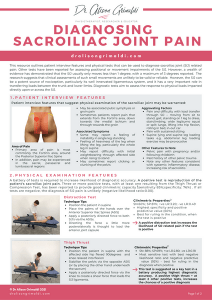
Sacroiliac joint related pain
The role the sacroiliac joint plays in posterior pelvic pain presentations has been a topic of contention for at least the last 10 years. There are still firm believers that pelvic asymmetry, malalignment or movement dysfunction drives all pelvic pain and should be the primary focus of intervention. On the other hand, some have decided that a joint that moves this little is irrelevant and do not even consider the sacroiliac joint in a differential diagnosis of posterior pelvic pain. At both ends of this spectrum of clinical bias, there may be adverse consequences – patients may develop harmful beliefs with long-lasting effects or suffer for much longer than necessary due to misdiagnosis.
My stimulus for writing about sacroiliac joint related pain this month, was the opportunity that arose recently to experience this pain again first-hand – not of course sought after or welcomed, but always a great learning experience! It was January the 2nd and my children and I decided to take a hike up Tabletop mountain – an extinct volcano near Toowoomba. We chose the Grade 5 hiking trail, which really ended up a scrabbling climb rather than a hike (some of you who live in Toowoomba or have visited the area might know the track).
Can't make the workshop? Do the Online Course

The views were completely worth the climb, as you can see above, but coming back down again was pretty precarious – rock hopping across the unstable watershed of basalt rubble that was once a lava stream. As gravity dictates, if you slip while walking down a 45° slope, you are most likely to fall backwards and unfortunately that is just what happened – and there was no soft landing! The force was absorbed by my sacrum on a sizeable, pointed rock that happened to be very firmly fixed in the ground beneath.
Ouch!!


The first interesting thing in what followed, was the immediate recall of past events and implications for anticipated consequences. I had taken a fall onto my sacrum at around 16 years of age (a long time ago now!) and had great difficulty walking and sitting for about 6-8 weeks. Imaging in my 20’s had revealed that I had in fact fractured my sacrum in that fall. As I lay there for a moment, my helpful brain decided it was a great time to drag this information from my memory centres, together with professional exposure to similar patient experiences, and force me to consider the possible consequences of this event. I reassured my helpful ‘protectometer1'and my 3 stunned teenage children, that I would be ok, rolled onto my side and struggled to my feet with a little assistance. After testing my ability to ambulate, which was certainly hampered, my brain turned its attention to exactly how I was getting back to the car. This involved not only making it to the bottom of this slippery volcano, but there was a second sharp rocky climb and descent to negotiate as well. At this point my helpful brain reminded me of the reviews we’d read about this climb before embarking – emergency services rescues were not uncommon, and I could now see why! I thanked my ‘protectometer’ for the timely reminder and determined that that would not be my story. The return journey was a slow one and then the next challenge was the car trip. Lucky we now have two other drivers in the family but sitting in a car while trying to avoid painful contact between the seat and the sacrum is interesting!
Bruising over the sacrum came out within a couple of days and the region of pain and functional difficulty suggested the primary trauma was localised to the left sacroiliac joint (SIJ). There was certainly pain in the typical Fortin’s area2, but as my patients have often reported, the pain extended in a string-line fashion from the posterior superior iliac spine, towards the medial ischium and through to the ipsilateral pubic symphysis. This was primarily evident with movement and likely reflected the trauma-induced mechanosensitivity of the broad network of pelvic ligaments.
Pain was primarily with loading of the left sacroiliac joint or direct contact with the sacrum, in sitting or supine lying. While radiostereometric analysis of SIJ movement has reported less than 2° of motion in all planes3, it has an incredibly important role in load transmission between the trunk and lower limbs. A lack of appreciable movement does not mean a lack of appreciable load. Full credit to this amazing flat joint that absorbs and transfers such large loads and yet moves so little! When the ligaments of the regions are sensitised, it’s pretty easy to tell when they are loaded!
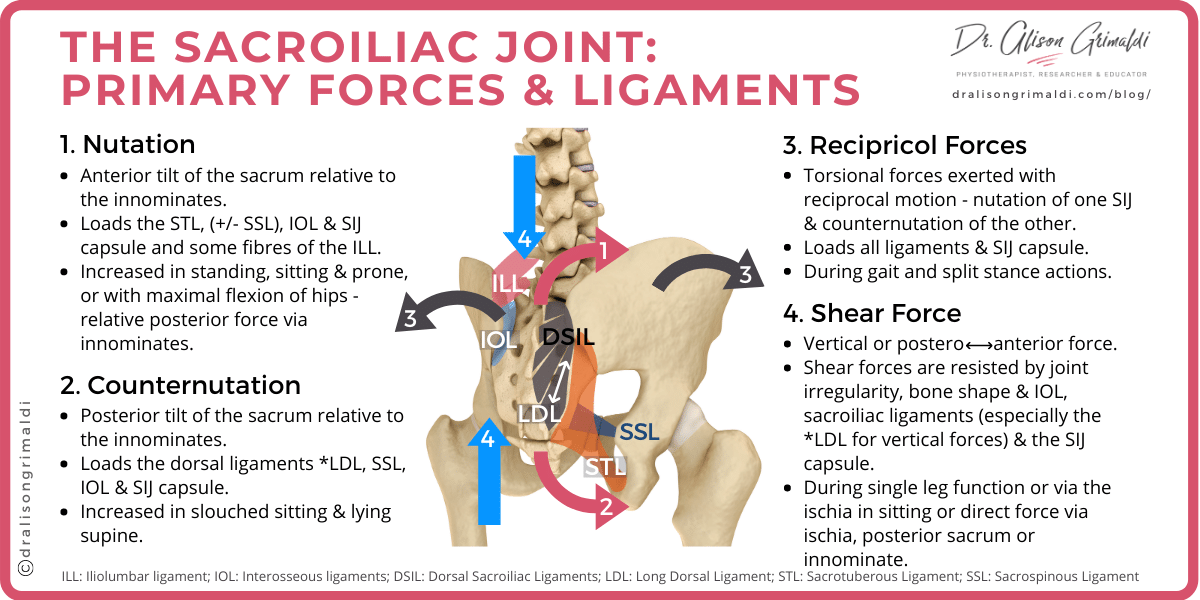
Forces that load the sacroiliac joint
1. Nutation forces acting on the sacroiliac joint
A nutation force is one in which the sacrum is encouraged to tilt anteriorly relative to the ilia or innominates (see infographic above). The axis for nutation and counternutation is a transverse axis around the body of S2. A forward tilt of the promontory (top) of the sacrum will be resisted by ligaments that constrain a posterior movement of the lower sacrum. The sacrotuberous ligament is a major constraint to sacral nutation4. Earlier studies suggest that the sacrospinous ligament will also resist nutation, although a more recent investigation argues that it's structure suggests it is more likely to assist in controlling counternutation5. The strong interosseous ligaments and sacroiliac joint capsule will also assist in controlling any torsional load crossing the sacroiliac joint. Some fibres of the iliolumbar ligament are also likely to assist in controlling these forces.
Sacroiliac joint pain associated with nutation forces
Nutation loads occur in positions of lordosis, such as in standing, upright sitting and in prone. These loads will be higher with hypervigiliant postures or movement patterns that use forced, excessive lumbar lordosis.
Nutation forces will also be induced by movement of the innominates on the sacrum. Bilateral flexion of the hips - for example pulling the knees to the chest - will induce a nutation force due to the posterior rotation force at the innominates and therefore relative anterior tilt force at the sacrum. Similarly, standing and leaning forward will induce a nutation load as the hamstrings constrain the movement of the innominates by holding firm on the ischia.
Standing forward lean/bending was certainly a challenge for me in the first couple of weeks post injury. In these positions, the nutation loads are high due to the effect of the centre of mass of the trunk. In upright standing, the mass of the trunk is sitting fairly vertically above the SIJ, so the lever arm in the sagittal plane is relatively small. However, when standing and leaning or bending forward, the centre of mass of the trunk is well forward of the sacroiliac joint centres, imposing much greater loads. Furthermore, the hamstrings play a very active role in load transfer and are not simply acting as an anchor for the ischium. The fibrous connection between the proximal hamstring tendons and the sacrotuberous ligament6, means that the stronger the force generated by the hamstrings, the greater the load that is transferred via the sacrotuberous ligament and across the dorsal sacroiliac complex. When standing in forward leaning, the hamstrings are working hard to support the high load of the trunk, with all that force transferred through the sacroiliac region. This is completely normal of course and not dangerous, but if the region is sensitised, pain may be experienced. Similarly, the multifidus and erector spinae influence loads crossing the sacroiliac joint. Spasm or hypervigilant behaviours may also amplify nutation forces and nociception from sacroiliac ligamentous structures.
2. Counternutation forces acting on the sacroiliac joint
Counternutation forces are those which encourage posterior tilt of the sacrum on the innominates - the sacral promontory forced posteriorly and the lower sacrum pushed forward (refer to infographic above). The long dorsal ligament running vertically from the posterior superior iliac spine (PSIS) down onto the sacrum, is a major constraint to sacral counternutation7 with the sacrospinous ligament reported to assist.5Again, the interosseous ligaments and capsule will also be loaded.
Sacroiliac pain associated with counternutation forces
Counternutation generally occurs in supine and in more flexed sitting positions. Supine lying can often be provocative for those with sacroiliac joint pain. This may be a combination of direct contact with sensitised structures, counternutation forces and even potentially some posteroanterior sheer force - like that imposed by a sacral thrust diagnostic test. So, even if you have determined that your patient may benefit from some abdominal conditioning, supine leg loading exercises may not be the best choice if they are reporting discomfort in this position and pain aggravation following supine exercises.
In sitting, lumbopelvic and sacral aching may be due in some cases to excessive, sustained counternutation loads on interosseus and long dorsal ligaments. Ideally, a relaxed supported sitting position that avoids both excessive nutation and counternutation forces is usually most comfortable for those with sacroiliac joint related pain.
3. Recipricol forces acting on the sacroiliac joint
The challenge to the sacroiliac joint ligaments can be even higher when different forces are imposed on the left and right joints. For example, if the left innominate is being forced into posterior rotation and the right innominate into anterior rotation, the sacroiliac joints need to absorb opposing forces - nutation and counternutation respectively.
Sacroiliac joint pain associated with reciprocal forces
The most obvious exposure to such forces is during gait where reciprocal lower limb movement drives torsional forces across the sacroiliac joints - posterior rotation of the innominate of the front leg and anterior rotation of the innominate of the back leg, which then reverses with each step. My post-trauma sensitised system obviously decided it would attempt to absolutely minimise such forces, leaving me feeling like my sacrum was clamped very firmly between the ilia. I called this my 'wooden pelvis'. Interestingly, the result was similar to the gait alterations commonly employed by those with anterior hip pain - in an attempt to avoid hip extension, lumbopelvic axial rotation may increase. So my system evidently decided it was less load (and therefore pain) to minimise sagittal plane loads and substitute with axial plane rotation of the pelvis as a block. The nervous system is an amazing thing!
Asymmetrical/reciprocal loading in other situations can also be challenging for those with sacroiliac joint pain - for example, split lunge type positions - amplified in something like a rear foot-elevated split lunge (Bulgarian split lunge) where the highly active extensors of the front hip and the flexors of the back hip create opposing forces across the pelvis.
4. Shear force acting on the sacroiliac joint
As a vertically oriented planar joint, the SIJ needs to resist significant shear force imposed by gravity in upright positions. The irregular joint surfaces, wedge shape of the sacrum and strong ligamentous system provide form closure, while myofascial forces provide force closure, together resisting shear forces6. Standing loads are greater than sitting, and standing on one leg requires a single sacroiliac joint to absorb all the shear force imposed by the load of the trunk, pelvis and other lower limb. Dynamic landing on one leg, will amplify these forces further.
Sacroiliac joint pain associated with shear forces
Standing and sitting may be painful for those with sacroiliac joint related pain, and difficulty with standing on one leg is a very common issue.
In my case, similar to many descriptions of prior patients, standing on one leg to dress was one of the most painful and functionally challenging tasks in the presence of sacroiliac joint related pain.
This is not of course simply about the shear force of standing on one leg, but the combined effect of:
- shear force,
- nutation force,
- muscle forces as everything works to maintain single leg balance and suspend the weight of the trunk, and
- coping with the dynamic and variable force of the other lower limb moving into hip flexion or flexion/abduction/external rotation to dress.
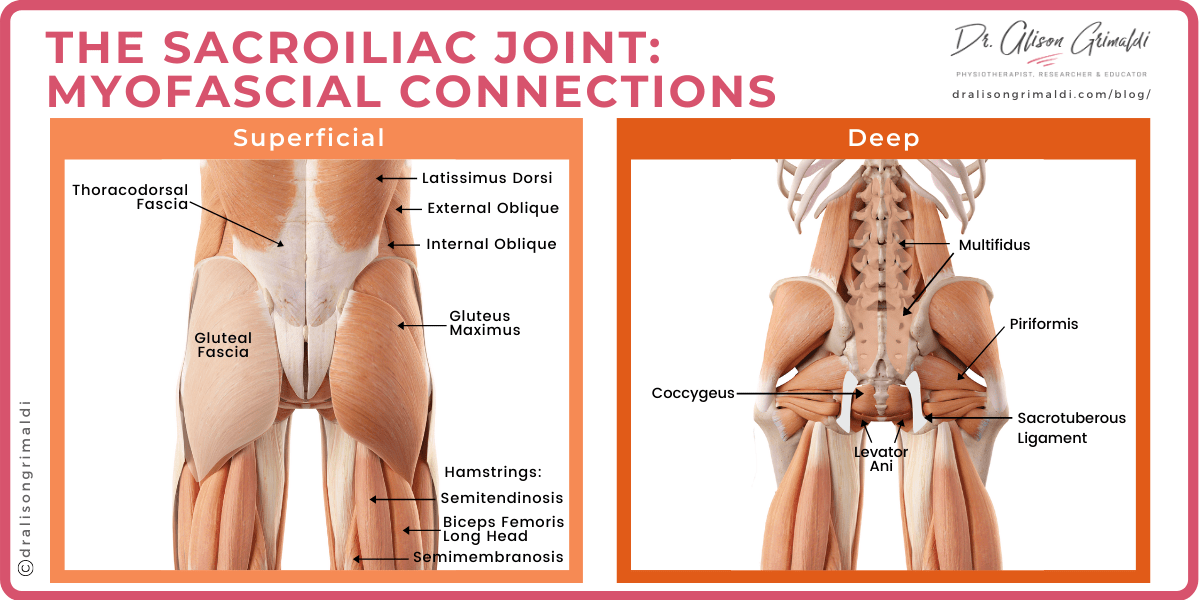
5. Muscle forces acting across the sacroiliac joint
As already mentioned, while muscles support and assist with load transfer across the sacroiliac joints, they largely accomplish this by controlling the trunk and hip levers and creating tension across the ligamentous system surrounding the sacroiliac joints.
Sacroiliac joint pain associated with muscle forces
Not surprisingly then, muscles pulling on sensitised ligaments may result in pain. Nociceptors in the interosseus ligaments and subchondral bone may also be stimulated by compressive loads exerted by the confluence of the thoracodorsal fascia, gluteal fascia and connecting latissimus dorsi, trunk and hip extensors and the lateral abdominals6(see graphic above). Other muscles such as the piriformis, coccygeus, levator ani and iliacus have more local connections with the sacroiliac ligaments and capsule. Muscle spasm or active contraction may amplify the nociceptive response to the forces discussed above. You might be surprised at the influence of even a gentle pelvic floor contraction - I was!
In at attempt to start with some gentle symmetrical movement, I was doing some 4 point kneeling exercise - pelvic tilting and rock-backs. Initially this was met with high levels of pain extending from the ischium, to the PSIS and then into the lumbar erector spinae - this was worst with a combination of rocking back and actively posterior pelvic tilting. It was not simply the nutation force and tension created by protective trunk extensors, but the natural activity of the lateral abdominals and pelvic floor during an active posterior tilt. Experimenting with this phenomenon, I was surprised at the dramatic increase in pain created by consciously working the pelvic floor a little harder. Of course, I backed off and worked within a reasonable level of discomfort until things started to ease, aiming to normalise my response to movement and tolerance of normal sacroiliac forces.
I'll leave you with these thoughts:
- Have function and load tolerance at the forefront when providing advice and developing an exercise program for sacroiliac joint pain.
- Asking patients to consciously tighten muscles harder to provide better strength gains and/or joint stability, may be provocative.
- Reflect on whether the pain and disability associated with sacroiliac joint pain for the patient in front of you is about joint malalignment and/or stability, or simply about load transfer and load tolerance.
- Listen to patient's response to movement, understand the loads (both physical and psychological - e.g. fear and beliefs about frailty) and aim to re-expose the system to gradually more challenging tasks.
P.S. In case you were wondering - After my own graduated loading program, I'm pretty much painfree now, wooden pelvis gone!
This month, a new SIJ clinician resource has been added to the growing library of pdf resources available for Hip Academy members.
Hip Academy Members - Log in & Download your Free Copy!
6 new diagnostic test videos are also now available for Hip Academy & Video Library Members
Easy-access reference videos to help you with diagnosing sacroiliac joint related pain:
- Sacral Thrust
- Distraction Test
- Thigh Thrust
- Compression Test
- Gaenslen's Test
- FABER Test for SIJ