Cam Morphology: Development and Prevention
Cam morphology is an aspherical femoral head, where extra bone at the femoral head-neck junction may cause damage to the acetabular labrum and rim cartilage, as the large bony bump is forced into the hip socket. This bony shape is a significant risk factor for the development of Femoracetabular Impingement (FAI – early impingement of the head-neck region with the acetabular rim), hip pain (Femoroacetabular Impingement Syndrome – FAIS) and osteoarthritis.1 It is no surprise then, that understanding development and prevention of cam morphology is of key importance.
Surgical interventions aim to trim the extra bone to restore function and reduce the chances of developing hip osteoarthritis. Such interventions do not provide a complete solution, with residual symptoms and disability common after surgery,2,3,4 and no clear evidence to date that surgery can prevent hip OA associated with this bony variant.
Therefore, researchers have been hard at work trying to understand cam morphology of the hip and answer 2 key questions:
- Why does cam morphology develop? and
- Can we prevent the development of cam morphology?
After all, prevention wherever possible, usually provides a much better outcome than a ‘cure’.
Join me in exploring the evidence around development and prevention of cam morphology.
These are the main topics:
- Factors linked to cam development – Who is more likely to develop cam morphology?
- Age and skeletal maturity
- Sex
- Activity levels
- Type of Sport
- Pathogenesis of cam morphology – Why does cam morphology develop?
- Is cam morphology a subtle slipped epiphysis?
- Changes in growth plate orientation
- What causes lateral epiphyseal extension?
- Links between inflammation and cam morphology
- Preventing development of cam morphology - How do we prevent it?
- Reducing exposure to hip-heavy sports to reduce load on the femoral growth plate
- Considerations for hip-heavy strength training in adolescents
- Screening for early intervention
Factors linked to the development of cam morphology – Who is more likely to develop cam morphology?
Age and skeletal maturity: Cam morphology develops during adolescence
The clearest factors associated with cam development are age and skeletal maturity – whether the physis (growth plate) is open or closed. It is now well accepted that cam morphology develops primarily during adolescence, when the growth plate is open.5,6,7,8
A number of studies have tracked changes in various bony indices linked with cam morphology, most commonly a change in alpha angle. Alpha angle is the angle between a line from the centre of the femoral head through the middle of the femoral neck and a line that crosses the point at which the bone of the head of the femur leaves the circular constraints of a typical femoral head (see infographic below). A normal alpha angle is usually described as less than 60°, although some researchers have defined cam morphology as less than 55°.
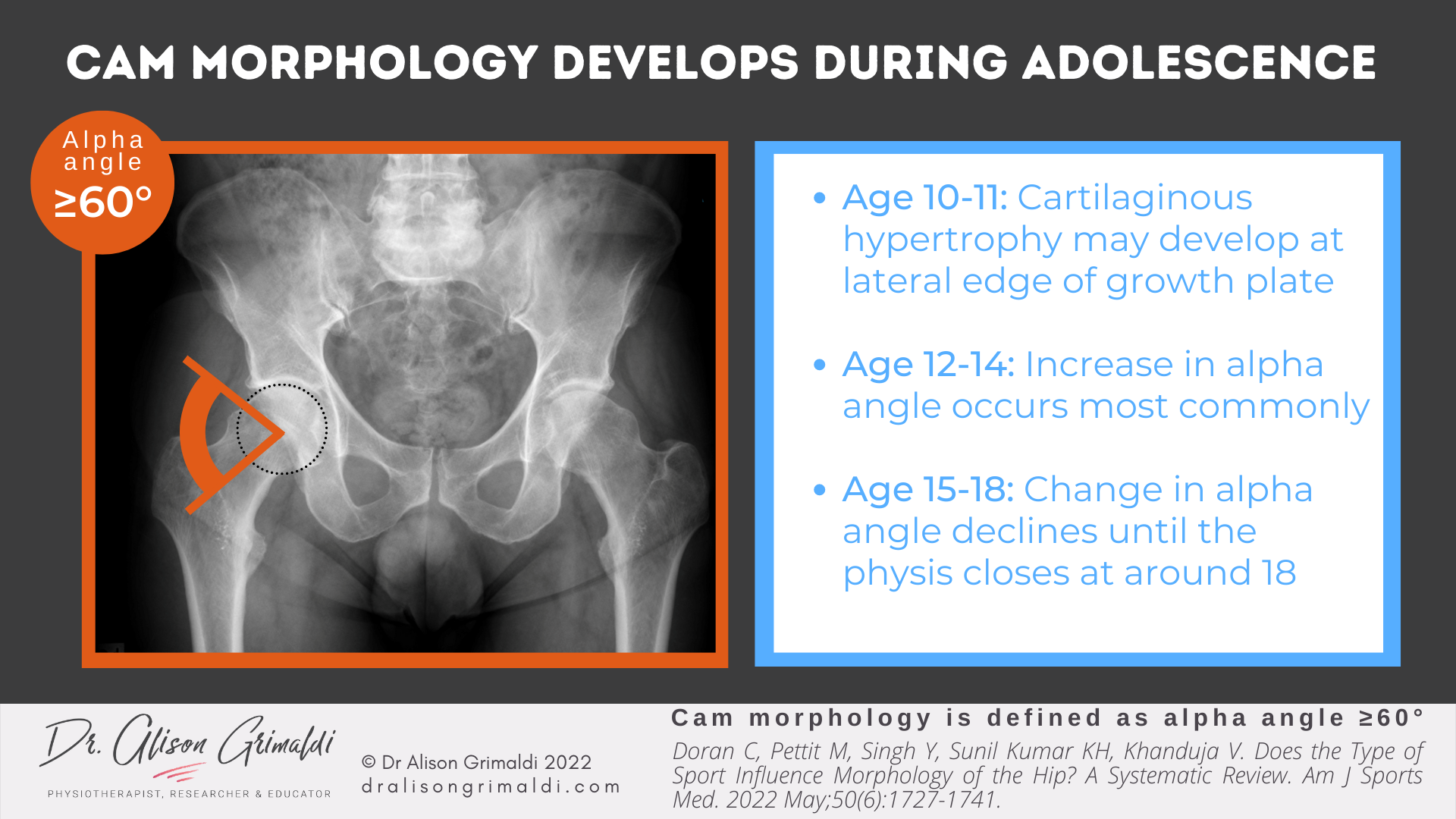
An increase in alpha angle has been shown to occur most commonly between 12 and 14 years of age, with change in the alpha angle declining until the physis closes at around 18 years of age. This early adolescent phase is likely to reflect a period of peak bone growth, which tends to be highest at around 14 years of age for males.9,10 While the earliest change in bone shape is usually around 12 years,5,6,7 Palmer et al. (2018) reported that cartilaginous hypertrophy at age 10-11 precedes the bone change visible on X-rays.8
Sex: Cam morphology is more common in males
There is a clear predisposition in males for the development of cam morphology. While 13 -72% of asymptomatic males develop cam morphology, only 0-11% of asymptomatic females develop this femoral shape.11 Fernquest and colleagues reported that males had a significantly greater change in alpha angle than female school children over the course of a 3-year longitudinal study of adolescents.12
Activity levels: Cam morphology is more common in active individuals
A recent systematic review of studies to date found a significant positive correlation between activity level and both alpha angle and prevalence of cam-type FAI. Higher activity levels were linked with greater alpha angles and higher prevalence of FAI.13
Cam morphology and activity levels using the Physical Activity Questionnaire
A commonly used tool for measuring physical activity is the 5-point Physical Activity Questionnaire (PAQ). A score of 1 indicates low physical activity, and a score closer to 5 indicates high physical activity.
Fernquest and colleagues (2021) reported that adolescent footballers with high activity levels had significantly greater change in alpha angle than those with lower activity levels.12 With adjustments made for age and gender, they reported:
- athletes with a PAQ score between 3 and 4 had an average change in alpha angle of 0.58° greater than those with a PAQ < 2.
- athletes with a PAQ score between 4 and 5 had an average change in alpha angle of 3.20° greater than those with a PAQ < 2.
- individuals with a PAQ score above 3 were at significantly elevated risk of developing cam morphology.
Cam morphology and sporting competition level
In a study by Palmer and colleagues (2018), alpha angles were on average 4° higher in adolescents who played sport as a school or club level, and 7.7° higher in individuals competing at a national or international level, compare with those who played no regular sport.8
Cam morphology and onset, frequency and duration of training
A recent systematic review and meta-analysis14 brought together the following evidence:
- Duration of sporting career has been associated with an increased alpha angle.
- Cam prevalence is increased in adolescents with sporting participation of >3 years vs <3 years.
- Age at which competitive soccer participation began was negatively associated with alpha angle values in 1 study – the earlier they started, the greater the alpha angle.
- Another study found an effect of training ≥4 times per week with an age cut off of 12, and no cumulative effect of training before the ages of 12-13.
The evidence suggests that throughout skeletal immaturity a dose - response relationship exists, with training ≥4 times per week, or >12.5 hours, resulting in greater risk of developing cam morphology.14
There was less clarity regarding at what age sporting loads begin to effect risk. Tak et al. (2015) suggest that the critical period is from age 12, as the cumulative effect of training before the age of 12-13 had no effect on cam development in their study.15
However, remember that Palmer et al. (2018) reported cartilaginous hypertrophy at age 10-11, preceding bony cam development, so there would seem to be growth plate responses as early at 10 years of age.8
Most studies report a dose-response relationship between cam morphology and activity levels – the higher the activity levels and level of competition, the larger the cam.

Type of sport: Cam morphology is more common in ‘hip-heavy’ or ‘power sports' athletes
So, we know that active individuals are more likely to develop cam morphology, but does it matter what type of activity? Yes, it appears it does. Doran et al. (2022) reported a higher prevalence of cam morphology in athletes who participated in what they referred to as ‘hip heavy’ sports – contact sports and sports that involve deep flexion and rotation.13 This includes sports such as soccer, basketball, baseball, ice hockey and martial arts.
Ice hockey players appear to be particularly at risk of developing cam morphology. Compared with the general population, elite ice hockey players are >3 times more likely to develop this femoral shape, with larger alpha angles recorded in this sub-population of athletes. Compared with skiers, ice hockey players are >4 times more likely to have cam morphology (odds ratio of 4.46), with 79% of ice hockey players presenting with this bone shape versus 40% of skiers.13
Westerman and colleagues (2021) assessed available bone imaging of 317 young participants involved in the longitudinal Iowa Bone Development Study, measured various impingement indices and compared the prevalence across different groups.16 They divided the population into non-athletes, power sport athletes (basketball, cheerleading, football, gymnastics, soccer, and volleyball) and non-power sport athletes (wrestling, baseball, cross-country or track and field, softball, or tennis), based on relative peak strain and ground reaction forces.
Compared with non-athletes, power athletes were almost 3 times more likely to develop cam morphology (odds ratio 2.93). In addition, non-power athletes did not have a significantly higher likelihood of developing cam morphology than non-athletes.16
Taking this information together, we know that adolescent males with open growth plates who participate at high levels in hip-heavy, power sports are at particularly high risk of developing cam morphology.
Pathogenesis of cam morphology – Why does cam morphology develop?
While researchers have provided quite a good idea of ‘who’ develops this femoral morphology, there is less clarity on the ‘why’. Let’s take a look at what is known and what has been suggested so far.
Is cam morphology a subtle slipped epiphysis?
One of the earliest theories around the pathogenesis of cam morphology was that this femoral shape was the result of a subtle slipped capital femoral epiphysis (SCFE). There has been a lack of agreement on this theory.
More recently, a study of bone features in a large osteological collection of 962 hips concluded that subtle SCFE-like deformity was not predictive of cam-like morphology. In fact, they found a mild opposite association – femurs with evidence of a subtle SCFE having smaller alpha angles. The authors concluded that although SCFE can lead to secondary cam morphology, it does not appear to explain idiopathic cam morphology.17
Changes in growth plate orientation – Lateral Epiphyseal Extension
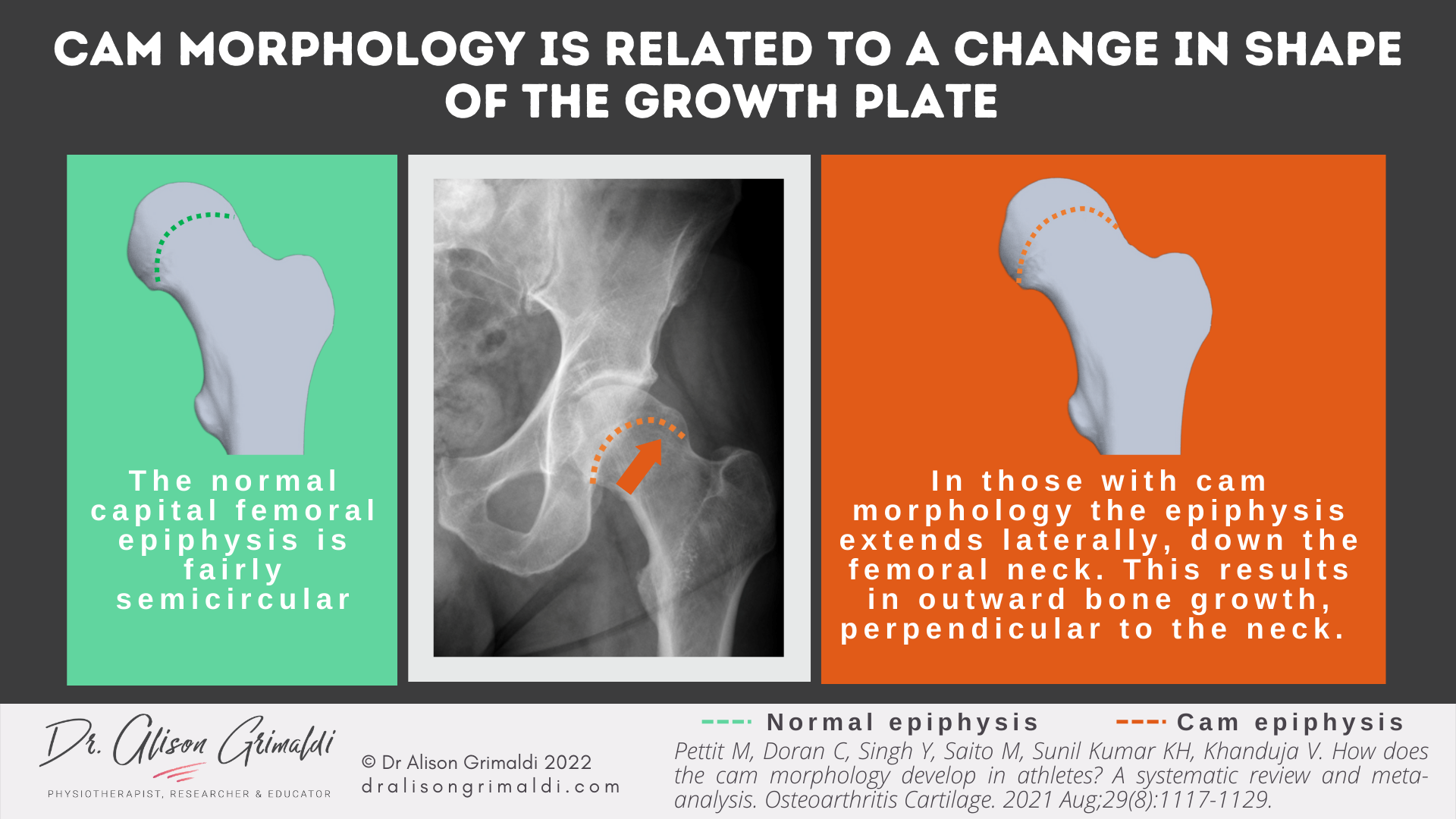
The bony feature that appears to be most closely linked to the development of cam morphology, is an extension of the lateral epiphyseal line. The typical epiphyseal line is visualised on 2-dimensional imaging as a fairly symmetrical curved line. In those who develop cam morphology, the lateral epiphyseal line appears to turn and start orienting down the femoral neck. Therefore, when growth occurs, bone will tend to grow outwards from the epiphyseal line, creating the characteristic bony prominence in the anterolateral head-neck junction.
In a recent meta-analysis, a strong positive correlation between epiphyseal extension and alpha angle was found in the pooled data from male, predominantly athletic populations.14 Therefore, it appears that cam morphology is a consequence of an alteration of the growth plate.
What causes lateral epiphyseal extension?
The next logical question then is ‘what causes lateral extension of the capital femoral epiphysis?’ Why does this occur in young, male athletes? The answer to this question is the one that might best direct prevention efforts.
Asymmetric closure of the growth plate
The leading theory is one of microinjury to the growth plate that results in asymmetric closure of the growth plate.
In 2015, Jonsson and co-authors reported results of their in vitro study using a skeletally immature porcine femur model. They exposed the femurs to repetitive vertical loading, which resulted in microscopic injuries to the physeal plate.18
In 2016, Cho and colleagues published a fascinating case report of a patient with cam-type femoroacetabular impingement.19 They showed MRI evidence of asymmetric closure of the capital femoral epiphysis. The posteromedial region of the epiphysis was closed, while the anterolateral area of the physis was still open at the site of the cam lesion.
This means that while no further growth was occurring at the posteromedial aspect of the femoral head, bony growth was still occurring in the anterolateral region, resulting in the relative overgrowth of the bone in the cam region.
This theory was tested very recently in another animal model of immature rabbits.20 These researchers surgically created an epiphyseal injury in the medial femoral head and waited to see what happened as the rabbits matured. They found that in the area of the iatrogenic injury at the medial proximal femoral physis, a bony bridge and/or growth arrest occurred. This resulted in a varus-type deformity, and a cam type shape of the anterolateral head-neck junction.
This link between cam morphology and varus head-neck alignment has also been made in humans.7,21 Coxa varus refers to a lower neck-shaft angle, where the femoral neck is more horizontal that a typical orientation. The early arrest of the medial growth plate may stunt the medial extension of the femur resulting in varus orientation, while the growth continues superolaterally to form the cam morphology.

What causes asymmetric closure of the growth plate?
Obviously, all of our young athletes have not been exposed to surgical injury to their growth plates. So, what is causing the asymmetric closure of their growth plates?
Cho and colleagues proposed that asymmetric epiphyseal closure may occur in response to unequal loading during intense physical activity.19 They cited evidence that when a highly compressive force is applied to a particular part of the growth plate, closure can be accelerated. Conversely, growth plate closure is delayed in regions where tensile force is focused.
The application of frequent, high loads across the femur is consistent with the population that is most likely to develop cam morphology – high volume athletes. Athletes involved in ‘power sports’ may also create higher compressive and tensile forces across the growth plate.
What type of actions might create unequal loading and the development of cam morphology?
In 2014, Roels et al. used finite element modelling of a femur with an open growth plate to study whether mechanical factors could explain the development of cam-type deformity in adolescents.22 Their results indicated that those exposed to hip flexion and external rotation forces are more likely to develop cam-type deformity that those exposed to regular loads of walking. They also suggested that this effect might be compounded by high impact loading. These findings were consistent with the type of sports those with cam morphology are most likely to be playing, such as soccer, basketball and ice-hockey.
Let’s reflect back on ice-hockey versus downhill skiing. What is it that makes ice hockey players at higher risk (>4 x higher) of developing cam morphology than downhill skiers? Is it the more abducted weightbearing position of ice hockey players and the high compressive loads imposed on the posterior hip by both muscle action and the anterior placement of the trunk centre of mass?
Ice hockey players are also at high risk of hip adductor injuries. Do high adductor forces create compressive load across the inferior aspect of the femoral head? Ice hockey goal-keepers tend to develop cam morphology in a slightly more anterior location, likely due to their unique hip loads – wide abduction and hip internal rotation. Relative to ice hockey players, elite downhill skiers tend to have a much narrower base of support and the centre of mass is usually situated more posteriorly – potentially increasing knee loads but reducing hip loads.
It is possible that posterior and inferior loads imposed by high muscle forces, and gravitational forces associated with position of the centre of mass, may result in excessively high compressive forces. These compressive forces may then arrest growth in the more posterior – inferior aspect of the physis, while the anterosuperior aspect continues to grow, resulting in typical cam morphology.
Links between inflammation and cam morphology
Is there a role for systemic inflammation? Emerging evidence suggests that for a small subset of adolescents that develop cam morphology, there may be an underlying systemic inflammatory condition. Seth and colleagues (2020) reported that 8.9% of paediatric patients with FAI were found to have an inflammatory comorbidity.23 This is markedly greater than the < 1% prevalence of immune-mediated inflammatory diseases in paediatric patients who have type-1 diabetes mellitus, inflammatory bowel disease, Hashimoto thyroiditis, and juvenile idiopathic arthritis.23
The presentation of the cam morphology in this subgroup however is distinctly different to the more common pistol-grip deformity with a large alpha angle and small offset. Adolescents with a systemic comorbidity had a unique and characteristic cam shape – a prominent sharp-edged beak with a negative femoral offset. Below the large beak, the bone drops back away quickly towards the femoral neck, resulting in the negative femoral offset.23
While an inflammatory co-morbidity is likely to occur in only a small subset of patients presenting with cam-type FAIS, recognition of this characteristic beak-shaped cam may lead to early identification of patients with undiagnosed inflammatory conditions.

Prevention of cam morphology
We are now fully aware of the significant risk this bony morphology represents for joint health. We know who tends to develop this bony shape and we are getting clearer about why. While research continues into the why, we also need to determine ‘how’.
How can we prevent cam morphology? This is certainly a challenging task, and the most obvious potential answers may be challenging to implement in the elite sporting world, where athletes are at highest risk of developing cam morphology.
Reducing exposure to hip-heavy sports to reduce load on the femoral growth plate
The lowest hanging fruit is of course activity levels. There is a clear dose-response relationship between level of activity/sport and development of cam morphology. The type of sport also appears highly relevant, with hip-heavy, power sports imparting the greatest risk.
The evidence suggests that risk of cam morphology may be reduced by keeping training/competition to less than 4 sessions per week:
- in adolescents with open growth plates, particularly between ages 12-14, but potentially as early as 10 years of age
- where the sport is a hip-heavy or power sport, such as soccer, football, basketball, baseball, ice hockey, volleyball, cheerleading and martial arts.
The Physical Activity Questionnaire provides another tool for evaluating level of physical activity, with a PAQ score of >3/5 increasing risk of cam morphology. However, the PAQ is rather a blunt tool, unable to provide important information on type, intensity, and duration of activity. More precise quantification tools and a comprehensive approach to load management in adolescents would be necessary.24
Physical activity is of course incredibly important in children and adolescents, so we need to ensure that the overall effect would not be to reduce other positive aspects of sports participation. As all sports are not equal in terms of potential impact on the femoral physis, perhaps one approach could be to pair ‘hip-heavy’ sports with ‘hip-light’ fitness training.
Cross training is certainly not a new concept, and perhaps could be applied in a very targeted manner that specifically selects low-cam-risk activities for cross training. This may help to ensure physical fitness is maintained if training sessions of ‘hip-heavy’ sports were reduced.
There is much work to be done to establish the validity or usefulness of any prevention plan, but it is clear that managing loads in adolescents will be an integral component of any prevention strategy.
Considerations for hip-heavy strength training in adolescents
Along with a rise in early sport specialisation, there appears to be a rise in strength training in children and adolescents. Overall, there is great potential benefit in resistance training and the global evidence suggests that risk of injury in youth training is low.25
However, the impact of additional weight training on cam risk in adolescent athletes participating in hip-heavy sports is unknown. If we apply what researchers have learnt so far, it is likely that hip-heavy resistance training may add to the overall risk of developing cam morphology.
In recent years, the strength training industry seems to have become enamoured with adding heavy bands around the knees for any type of glute training possible. The aim here is to increase work done by the posterior hip musculature, for higher strength/hypertrophy gains.
Impacts outside strength and hypertrophy are however rarely considered. I have previously mentioned my concerns about the effects of this type of training on muscle efficiency – i.e., training primary coronal and axial plane muscles to work at much higher intensities than required for sagittal plane tasks. Patterns of excessive co-contraction of buttock musculature are common in those who present with hip pain.
In adolescent athletes, knee-banded posterior chain strengthening may add high compressive load to the posterior capital femoral growth plate. Holding against a heavy band through the hip action, will impose not only higher but more sustained compressive loads through range. The concern is likely to be most relevant in athletes involved in hip-heavy sports, who are of course most regularly prescribed this type of gym exercise.
The high compressive load of such posterior hip strengthening may contribute to the mechanisms that induce early closure of the physis more posteriorly/inferiorly. As discussed above, science suggests that this results in uneven overgrowth at the anterosuperior growth plate and development of cam morphology.
So, what do we do? Is some of this training ok? Maybe? The problem is that the threshold that shifts the needle from positive to negative health impacts is unknown and will vary between individuals. Much further research is required to clarify if and how strength training contributes to the risk of developing cam morphology and the steps that should be taken to reduce these risks.
In the meantime, this is my suggestion. For adolescents, particularly males, involved in hip-heavy sports,
- Hip-heavy strength training may be best minimised during periods of high sport-related training/competition loads,
- The use of knee-banded gluteal training may be best avoided or minimised.

Screening for early intervention
With the next important frontier for cam-type FAIS being prevention, van Klij and colleagues (2021), investigated radiological and clinical features that might be predictive of cam development.21 If they appear prior to the development of the cam, these features might allow selection of higher-risk athletes for preventative measures.
Over a 5-year longitudinal study, they tracked
- epiphyseal extension (lateral extension linked with cam development),
- neck-shaft angle (varus angle linked with cam development),
- lateral centre-edge angle (relationship unknown), and
- hip internal rotation range of motion (commonly limited with cam morphology).
No links were found with lateral centre-edge angle. There were close links between cam morphology and the other 3 features. Unfortunately, cam morphology developed simultaneously with a varus orientation, growth plate extension towards the femoral neck and limited hip internal rotation.21
By the time these imaging and clinical features were present, so too was the cam. As none of these parameters preceded development of cam morphology, they cannot therefore be used in screening to identify at-risk individuals. Broad prevention strategies, particularly in adolescent males involved in hip-heavy sports may then need to be applied as early at 10 years of age.
Testing of such strategies is time consuming, with longitudinal studies of 5 or more years required and then more time to allow for analysis and publication. There is much work to be done to establish the validity or useful of any prevention plan, but it is clear that managing loads in adolescents will be an integral component of any prevention strategy.

-
- A detailed examination of mechanisms of physical overload (morphology, movement, muscle) and impairments associated with anterior hip pain and groin pain, clinical diagnostic tests and management approaches.
- Including joint related-pain & bony impingement (intra & extra-articular), soft tissue-related pain and nerve-related pain.

- All Online Hip Courses
- eBook Series
- Growing How-to Video Library
- Growing PDF Resource Library
- Live Hip Academy Zoom Meetings
- Hip Academy Forum
Check Out Some More Relevant Blogs
Another great Anterior Hip Pain blog

Anterior Hip Pain: Causes & Contributing Factors
Adequate consideration of individual causes and contributing factors is important for best outcomes.
References
- Agricola, R. et al. Cam impingement of the hip: A risk factor for hip osteoarthritis. Rev. Rheumatol. 2013; 9(10):630–634.
- Griffin DR, Dickenson EJ, Wall PDH, et al. Hip arthroscopy versus best conservative care for the treatment of femoroacetabular impingement syndrome (UK FASHIoN): a multicentre randomised controlled trial. Lancet. 2018 Jun 2;391(10136):2225-2235.
- Palmer AJR, Ayyar Gupta V, Fernquest S, et al. Arthroscopic hip surgery compared with physiotherapy and activity modification for the treatment of symptomatic femoroacetabular impingement: multicentre randomised controlled trial. BMJ. 2019 Feb 7;364:l185.
- Ishøi L, Thorborg K, Kraemer O, Hölmich P. Return to Sport and Performance After Hip Arthroscopy for Femoroacetabular Impingement in 18- to 30-Year-Old Athletes: A Cross-sectional Cohort Study of 189 Athletes. Am J Sports Med. 2018 Sep;46(11):2578-2587.
- van Klij P, Heijboer MP, Ginai AZ, Verhaar JAN, Waarsing JH, Agricola R. Cam morphology in young male football players mostly develops before proximal femoral growth plate closure: a prospective study with 5-year follow-up. Br J Sports Med 2019;53(9):532e8.
- Agricola R, Bessems JHJM, Ginai AZ, Heijboer MP, van der Heijden RA, Verhaar JAN, et al. The development of Cam-type deformity in adolescent and young male soccer players. Am J Sports Med 2012;40(5):1099e106.
- Agricola R, Heijboer MP, Ginai AZ, Roels P, Zadpoor AA, Verhaar JA, et al. A cam deformity is gradually acquired during skeletal maturation in adolescent and young male soccer players: a prospective study with minimum 2-year follow-up. Am J Sports Med 2014;42(4):798e806.
- Palmer A, Fernquest S, Gimpel M, Birchall R, Judge A, Broomfield J, et al. Physical activity during adolescence and the development of cam morphology: a cross-sectional cohort study of 210 individuals. Br J Sports Med 2018;52(9):601e10.
- Bailey DA. The Saskatchewan pediatric bone mineral accrual study: bone mineral acquisition during the growing years. Int J Sports Med 1997;18(Suppl 3):S191e4.
- Bailey DA, Martin AD, McKay HA, Whiting S, Mirwald R. Calcium accretion in girls and boys during puberty: a longitudinal J Bone Miner Res 2000;15(11):2245e50.
- van Klij, P., Heerey, J., Waarsing, J. and Agricola, R. The Prevalence of Cam and Pincer Morphology and its Association with Development of Hip Osteoarthritis. Journal of Orthopaedic & Sports Physical Therapy 2018; 48(4):230-238.
- Fernquest S, Palmer A, Gimpel M, Birchall R, Broomfield J, Wedatilake T, Dijkstra H, Burchall J, Lloyd T, Pereira C, Newman S, Carr A, Glyn-Jones S. A longitudinal cohort study of adolescent elite footballers and controls investigating the development of cam morphology. Sci Rep. 2021 Sep 17;11(1):18567.
- Doran C, Pettit M, Singh Y, Sunil Kumar KH, Khanduja V. Does the Type of Sport Influence Morphology of the Hip? A Systematic Review. Am J Sports Med. 2022 May;50(6):1727-1741.
- Pettit M, Doran C, Singh Y, Saito M, Sunil Kumar KH, Khanduja V. How does the cam morphology develop in athletes? A systematic review and meta-analysis. Osteoarthritis Cartilage. 2021 Aug;29(8):1117-1129.
- Tak I, Weir A, Langhout R, Waarsing HJ, Stubbe J, Kerkhoffs G. The relationship between the frequency of football practice during skeletal growth and the presence of a cam deformity in adult elite football players. Br J Sports Med 2015;49(9):630e4.
- Westermann RW, Scott EJ, Schaver AL, Schneider A, Glass NA, Levy SM, Willey MC. Activity Level and Sport Type in Adolescents Correlate with the Development of Cam Morphology. JB JS Open Access. 2021 Nov 11;6(4):e21.00059.
- Morris WZ, Furdock RJ, Yuh RT, Xie K, Fowers CA, Liu RW. Subtle slipped capital femoral epiphysis is not associated with idiopathic cam morphology. J Pediatr Orthop. 2021 Apr 1;41(4):216-220.
- Jónasson PS, Ekström L, Hansson HA, Sansone M, Karlsson J, Swärd L, Baranto A. Cyclical loading causes injury in and around the porcine proximal femoral physeal plate: proposed cause of the development of cam deformity in young athletes. J Exp Orthop. 2015 Dec;2(1):6.
- Cho YJ, Jung GY, Kim EJ, Chun YS, Rhyu KH. Asymmetric epiphyseal closure of the femoral head as a potential cause of the primary cam lesion: a case report. Skeletal Radiol. 2016 Sep;45(9):1299-302.
- Kamenaga T, Haneda M, Brophy RH, O'Keefe RJ, Clohisy JC, Pascual-Garrido C. A novel model of hip femoroacetabular impingement in immature rabbits reproduces the distinctive head-neck cam deformity. Am J Sports Med. 2022 Jun;50(7):1919-1927.
- van Klij P, Heijboer MP, Ginai AZ, Verhaar JAN, Waarsing JH, Agricola R. Clinical and radiological hip parameters do not precede but develop simultaneously with cam morphology: a 5-year follow-up study. Knee Surg Sports Traumatol Arthrosc. 2021 May;29(5):1401-1410.
- Roels P, Agricola R, Oei EH, Weinans H, Campoli G, Zadpoor AA. Mechanical factors explain development of cam-type deformity. Osteoarthritis Cartilage. 2014 Dec;22(12):2074-82.
- Seth A, Yen YM, Tourn D, Smit K, Carsen S. A Unique and Characteristic Cam FAI Morphology in Young Patients with Comorbid Inflammatory Conditions. J Bone Joint Surg Am. 2020 Nov 4;102(Suppl 2):15-21.
- Murray A. Managing the Training Load in Adolescent Athletes. Int J Sports Physiol Perform. 2017 Apr;12(Suppl 2):S242-S249.
- Stricker PR, Faigenbaum AD, McCambridge TM; Council on Sports Medicine and Fitness. Resistance training for children and adolescents. Pediatrics. 2020 Jun;145(6):e20201011.