The case against iliopsoas release

Last month we looked why the iliopsoas muscle has been so demonised and the reported indications and techniques for iliopsoas release. But what evidence is there for or against iliopsoas release? In what scenarios might it be regrettable but unavoidable? In what scenarios should it be contraindicated? In this month’s blog, I’ll be presenting the evidence and the case against iliopsoas release in most situations.
The case against iliopsoas release will cover the following topics:
- No other hip flexors do what the iliopsoas does
- Lack of understanding of symptoms and underlying mechanisms
- Efficacy of iliopsoas release
- Potential risks and complications of non-surgical iliopsoas release
- Risks and complications of iliopsoas tenotomy
- What are the long term sequalae of iliopsoas release?
- Alternative approaches to addressing iliopsoas issues


No other hip flexors do what the iliopsoas does!
The first important point in the case against iliopsoas release is that no other hip flexors do what the iliopsoas does. The apparent flippancy with which some surgeons release this important muscle is concerning. I recently had a patient report that her surgeon told her that he routinely releases the iliopsoas during arthroscopy, for good measure! It’s as if the iliopsoas is a redundant muscle, just one of many hip flexors.
Sure, we have other muscles that can help lift the thigh, but none of these long strappy thigh muscles can replace the other essential functions of the iliopsoas:
- providing dynamic anterior stability for the hip joint
- providing anterior support for the sacroiliac joint
- providing anterior support for the lumbar spine
- lifting the hip into inner range hip flexion
- transferring load between the trunk and femur during gait.
Jump back to last month’s blog if you’d like to review the anatomy and function of the iliopsoas.
Lack of understanding of symptoms and underlying mechanisms
So why has the poor iliopsoas become so demonised? Perhaps because of its extensive connections, some interpret this as the ‘connection’ between back, pelvic and hip pain – it’s the thing that connects them all, so therefore it must be the underlying issue! Inadequate reasoning, and not supported by the scientific literature.
Assumptions of iliopsoas tightness
There has been a huge overemphasis on iliopsoas tightness as the primary ‘dysfunction’ afflicting this muscle complex - that this tightness is the reason for anterior hip, pelvic, back pain … and various other problems.
And yet, if you look for evidence of links between iliopsoas tightness and hip conditions – persistent anterior hip pain, snapping hip, labral impingement, iliopsoas impingement – there is no convincing evidence at all that iliopsoas tightness is the mechanism underlying these conditions. Particularly surgical case studies frequently mention iliopsoas tightness as a rationale for releasing or lengthening the iliopsoas, and yet there does not appear to have been any pre-operative assessment of hip extension range of motion in these cohorts. The rationale is based on an assumption.
In those with anterior snapping hip (internal coxa saltans), there has been a long-held belief that tightness causes snapping of the tendon over the anterior bony structures. Recommended treatment has been massage, stretching and finally surgical partial release or lengthening of the iliopsoas tendon. Snapping hip has been reported to be present in 5 - 10% of the general population,1 but at least 60% of a classical dance population.2
Does this mean that dancers have an extremely high prevalence of iliopsoas shortness and restricted hip extension? Doesn’t make sense, does it? This population is much more likely to be long in their iliopsoas, with large ranges of hip extension.


Would you like to learn more about the iliopsoas?
My Anterior Hip and Groin Pain online course is for you! Built in an easy to consume layout, learn in your own time, from the comfort of your own home. Discover joint related pain and bony impingement, soft tissue related pain, referred and nerve related pain & lots more! Explore this course today, and help more patients!
Sure, the iliopsoas can be tight in some people with anterior hip pain and it may impact on the hip joint, for example due to increased anterior pelvic tilt and earlier anterior impingement. However, stretching or iliopsoas release is unlikely to be helpful, particularly in the longer term. Read more below on alternative approaches to addressing iliopsoas issues.
Iliopsoas upregulation
Due to its important role in hip joint protection and anterior support, in some people with reduced passive support mechanisms (acetabular dysplasia, capsuloligamentous laxity or deficiency), the iliopsoas may increase its activity in compensation. The patient may sense this tension, but this doesn’t mean that overall muscle length is reduced and certainly doesn’t mean that the iliopsoas needs to be released – this can be devastating for the underlying joint (read more on this below).
Increased muscle activity can also simply be a response to pain – that all too familiar muscle guarding. Even in those with hip joint conditions without stability issues, we may see upregulation of the iliopsoas and we also commonly see adductor guarding. Does this mean these muscles should be surgically released? No! This is a response and not the underlying issue.
Increased muscle recruitment may also be due to muscle weakness or inefficiency, greater numbers of motor units required for function.
While the iliopsoas may become upregulated (higher levels of muscle recruitment for a given task) or even tight, it has been my experience as a high-volume hip physiotherapist that:
- the iliopsoas is more commonly long than short in those with persistent anterior hip pain with iliopsoas snapping,
- iliopsoas related pain is more commonly related to overload imposed by excessive hip extension, than tightness associated with limited extension,
- upregulation of the iliopsoas is most commonly a response to reduced stability, pain or weakness,
- addressing underlying mechanisms is far more effective, particularly in the long term, than iliopsoas stretching or release strategies.


Efficacy of iliopsoas release
Let’s look at the evidence around the efficacy of surgical and manual interventions, in the case against iliopsoas release.Systematic reviews of surgical iliopsoas release report favourable outcomes, with arthroscopic techniques superior to open techniques with regards to recurrence of snapping (5.1% vs 21.7%) and groin pain relief (89.1% vs 85.6%), and with fewer complications (4.2% vs 21.1%) overall.3
BUT, almost all studies reporting outcomes of surgical iliopsoas release are case series, predominantly retrospective, with only 1 randomised controlled trial and this study comparing 2 different surgical techniques. The evidence to date then is overall of relatively low quality, with substantial risk of bias. Particularly in retrospective reviews, the loss to follow up is problematic, as the patients who are lost may often be those with poor outcomes, resulting in artificially positive outcomes.
Another issue with arthroscopic studies, is that iliopsoas release is often performed together with other intra-articular procedures such as labral debridement or repair,3 making it impossible to attribute positive outcomes directly to the iliopsoas release.
One recent surgical study reported that outcomes were significantly poorer in patients with iliopsoas pathology who underwent iliopsoas release during arthroscopy for femoroacetabular impingement syndrome (FAIS). These authors warned that ‘indiscriminate tenotomy for iliopsoas pathology in this setting should be cautiously considered.’4
Indeed, despite reviews reporting favourable results of iliopsoas release, there appears to be diverse beliefs and practices amongst even high-volume hip arthroscopists. A survey study of 16 highly experienced, high-volume hip arthroscopists reported that iliopsoas tenotomy was performed by these surgeons 12% of the time on average, but the range was between 0.5 - 90% of hip arthroscopy cases!5 This certainly reflects a huge variance.
This variance may be a reflection of the problem highlighted by this paper - that surgeons have been making decisions based on limited, even anecdotal evidence, with no high-level research or consensus on how to best manage the iliopsoas.5 Of those surveyed, 75% of high-volume hip arthroscopists reported that the frequency with which they perform iliopsoas tenotomy had decreased over time. This was not due to any guidance from the scientific literature, but most commonly due to their perception of poor outcomes in their own practice.


With regard to non-surgical options for iliopsoas management, there is arguably even poorer guidance and evidence available in the literature. Non-surgical management of iliopsoas snapping or impingement described in scientific papers most commonly includes repeated local injections (local anaesthetics and corticosteroids) into the iliopsoas tendon sheath and surrounds, and stretching exercises.6,7 From the available low-quality literature on snapping hip, between 36% and 67% of patients diagnosed experience reduction or resolution of symptoms with conservative measures.7
Results of such non-surgical interventions for iliopsoas tendon impingement are, not surprisingly, relatively poor compared with surgical interventions6,8,9 - local anaesthetics and corticosteroids are toxic for tendons and stretching into a position of impingement makes no logical sense at all!
Potential risks and complications of non-surgical iliopsoas release – manual therapy techniques
If we reflect on the anatomical relationships of the iliopsoas discussed in last month’s blog, the risks of deep pressure or friction targeted at the muscle bellies of the iliacus and psoas, would mainly be related to possible injury imparted to the internal organs or nerves that sit anterior to these muscle bellies.
The other ‘risks’ are those inherent in providing patients with unhelpful explanations and beliefs around their condition, and the financial, time and psychological burdens of ineffective treatments. In addition, pain commonly accompanies manual ‘iliopsoas release’ and unnecessary persistence of their hip pain may be experienced if treatment is unsuccessful.
Risks and complications of iliopsoas tenotomy
The risks and complications or surgical iliopsoas release are more concerning and some irreversible.
Reported complications of surgical iliopsoas release include:3
- Recurrence of iliopsoas snapping
- Hip flexor weakness
- Iliopsoas atrophy
- Lateral femoral cutaneous nerve injury
- Anterior hip instability and dislocation
- Persistent pain
- Heterotopic ossification
- Infection
- Haematoma
- Abdominal compartment syndrome
- Partial femoral nerve palsy
- Joint stiffness
- Genital numbness, and
- Pseudoaneurysm of the femoral circumflex artery
Hip flexor weakness after iliopsoas release
Hip flexor weakness and iliopsoas atrophy are the most common complications.3,7,10 Immediately after surgery, patients experience a marked loss of active flexion for 2-8 weeks, requiring crutches for mobilisation.10 This profound weakness gradually recovers with studies often reporting full return of strength, usually within 12 months.
However, these assessments of hip flexor strength are predominantly performed as observation of functional movement, such as performance of an active straight leg raise, or manual muscle tests. These are not ideal objective measures, particularly in an unblinded test environment. One study using manual muscle testing did report that only 50% of their cohort achieved 5/5 (full strength), with 39% achieving 4/5 and 11% scoring 3/5.11
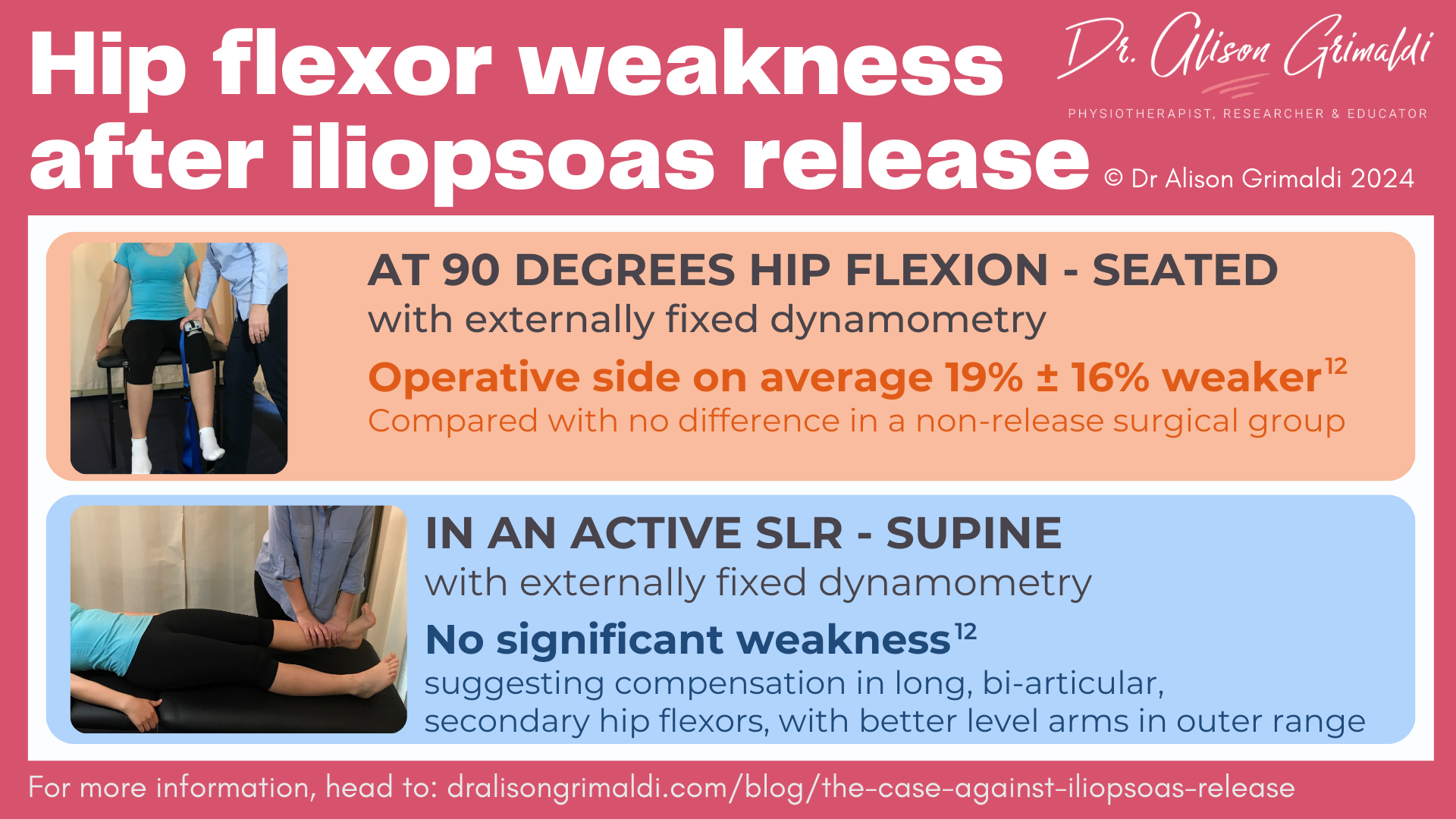
Objective hip flexor dynamometry has only been used in one study, performed in a standardised seated test position and also as a resisted active straight leg raise in around 10° of hip flexion. In the seated position, Brandenburg and colleagues (2016) demonstrated a mean 19% hip flexor strength deficit compared with the other side, at least 12 months after arthroscopic iliopsoas release.12
In the long lever, supine straight leg raise position, no significant strength deficit was detected.12 This suggests the long bi-articular hip flexors are able to compensate in the long-lever, outer-range test, but are mechanically disadvantaged in the inner-range, short-lever test. The seated test, or tests in inner-range flexion, are a better reflection of iliopsoas deficits.

Iliopsoas atrophy after iliopsoas tenotomy
Atrophy of the iliopsoas muscle has also been assessed followed surgical iliopsoas release, using Magnetic Resonance Imaging (MRI). Atrophy occurs to variable degrees, depending on the level of iliopsoas release.
Studies have only been performed in those with native hips i.e., not in those who have had iliopsoas release post total hip replacement. Two studies visually assessed the level of fatty infiltration of the iliacus and psoas on MRI before and after iliopsoas release, assessing the muscle tissue only around the level of the iliopectineal eminence (pelvic brim level).11,13
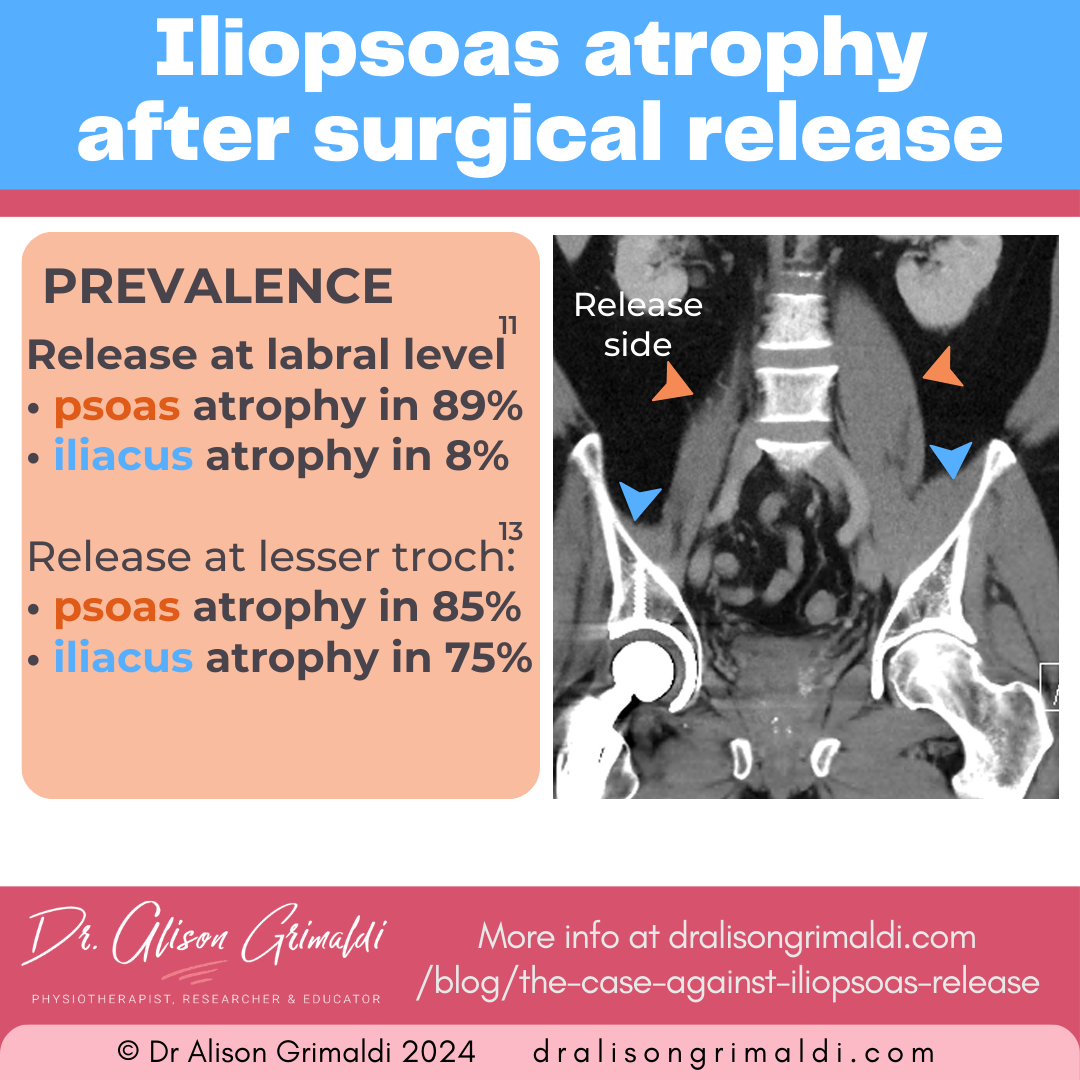
Following an iliopsoas release at the labral level (central compartment release):11
- psoas atrophy was evident in 89% and
- iliacus atrophy was present in 8% of patients.
Following an iliopsoas release at the lesser trochanter:13
- psoas atrophy was evident in 85% and
- iliacus atrophy was present in 75% of patients.
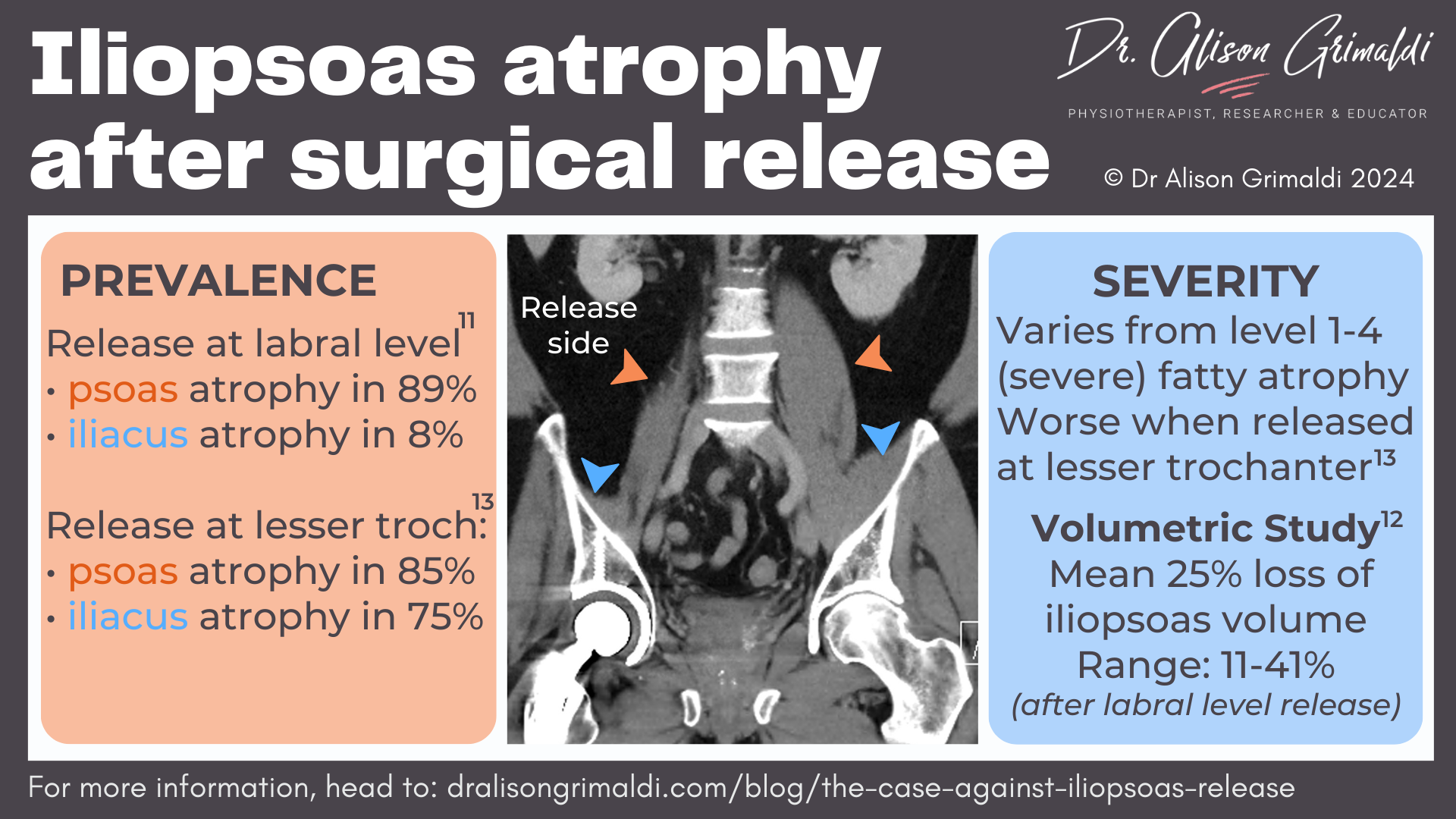
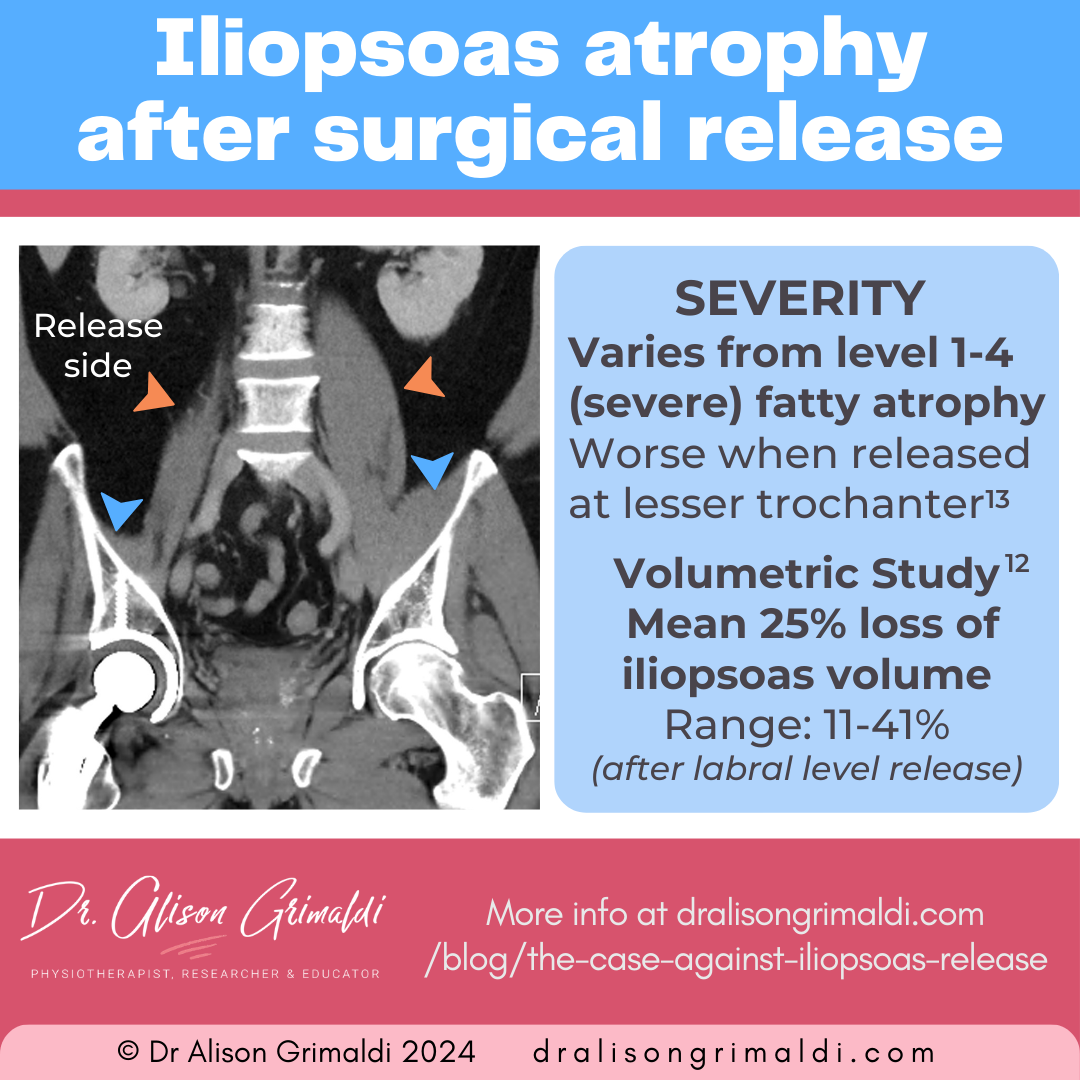
The severity of the fatty infiltration was variable, ranging from mild (grade 1) to severe (grade 4), with higher prevalence of severe atrophy after iliopsoas release from the lesser trochanter - over half that group with grade 4 atrophy (more fat than muscle).13
Clearly, release at the lesser trochanter results in greater levels of atrophy, due to the greater proportion of the muscle-tendon unit that is released. Return to last month’s blog to if you need, to revise the changing muscle-tendon proportions within the iliopsoas.
The iliacus is more profoundly impacted by a lesser trochanter release. This is because at the labral level, the tendinous structure is primarily the psoas tendon, with iliacus predominantly muscle tissue, while at the lesser trochanter iliacus is also predominantly a tendon structure.
These 2 studies only provide a localised snapshot of atrophy in one area of the muscle at the pelvic brim. However, Brandenburg and colleagues (2016) measured volumes of the whole iliopsoas muscle, comparing the operated and non-operated side after arthroscopic, central-compartment release. They also compared side-side differences in a control group who had undergone arthroscopic surgery but without iliopsoas release.12 They reported an average 25% (range 11 – 41%) loss of iliopsoas muscle volume after iliopsoas release compared to the contralateral side, and no significant difference in the control group.
Unfortunately, all these studies were retrospective in nature, with only a small percentage of the operative groups studied, and MRIs taken at variable time points – 3 months to 6 years.
To better understand the impact of iliopsoas release on muscle size, we need:
- prospective studies,
- collecting MRI scans on all patients,
- and a comparable surgical but non-release control group,
- performed at a consistent time point,
- with repeatable, objective measures of both muscle size and quality (fatty infiltration),
- using volumetric analysis of the iliopsoas, and separate cross-sectional area evaluation of iliacus and psoas at distinct levels through the isolated muscle bellies.
It would also be valuable for future studies to assess size changes in secondary hip flexors, such as the sartorius, tensor fascia lata (TFL) and rectus femoris. The Hain and Walczak studies both reported no compensatory hypertrophy in nearby muscles, although there was no formal measurement performed, simply a visual impression.11,13 Brandenburg and colleagues (2016) did not measure other muscles but suggested that this would be important in future studies.12
In clinical practice, I regularly note presumably compensatory hypertrophy of the sartorius and sometimes the TFL musclesin the longer term, usually > 9- 12 months post iliopsoas release surgery. A shift in the relative bulk and contribution of muscles within the hip flexor surgery may have implications, such as alterations in the force vectors within the underlying joint or prosthesis – read more about possible long term sequalae below.

Understand the Iliopsoas better!
This Anterior Hip and Groin Pain online course can help you help more people with Anterior Hip & Groin Pain! Explore joint related pain and bony impingement, soft tissue related pain (including iliopsoas related pain), referred and nerve related pain & lots more! Signup today!
Hip joint instability and dislocation following iliopsoas release
One of the other concerns regarding iliopsoas tenotomy is reduction of anterior joint stability, and even anterior dislocation. To access the iliopsoas tendon during hip arthroscopy, a large capsulotomy needs to be performed – i.e., the anterior capsule needs to be opened. This means 2 of the major anterior restraints, the iliopsoas and the capsule, have been sectioned during an arthroscopic transcapsular iliopsoas release. The critically important iliofemoral ligament may also be damaged in a large anterior capsulotomy.
Anterior dislocation of 3 native hips in young active individuals has been reported after iliopsoas release and anterior capsulotomy.3 One case of dislocation of a prosthetic femoral head has also been reported after iliopsoas release for iliopsoas impingement following total hip arthroplasty.10 However, the actual prevalence of gross instability and dislocation following arthroscopic surgery is unknown. The few case reports of instability after iliopsoas release may underestimate this devastating complication.
Harms reporting (reporting of complications) in systematic reviews of hip arthroscopy outcomes has been shown to be inadequate,14 and this is partly due to the fact that some studies may not report complications at all. In Gouveia and colleagues’ 2021 systematic review of post operative outcomes after arthroscopic iliopsoas tenotomy, 7 of 21 studies did not report complications.15
A lack of adequate reporting of complications means that it is not possible to fully understanding the potential consequences of a procedure. And remember, the surgeons performing procedures in these studies are generally highly experienced surgeons. It is unknown how closely the reported complication rates in scientific papers reflects that in the community after iliopsoas release performed by less experienced surgeons.
If gross instability and dislocation can occur after iliopsoas release, it stands to reason that microinstability may occur and be even more common. How many patients are affected is unknown, as this is difficult to measure objectively and has not been reported as a complication in any studies to date.
The risk of dislocation or post-operative instability following iliopsoas tenotomy will be influenced by a number of surgical and patient factors. Iliopsoas release via arthroscopy is often performed concurrently with other intra-articular procedures, and lack of capsular closure during hip arthroscopy may result in instability – remember the capsule is opened during arthroscopy and not all surgeons repair the capsule.
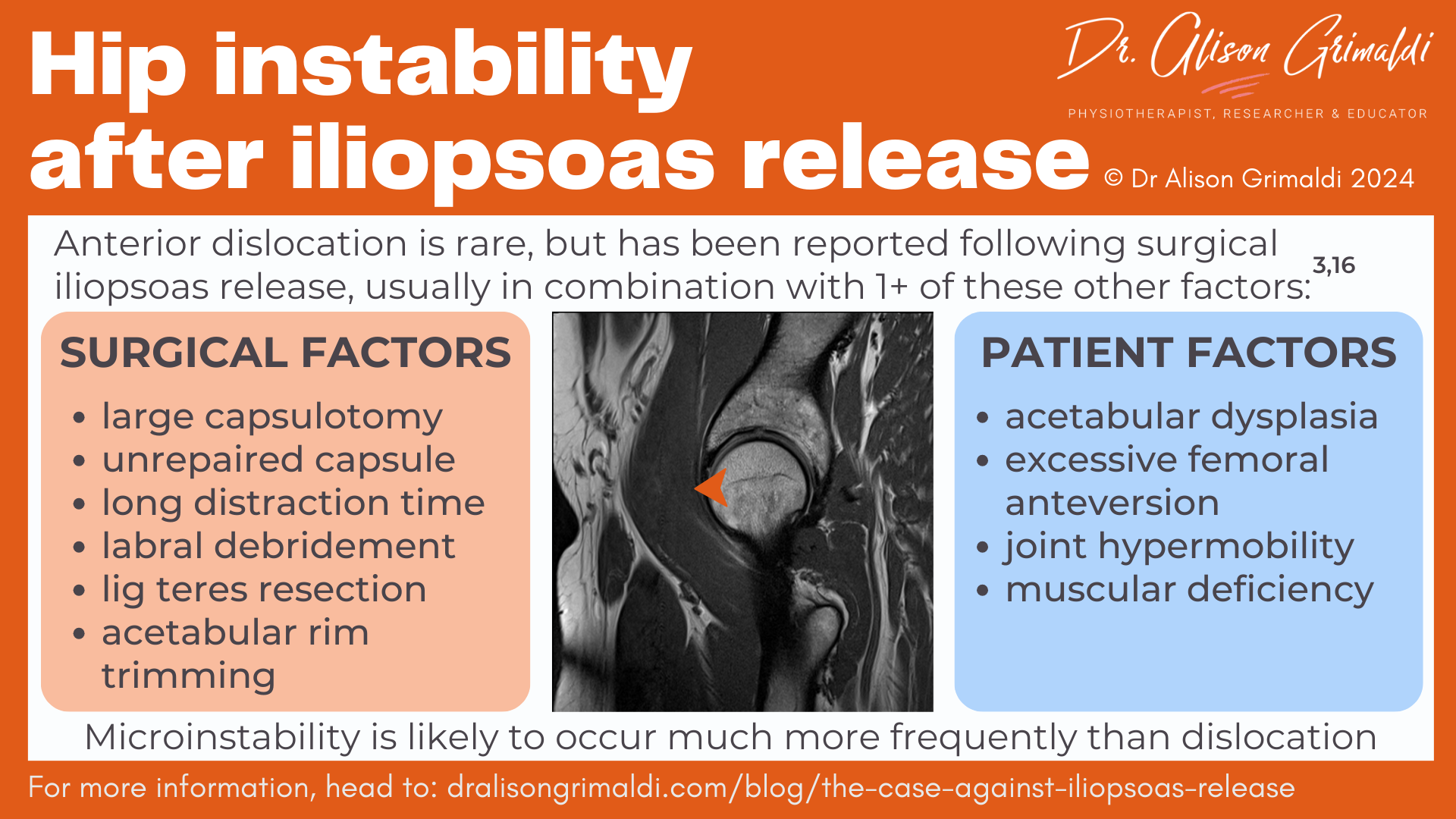
Surgical factors that may increase risk of instability following iliopsoas release include:3,16
- excessive capsulotomy, particularly anterior capsule from the central compartment,
- unrepaired capsulotomy,
- long distraction time (common in FAIS surgery), resulting in ligament elongation,
- labral debridement,
- ligamentum teres resection, and
- acetabular rim resection
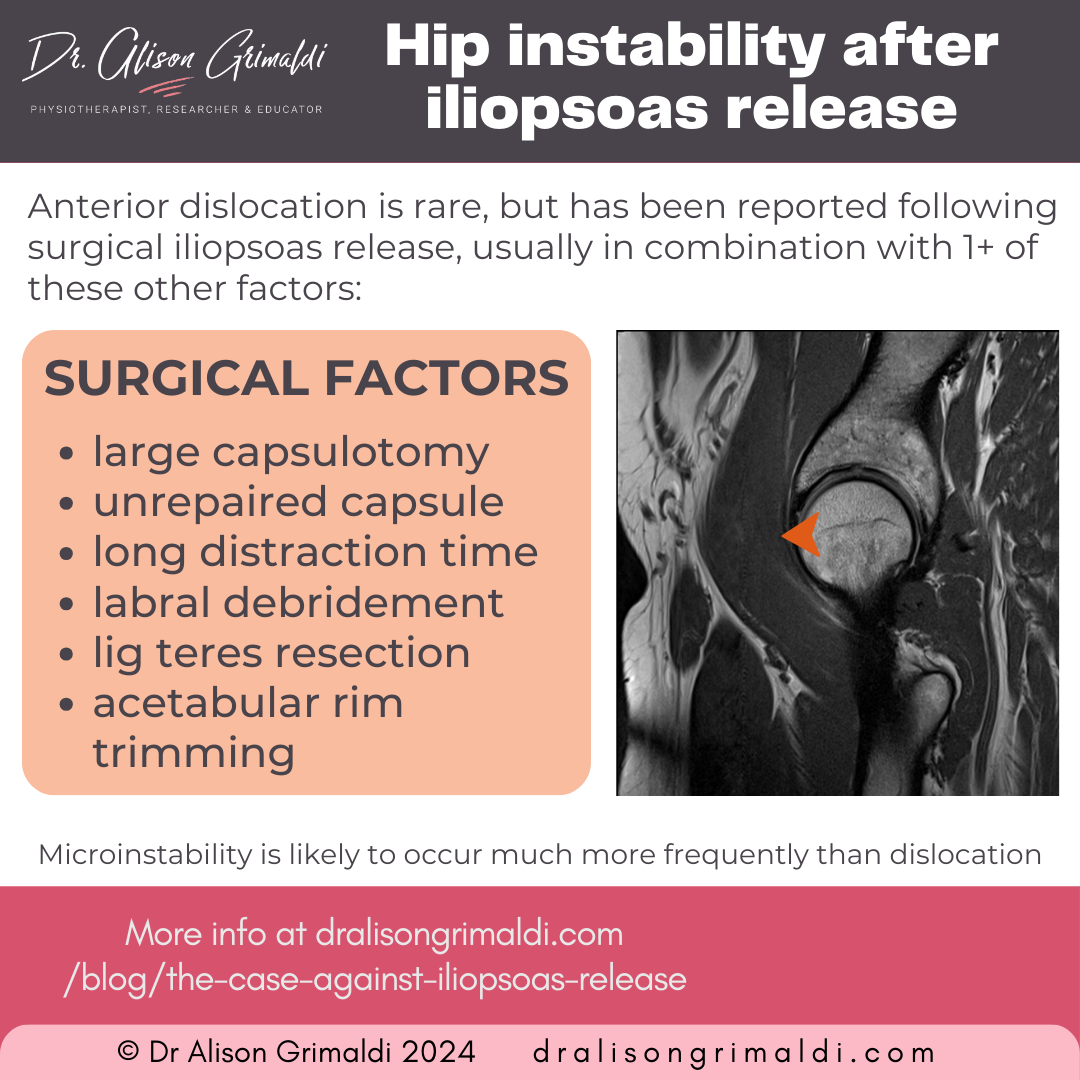
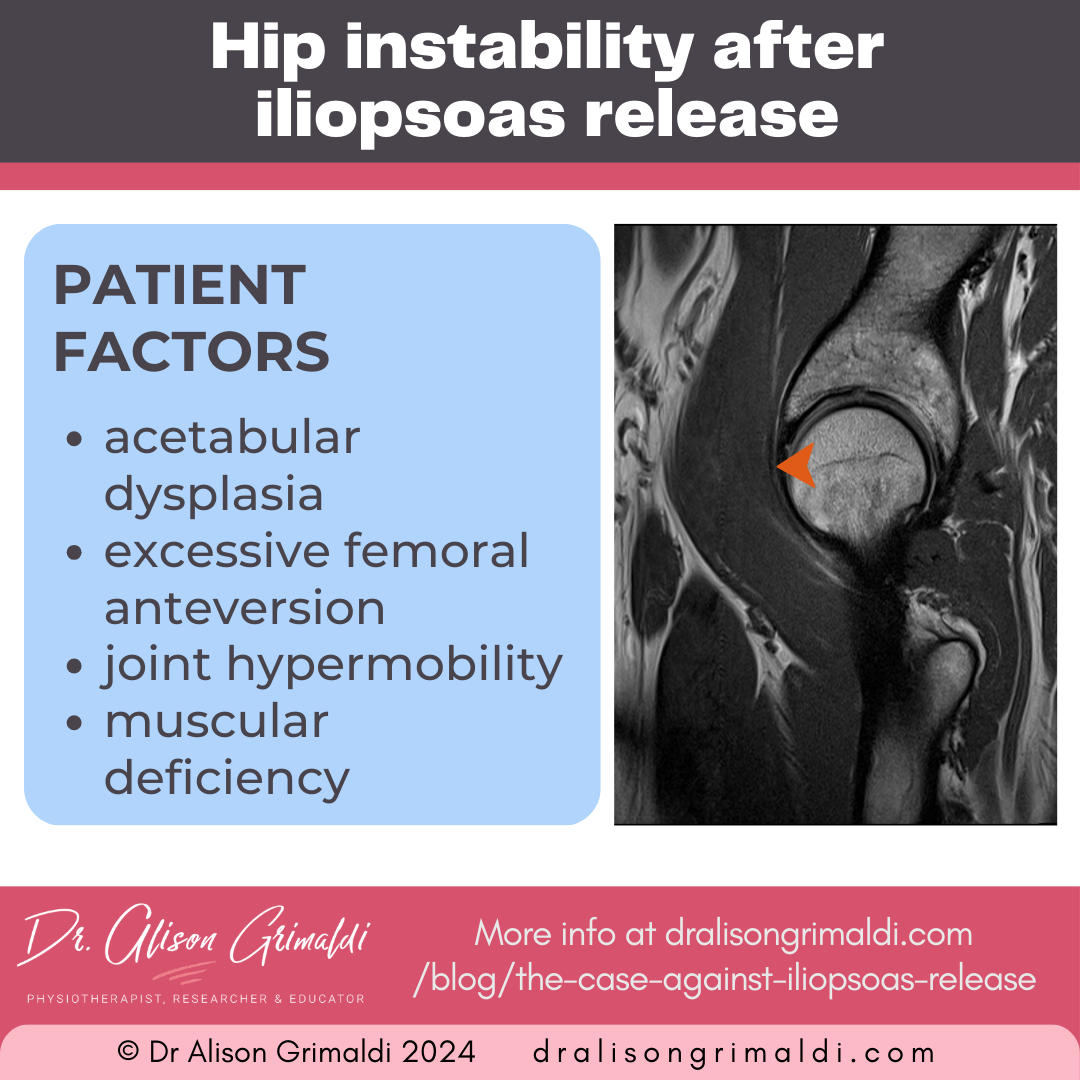
Patient factors that increase risk of instability following iliopsoas release include: 3,16
- acetabular dysplasia,
- excessive femoral anteversion,
- joint hypermobility, and
- muscular deficiency.
What are the long term sequalae of iliopsoas release?
While we have some, albeit inadequate, information on early-medium term complications, we have minimal information on the long term effects of surgical iliopsoas release. Major concerns are around the impact on the underlying hip joint and lumbar spine, but there many also be less easily measured impacts on gait, muscle efficiency and fatigue.
Long term sequalae of iliopsoas release for the underlying hip joint or prosthesis
Microinstability of the hip joint is likely to have an adverse effect on joint or prosthetic health over longer time frames. The chondral surfaces of the native hip joint are known to deteriorate over time in response to excessive translation and the associated shear force. Without the full anterior restraint of the iliopsoas, the anterior capsule and labrum may also be adversely impacted by increased anteriorly directed forces from the femoral head.
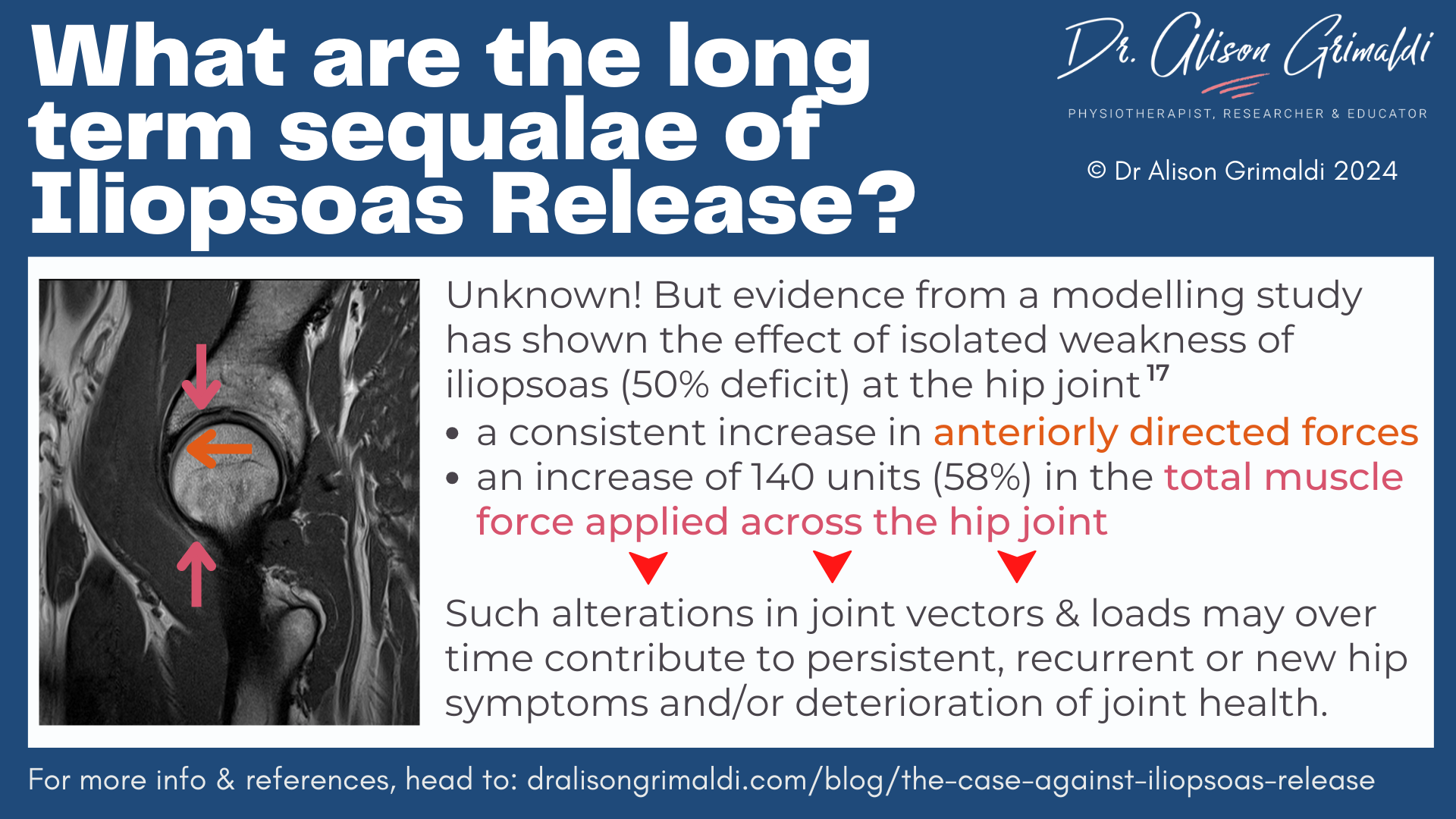
Cara Lewis and colleagues have done some nice work in this space, using musculoskeletal modelling.17 They demonstrated the importance of the iliopsoas in moderating overall and anteriorly directed joint forces during sagittal plane tasks. Within the model, they were able to manipulate force contribution from various muscles and assess impact on joint forces.
During a simulated supine active straight leg raise, between 10° extension and 30° flexion,
- A 50% reduction of iliopsoas force resulted in:
- a consistent increase in anteriorly directed forces across the range, and
- an increase of 140 units (58%) in the total muscle force applied across the hip joint at 0°.
- A 50% reduction of rectus femoris, sartorius and tensor fascia lata force resulted in:
- An increase of only 16.4 units (6.8%) in the total muscle force applied across the hip joint at 0°.
What this tells us, is that reduced contribution from the iliopsoas within the hip flexor synergy will result in greater anteriorly directed forces. This means the anterior femoral head will apply greater force onto the anterior-superior acetabular cartilage, the labrum and capsule.
The hip flexor synergy also loses efficiency, resulting in higher total forces imposed on the joint by muscles. This is because, when you reduce contribution from the efficient primary flexor – iliopsoas, relatively inefficient secondary flexors whose primary action is in another plane, need to increase their contribution to compensate and balance each other. This results in higher cumulative muscle forces on the underlying joint.
Many surgical studies brush off the impact of iliopsoas release, reporting a partial-to-full recovery of hip flexor strength, even in the presence of iliopsoas atrophy. Does this mean that everything is ok?? Lewis’ research shows that reduction of iliopsoas contribution and compensatory increase in contribution from inefficient secondary hip flexors is likely to impose aberrant loads on the hip joint, that may over time contribute to persistent, recurrent or new hip symptoms and/or deterioration of joint health.

Long term sequalae of iliopsoas release for the lumbar spine
And what about the lumbar spine?!! No-one talks about the impact on the lumbar spine, but the psoas muscle belly is the portion of the iliopsoas that is most impacted by iliopsoas release. In last month’s blog, we talked about the important role of the psoas major in providing support for the lumbar spine – the only muscle attaching to the lumbar vertebral column anteriorly.
What is the impact of longstanding asymmetry of the psoas major muscle belly? Low back pain? Asymmetrical spinal degeneration? Scoliosis? How can there be no impact in the longer term?
Let’s try to think more about the future!
Alternative approaches to addressing iliopsoas issues
With all of these potential short and long-term complications and implications, iliopsoas release should be a last resort after a prolonged trial of a high-quality, clinically reasoned rehabilitation program.
A trial of repeated corticosteroid injections, NSAIDS and hip flexor stretching is simply NOT ADEQUATE! And may be harmful…
Find out what the real problem is
The initial priority is a detailed assessment that aims to reveal not only the source of pain, but the true underlying mechanisms. There should NEVER be an assumption that pain at the front of the hip (even if reproduced on resisted hip flexion and stretching) is from the iliopsoas, related to tightness and overactivity of a misbehaving muscle.
Perform a thorough assessment, with the priorities including:
- Diagnostic tests for local joint, soft tissue and nerve related pain, and referral sources,
- Anterior hip joint stability tests,
- Hip and lumbopelvic mechanics. How do they stand, walk, move? Pelvic position is critical! (Hip Academy members – see the recorded lecture on this),
- Muscle assessment – not just strength testing, assess length and function within the hip flexor synergy.
Address impairments and underlying mechanisms
Use a clinically reasoned rehabilitation approach:
- Focus on optimising load imposed on the anterior soft tissues and joint structures (Hint: Pelvic position/control and range of hip extension used during function is critical!),
- Address impairments in hip flexor function and strength,
- Avoid hip flexor stretching for anterior hip pain, snapping hip and iliopsoas impingement,
- Use eccentric lengthening of the iliopsoas, avoiding extended hip positions, IF hip extension range is limited by soft tissue tightness (Test it),
- Address accompanying impairments and contributors.
I hope the information in this and last month’s blog on the what, why and how of iliopsoas release, has helped clarify the case against iliopsoas release. Time and money spent on painful manual ‘iliopsoas release’ techniques is not justified. These should be set aside and replaced by high-quality, clinically reasoned assessment and management techniques.
High-quality non-surgical interventions may save our patients from often unnecessary surgical techniques with irreversible effects on the iliopsoas itself and the unknown implications for long term hip joint and lumbar spine health.
Also, it is worth noting that with anterior approach hip arthroplasty, there appears to be quite a high prevalence of soft-tissue related pain and hip flexor dysfunction, despite the ‘muscle sparing’ technique. This does not mean the iliopsoas is short or even impinging on the prosthesis, and infiltration of local anaesthetic and corticosteroids around the iliopsoas will also impact on other nearby nociceptors.
Iliopsoas should not be undertaken lightly following total hip arthroplasty. This important stabilising structure is also likely to play a role in optimal prosthetic health in the longer term. This becomes even more important with the younger cohort who are now being offered early arthroplasty.
The keys here are optimal early care after anterior approach arthroplasty in particular. Aim to reduce local swelling quickly, avoid excessive scar formation, restore optimal hip flexor function and very importantly, control anterior soft tissue loads imposed by pelvic and hip joint position. (Hip Academy members, you’ll find lectures on post-operative rehabilitation in your Hip Academy Meetings area)
There will be situations where prosthetic impingement of the iliopsoas is too great, even when all factors are optimised. In these cases, iliopsoas release has lower rates of complications than revision of the acetabular cup. Iliopsoas release may be unavoidable but ensure high quality rehab is exhausted first, aim for a release at the joint level, rather than the lesser trochanter, and optimise iliopsoas function postoperatively.

This blog was written by Dr Alison Grimaldi
Dr Alison Grimaldi is a physiotherapist, researcher and educator with over 30 years of clinical experience. She has completed a Bachelor of Physiotherapy, a Masters of Sports Physiotherapy and a PhD, with her doctorate topic in the hip region. Dr Grimaldi is Practice Principal of PhysioTec Physiotherapy in Brisbane and an Adjunct Senior Research Fellow at the University of Queensland. She runs a global Hip Academy and has presented over 100 workshops around the world.
Check Out Some More Relevant Blogs
- Byrd JW. Snapping hip. Oper Tech Sports Med. 2005;13:46-54.
- Winston P, Awan R, Cassidy JD, Bleakney RK. Clinical examination and ultrasound of self-reported snapping hip syndrome in elite ballet dancers. Am J Sports Med. 2007 Jan;35(1):118-26. doi: 10.1177/0363546506293703. Epub 2006 Oct 4. PMID: 17021311.
- Longstaffe R, Hendrikx S, Naudie D, Willits K, Degen RM. Iliopsoas Release: A Systematic Review of Clinical Efficacy and Associated Complications. Clin J Sport Med. 2021 Nov 1;31(6):522-529. doi: 10.1097/JSM.0000000000000784. PMID: 32032164.
- Matsuda D, Kivlan BR, Nho SJ, Wolff AB, Salvo JP Jr, Christoforetti JJ, Martin RL, Carreira DS. Tenotomy for iliopsoas pathology is infrequently performed and associated with poorer outcomes in hips undergoing arthroscopy for Femoroacetabular Impingement. Arthroscopy. 2021 Jul;37(7):2140-2148. doi: 10.1016/j.arthro.2021.02.018. Epub 2021 Feb 23. PMID: 33631254.
- Chen AW, Steffes MJ, Laseter JR, Maldonado DR, Ortiz-Declet V, Perets I, Domb BG. How has arthroscopic management of the iliopsoas evolved, and why? A survey of high-volume arthroscopic hip surgeons. J Hip Preserv Surg. 2020 Aug 2;7(2):322-328. doi: 10.1093/jhps/hnaa023. PMID: 33163218; PMCID: PMC7605777.
- Dora C, Houweling M, Koch P, Sierra RJ. Iliopsoas impingement after total hip replacement: the results of non-operative management, tenotomy or acetabular revision. J Bone Joint Surg Br. 2007 Aug;89(8):1031-5. doi: 10.1302/0301-620X.89B8.19208. PMID: 17785740.
- Lewis CL. Extra-articular Snapping Hip: A Literature Review. Sports Health. 2010 May;2(3):186-90. doi: 10.1177/1941738109357298. PMID: 23015936; PMCID: PMC3445103.
- Chalmers BP, Sculco PK, Sierra RJ, Trousdale RT, Berry DJ. Iliopsoas impingement after primary total hip arthroplasty: Operative and nonoperative treatment outcomes. J Bone Joint Surg Am. 2017 Apr 5;99(7):557-564. doi: 10.2106/JBJS.16.00244. PMID: 28375888.
- Shapira J, Chen SL, Wojnowski NM, Lall AC, Rosinsky PJ, Maldonado DR, Domb BG. Outcomes of nonoperative management, iliopsoas tenotomy, and revision arthroplasty for iliopsoas impingement after total hip arthroplasty: A Systematic Review. J Arthroplasty. 2019 Sep;34(9):2184-2191. doi: 10.1016/j.arth.2019.04.067. Epub 2019 May 8. PMID: 31147246.
- Coulomb R, Nougarede B, Maury E, Marchand P, Mares O, Kouyoumdjian P. Arthroscopic iliopsoas tenotomies: a systematic review of surgical technique and outcomes. Hip Int. 2022 Jan;32(1):4-11. doi: 10.1177/1120700020970519. Epub 2020 Nov 23. PMID: 33226846.
- Walczak BE, Blankenbaker DG, Tuite MR, Keene JS. Magnetic Resonance Imaging appearance of the hip musculature after arthroscopic labral-level iliopsoas tenotomies. Orthop J Sports Med. 2017 May 25;5(5):2325967117707498. doi: 10.1177/2325967117707498. PMID: 28596974; PMCID: PMC5448789.
- Brandenburg JB, Kapron AL, Wylie JD, Wilkinson BG, Maak TG, Gonzalez CD, Aoki SK. The functional and structural outcomes of arthroscopic iliopsoas release. Am J Sports Med. 2016 May;44(5):1286-91. doi: 10.1177/0363546515626173. Epub 2016 Feb 12. PMID: 26872894.
- Hain KS, Blankenbaker DG, De Smet AA, Keene JS, Del Rio AM. MR appearance and clinical significance of changes in the hip muscles and iliopsoas tendon after arthroscopic iliopsoas tenotomy in symptomatic patients. HSS J. 2013 Oct;9(3):236-41. doi: 10.1007/s11420-013-9361-9. Epub 2013 Aug 21. PMID: 24426875; PMCID: PMC3772171.
- Peters C, Chancellor M, Flores H, Wise A, Garrett M, Checketts J, Hanson C, Vassar M. Harms reporting is inadequate in systematic reviews regarding hip arthroscopy. Arthrosc Sports Med Rehabil. 2023 Jan 9;5(1):e75-e85. doi: 10.1016/j.asmr.2022.10.010. PMID: 36866301; PMCID: PMC9971868.
- Gouveia K, Shah A, Kay J, Memon M, Simunovic N, Cakic JN, Ranawat AS, Ayeni OR. Iliopsoas tenotomy during hip arthroscopy: A systematic review of postoperative outcomes. Am J Sports Med. 2021 Mar;49(3):817-829. doi: 10.1177/0363546520922551. Epub 2020 Jul 6. PMID: 32628861.
- Sansone M, Ahldén M, Jónasson P, Swärd L, Eriksson T, Karlsson J. Total dislocation of the hip joint after arthroscopy and ileopsoas tenotomy. Knee Surg Sports Traumatol Arthrosc. 2013 Feb;21(2):420-3. doi: 10.1007/s00167-012-2300-3. Epub 2012 Nov 22. PMID: 23179452.
- Lewis CL, Sahrmann SA, Moran DW. Effect of position and alteration in synergist muscle force contribution on hip forces when performing hip strengthening exercises. Clin Biomech (Bristol, Avon). 2009 Jan;24(1):35-42. doi: 10.1016/j.clinbiomech.2008.09.006. Epub 2008 Nov 22. PMID: 19028000; PMCID: PMC2677193.