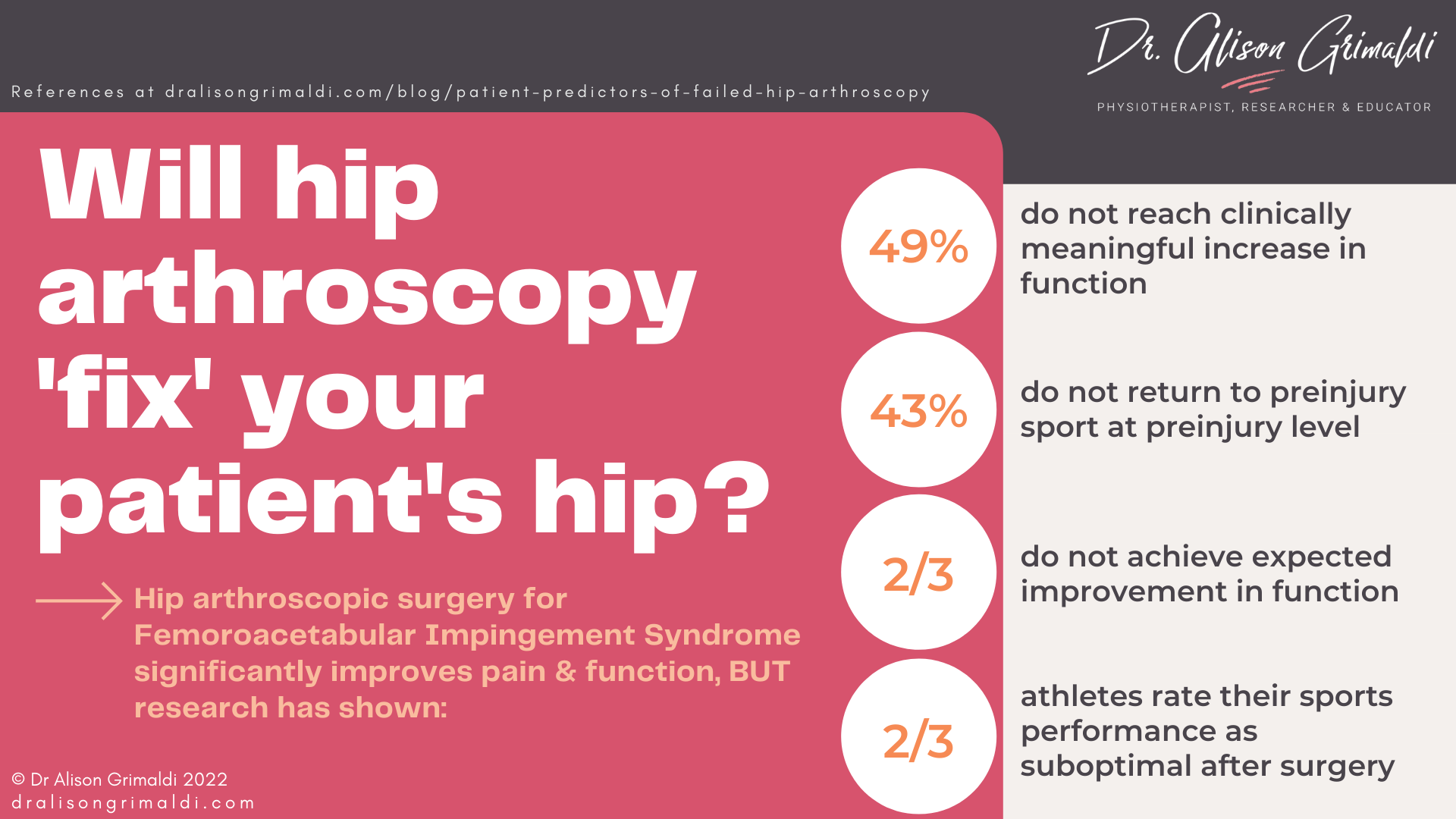
Patient selection factors that predict failed hip arthroscopy
Selecting patients who are likely to experience a positive benefit from hip arthroscopy is not an exact science, so an evaluation of relative risks and potential benefits is required. This responsibility falls primarily on the surgeon but remember when non-surgical health professionals refer a patient to a surgeon, it usually sends a message that non-surgical options have been exhausted. Therefore, it is important for non-surgical health professionals to be aware of the patient selection factors that make an individual a poorer or better candidate for surgery, prior to referral for a surgical consultation.
Wrong or incomplete diagnosis
The first and perhaps most obvious reason that a patient will fail to benefit from hip arthroscopy, is that the problem is not a hip joint related problem, or that the hip is not the primary issue.6 The main source of nociception may instead be extra-articular or remote. The lumbar spine is the most common remote source of referred hip pain. It is critical that a thorough differential diagnostic process is completed, and multiple sources are recognised when present. Patients with more complicated presentations may have co-morbid presentations of lumbar, intra-articular and extra-articular sources. Sometimes it is not possible to clearly determine the relative contributions of different sources, but treatment programs should ensure that each of these elements has been addressed as far as possible prior to any surgical intervention. The unknowns regarding surgical outcome should also be discussed with the patient within an informed, shared-decision-making process.
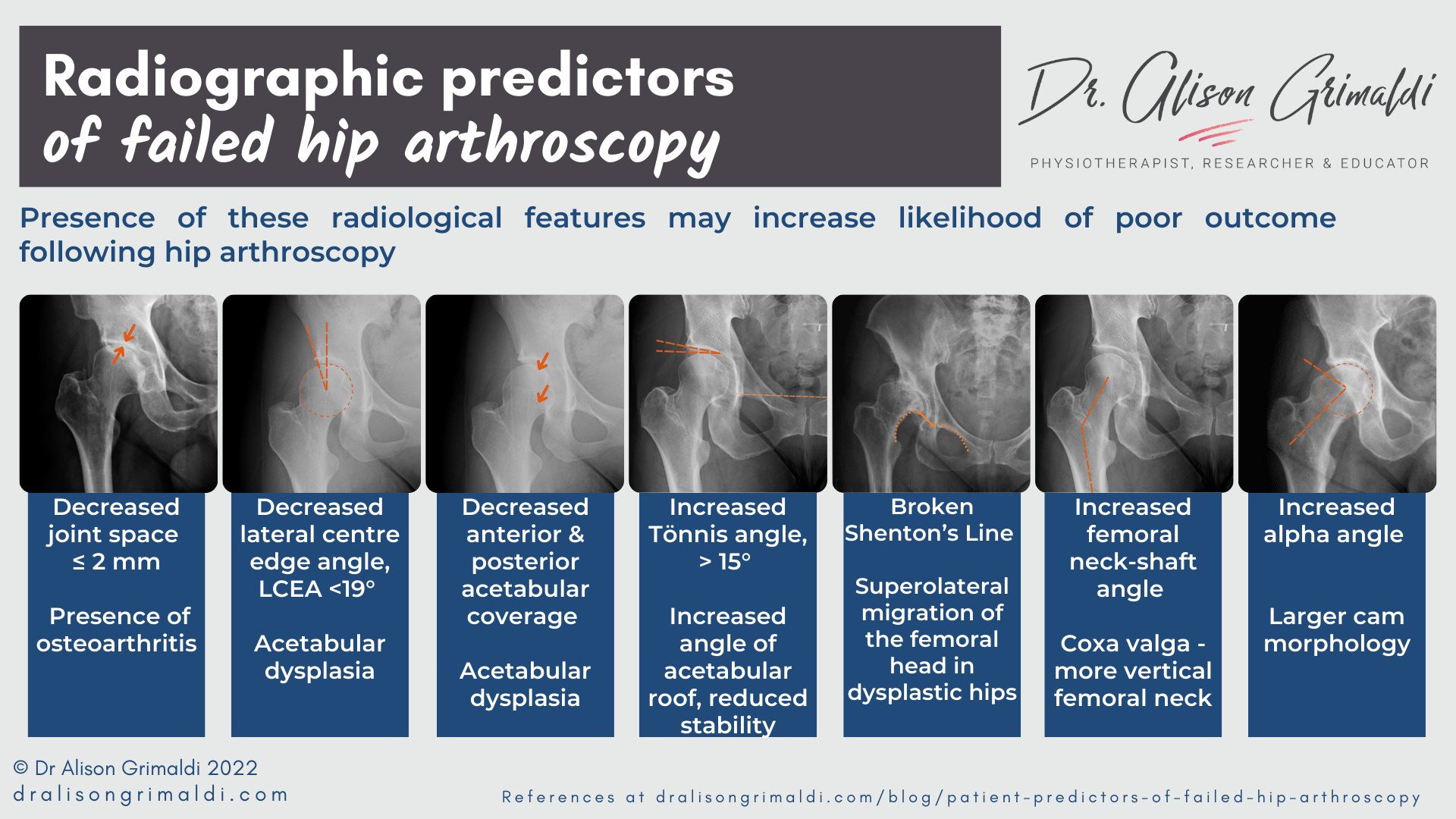
Radiographic predictors of failed hip arthroscopy
There is now a growing body of evidence around radiological signs that are more likely to result in failed hip arthroscopy. These are patients that just don’t do well after arthroscopy as their joint is too compromised to benefit adequately from an arthroscopic procedure.
Radiographic predictors of failed hip arthroscopy include:3
- decreased lateral centre edge angle (LCEA <19°, acetabular dysplasia)
- increased Tönnis angle (> 15°, increased angle of acetabular roof, reduced stability)
- broken Shenton’s Line (superolateral migration of the femoral head in dysplastic hips)
- increased alpha angle (larger cam morphology)
- decreased joint space (≤ 2 mm, indicating osteoarthritis)
- increased femoral neck-shaft angle (coxa valga - more vertical neck)
- decreased anterior and posterior acetabular coverage (acetabular dysplasia).
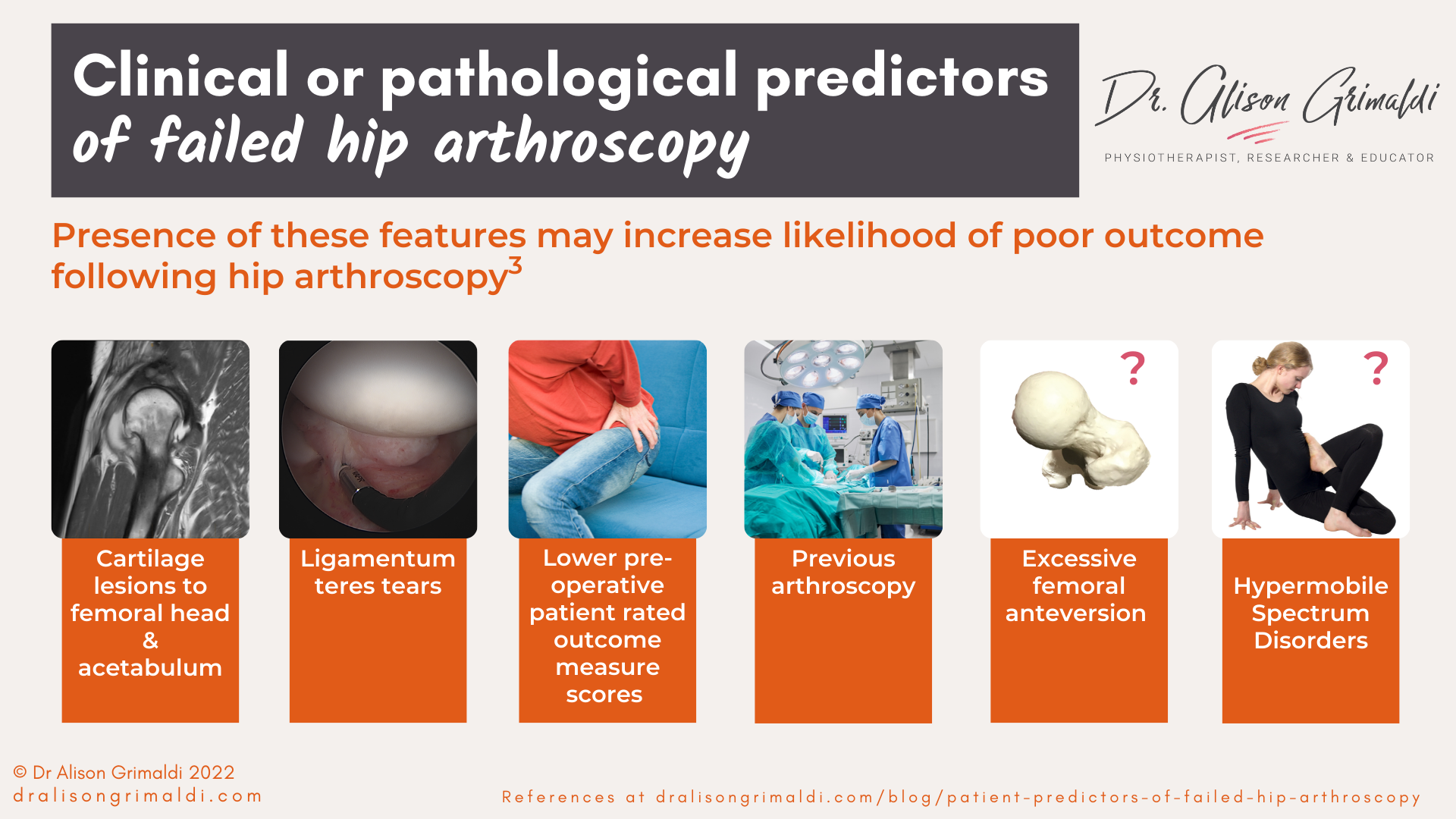
Clinical or pathological predictors of persistent pain after hip arthroscopy
In addition to the radiological predictors, other indicators of advanced joint disease or greater clinical severity have been linked to poorer outcomes and persistent pain following arthroscopy.
Clinical or pathological predictors of failed hip arthroscopy include:
- cartilage lesions to femoral head and acetabulum3
- ligamentum teres tears3
- lower pre-operative patient rated outcome measure scores (WOMAC/mHHS/HOS-ADL)3
- previous arthroscopy3
- femoral anteversion – possible
- hypermobility – possible
Cartilage lesions to the anterior acetabulum and posterior femoral head have been shown to independently predict conversion to total hip arthroplasty following arthroscopy.3 Damage to the femoral head cartilage is often a sign of more advanced degenerative joint disease. Ligamentum teres tears have been associated with poorer outcomes following arthroscopy.7 This may be due to deficient stability and greater translational forces within the hip joint or simply another sign of more advanced joint disease.
At a minimum of 2 years after hip arthroscopy for FAIS,
- those with a complete Ligamentum Teres tear were 3 x more likely to require total hip arthroplasty (replacement)
- almost 30% had converted to total hip arthroplasty.7
Those with greater clinical severity as indicated by lower pre-operative patient rated measures of disability (WOMAC, modified Harris Hip Score, Hip Outcome Score-ADL subscale), also fare more poorly after hip arthroscopy. The reasons for this are likely to be multifactorial. Lower scores in some cases are associated with greater pathology but are often more closely linked with physical impairments (e.g., muscle weakness, reduced physical capacity) or psychological factors (e.g., fear, reduced self-efficacy, catastrophisation, anxiety, depression or low expectations).4
It is also well acknowledged that outcomes of subsequent arthroscopies are on average poorer than what can be expected after an index procedure. Those undergoing repeat arthroscopy have already had a failed procedure, with the chances of success of a subsequent procedure significantly reduced.5
Two other clinical factors that have been suggested but not well established at this point are femoral anteversion and ligamentous laxity or hypermobility spectrum disorders. Increased joint loads imposed by both of these factors may impact on outcomes following arthroscopy. One study reported inferior outcomes after arthroscopy for patients with generalised ligamentous laxity, unless careful capsular management was performed.6
Demographic predictors of poor outcome after hip arthroscopy
There are other patient factors, not directly related to joint pathology or morphology, that can influence outcome of hip arthroscopy.
Demographic predictors of failed hip arthroscopy include:3
- increased Body Mass Index (BMI)
- increased age,
- male gender, or
- young, thin females.
Not surprisingly, older individuals and those with higher BMI are less likely to gain benefit from hip arthroscopy. Two groups – older overweight males (BMI >25) and young, thin females in the context of mild-moderate dysplasia – are more likely to experience failed arthroscopy.3
Age alone has a significant impact on conversion rate to arthroplasty. A systematic review of outcomes in patients aged 40 years or more reported that the rate of conversion to total hip arthroplasty (hip replacement surgery) was 18.1% for patients aged 40 years or older, 23.1% for patients older than 50 years, and 25.2% for patients older than 60 years, with a mean time to arthroplasty of 25.0 months.8
Prior to arthroscopic surgery, both surgeons and non-surgical health professionals should carefully evaluate the individual and determine if there are patient predictors that increase the chances of a poor outcome. If so, a more prolonged and perhaps optimised course on non-surgical management may be warranted. Join me next month to explore surgical and rehabilitation predictors that may help provide some explanation for failed hip arthroscopies.
If you are keen to hear more about rehabilitation considerations for hip arthroscopy, you might like to join me at our upcoming Hip Academy meeting.
TOPIC: Rehabilitation Considerations for Hip Arthroscopy - APRIL 28th
Rehabilitation Considerations for Hip Arthroscopy. I stepped through
- Factors that influence outcomes of hip arthroscopy,
- Considerations for early & advanced rehab, and
- Optimising outcomes for your patients post hip arthroscopy.
For non-members, if you'd like to review this lecture and join us for future meetings, Join Hip Academy below.
Another great Anterior Hip Pain blog

Anterior Hip Pain: Causes & Contributing Factors
Adequate consideration of individual causes and contributing factors is important for best outcomes.
References
- Palmer AJR, Ayyar Gupta V, Fernquest S, et al; FAIT Study Group. Arthroscopic hip surgery compared with physiotherapy and activity modification for the treatment of symptomatic femoroacetabular impingement: multicentre randomised controlled trial. BMJ. 2019 Feb 7;364:l185.
- Ishøi L, Thorborg K, Kraemer O, Hölmich P. Return to Sport and Performance After Hip Arthroscopy for Femoroacetabular Impingement in 18- to 30-Year-Old Athletes: A Cross-sectional Cohort Study of 189 Athletes. Am J Sports Med. 2018 Sep;46(11):2578-2587.
- Shah A, Kay J, Memon M, Simunovic N, Uchida S, Bonin N, Ayeni OR. Clinical and radiographic predictors of failed hip arthroscopy in the management of dysplasia: a systematic review and proposal for classification. Knee Surg Sports Traumatol Arthrosc. 2020 Apr;28(4):1296-1310.
- Shin JJ, de Sa DL, Burnham JM, Mauro CS. Refractory pain following hip arthroscopy: evaluation and management. J Hip Preserv Surg. 2018 Jan 18;5(1):3-14.
- Shapira J, Kyin C, Go C, Rosinsky PJ, Maldonado DR, Lall AC, Domb BG. Indications and Outcomes of Secondary Hip Procedures After Failed Hip Arthroscopy: A Systematic Review. Arthroscopy. 2020 Jul;36(7):1992-2007.
- Makhni EC, Ramkumar PN, Cvetanovich G, Nho SJ. Approach to the patient with failed hip arthroscopy for labral tears and femoroacetabular impingement. J Am Acad Orthop Surg. 2020 Jul 1;28(13):538-545.
- Maldonado DR, Laseter JR, Perets I, Ortiz-Declet V, Chen AW, Lall AC, Domb BG. The effect of complete tearing of the ligamentum teres in patients undergoing primary hip arthroscopy for femoroacetabular impingement and labral tears: a match-controlled study. Arthroscopy. 2019 Jan;35(1):80-88.
- Horner NS, Ekhtiari S, Simunovic N, Safran MR, Philippon MJ, Ayeni OR. Hip arthroscopy in patients age 40 or older: a systematic review. Arthroscopy. 2017 Feb;33(2):464-475.e3.


