Gluteal Overactivity – the quest for Goldilocks Glutes – Part 2
Optimal gluteal function is often seen as the holy grail of hip rehabilitation, but can you have too much of a good thing? Last month we talked about gluteal underactivity and the key underlying reasons for poor gluteal activation. This month we're going to explore gluteal overactivity and key reasons why some people struggle to turn off their glutes. These people are sometimes referred to as 'butt grippers' - is this nature or nature? With most things in life, balance usually provides best outcomes, particularly in the longer term - not too little, not too much - this is our quest for Goldilocks Glutes! But don't worry, it's not that hard, we just need to have an awareness of factors that might be confounding our efforts to upregulate gluteal response (discussed last month), while avoiding inefficient and sometimes painful extremes of activity.
First, a note about muscle excitation, activation, force and effects
Muscle activation is best defined as 'the active state of a muscle, ranging from 0% (all fibers inactive) to 100% (all fibers active).'1 Electromyography (EMG) is often used to infer level of muscle activation, force production and potential for muscle size and strength adaptations, based on amplitude of EMG signals. However the relationship between these entities is complex and direct inferences should be regarded with caution. EMG is a measure of muscle excitation, a reflection of the electrical activity that occurs during initial depolarisation, when the messages are received from the efferent/motor neuron. Because there are other steps between depolarisation and mechanical activation of a muscle fibre, the relationship between EMG amplitude and muscle activation is not entirely linear. Excitation and activation are of course closely linked, and we would expect greater activation to be linked with higher levels of excitation. However, the relationship between EMG levels, force production and propensity of an activity or exercise to induce change in strength or size is far more tenuous.
EMG amplitude is a poor predictor of force production, which is strongly influenced by muscle size and mechanical efficiency factors such as fibre length. Furthermore, claims that selecting exercises that elicit high levels of EMG will return greater gains in muscle strength or size, has not been supported by longitudinal studies.1
Key reasons for gluteal overactivity
Now that we have that out of the way, let's talk about the key reasons for gluteal overactivity, a state where the gluteal muscles are working more than expected for a particular task.
Gluteal overactivity associated with mechanical inefficiency
One of the most common reasons for a muscle to increase its level of activation is related to mechanical inefficiency. If a group of muscle fibres is unable to output the level of force required for a particular task, higher levels of activation will allow for mechanical contribution from a greater number of muscle fibres. Mechanical inefficiency may be the result of a number of factors, including fibre size and/or number, and lever arm/length-tension relationships associated with morphology or joint position.
Gluteal overactivity associated with muscle atrophy
An atrophied muscle will have undergone a reduction in size of muscle fibres and/or death of some fibres, resulting in reduced physiological cross-sectional area. With less and/or smaller fibres, the capacity for mechanical force production is reduced, resulting in a weaker muscle. Assuming all other factors are equal, an atrophied muscle will necessarily need to employ more fibres than a healthy muscle to perform the same task, therefore increasing it's relative level or duration of activation. This may be one explanation for greater and/or more sustained excitation of segments of the gluteus medius and minimus muscles during gait, recorded in those with gluteal tendinopathy compared with painfree control participants.2,3 In these populations, such alterations in muscle excitation (EMG) coexist with gluteal atrophy4 and hip abduction weakness.3,5
Gluteal overactivity associated with bony morphology
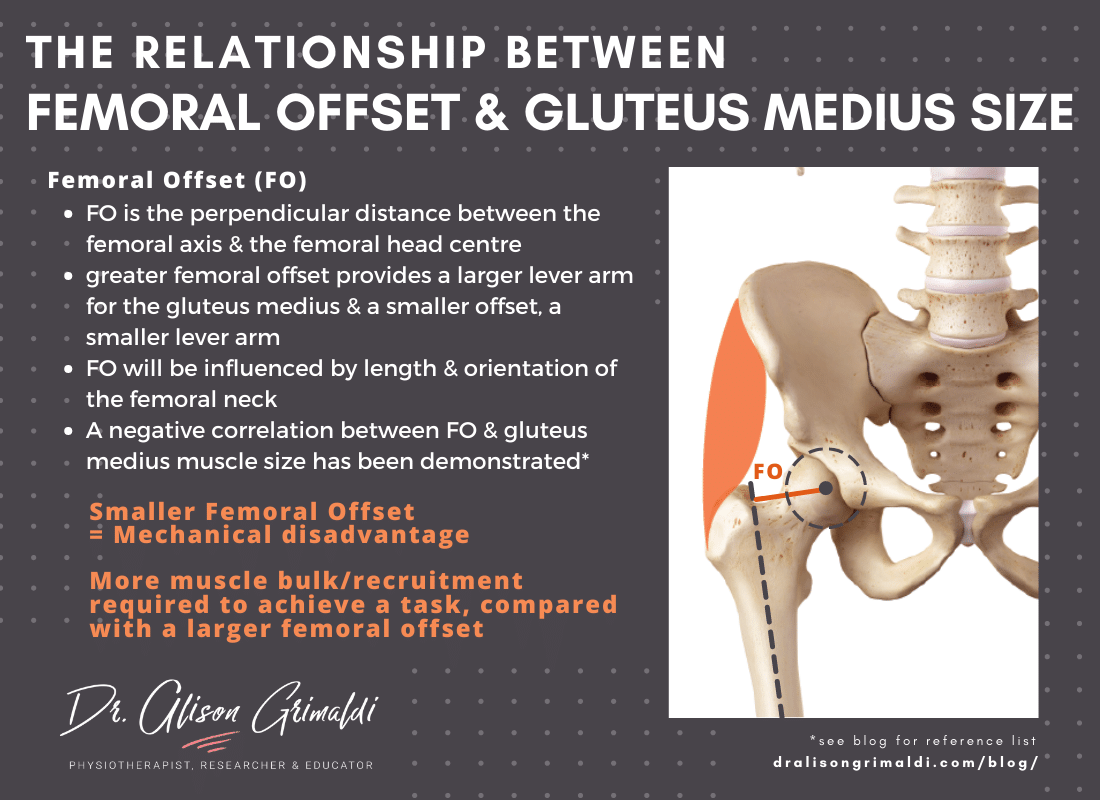
Sometimes a muscle has to work harder due to a lever arm disadvantage imposed by innate or acquired morphology. For example, the length and orientation (neck-shaft angle) of the femur will influence the femoral offset (see illustration below) and the lever arm of the gluteus medius and minimus muscles. Research has demonstrated a negative correlation between femoral offset and gluteus medius muscle size,6 indicating that if you have a greater lever arm advantage (greater femoral offset), you won't need to work the gluteus medius as hard, resulting in smaller bulk. Conversely, the mechanical disadvantage imparted by a smaller femoral offset, will require greater effort from the gluteus medius to perform the same task, such as standing on one leg. Smaller offset may be related to coxa breva (short neck) or coxa valga (more vertically oriented femoral neck), or may be acquired after total hip replacement associated with the femoral component selected.
A mechanical disadvantage will mean higher muscle activation and/or bulk will be required to perform a particular function. A combination of muscle weakness, atrophy and a smaller lever arm may result in necessary muscle upregulation or overactivity. Alternatively, you might see compensatory strategies to shift the load elsewhere - for example ipsilateral trunk lean in single leg stance - moving the centre of mass over the hip to reduce load on the hip abductors. However, such offloading strategies will of course result in further weakness and atrophy.
If overactivity is related to a morphological mechanical disadvantage, then the aim would be to build muscle size and strength to allow the force to be generated more efficiently with fewer fibres.
Gluteal overactivity associated with joint position
All muscles have a ‘sweet-spot’ – a range in which the length-tension relationship is optimal and they can generate greatest force. This is generally through the mid-range, with mechanical inefficiency occurring at either extreme of range where the muscle is maximally shortened or lengthened. This can be visualised as a curve with peak force production capacity at optimal fibre length, gradually dropping to 0 at either extreme of muscle fibre length. So, at optimal fibre length which we will denote as 1, a force that can be generated with 60% activation will require 70% activation at a relatively shorter length of around 0.8 or a relatively longer length of around 1.2.1
If we put this into the context of an exercise task for the lower (extending) fibres of gluteus maximus, the muscle will need to work much harder to generate force in a prone hip extension task (inefficient shortened fibre length) than in the mid ranges of a squat, where fibre length will be more optimal. An investigation of the influence of range of hip flexion on lower-extremity muscle activity and torque output, found that gluteus maximus excitation (EMG) levels were significantly higher and torque production was significantly lower at 0 degrees compared with 90 degrees of hip flexion.7 In prone hip extension, gluteus maximus will need to increase its activation due to the short fibre length and mechanical disadvantage and its capacity for force production will be poor.
Assumptions that any exercise that induces high levels of EMG will provide superior strength and size gains must be re-examined. High excitation or activation may simply be a reflection of mechanical inefficiency, and poorly correlated with force generation.

Gluteal overactivity associated with pain and/or injury
In last month's blog, we talked in depth about the flexible solutions the motor system uses to adapt to pain or injury, either or concurrently downregulating or upregulating muscle excitability and activation, with a primary purpose to reduce pain and protect the painful region.
Muscle overactivity may in some circumstance then be a response to pain or the nervous system’s attempt at protecting an injured body part or an area perceived to be at risk. High levels of muscle activity might be put in place to protectively ‘splint’ an area.
Gluteal overactivity related to excess stimulus
There are reasons for gluteal overactivity that are linked to increased stimulus related to the effects of gravity, type of training or high levels of volitional recruitment.
Specific gravitational effects on gluteal muscle activity
Last month, we discussed the intimate relationship between the positioning of the trunk centre of mass and gluteal recruitment in upright weightbearing function. If you think of the hip joint centre as the fulcrum for force transmission of the hip, the further the centre of mass of the trunk moves away from a position vertically above the hip, the greater the demand on structures opposing the direction of movement to control that moment or force.
In those that you identify with inefficiently high gluteus maximus activity in quiet bilateral stance, take a close look at their trunk and pelvic position. If the trunk is leaning even slightly forward, the hip extensors will need to increase their activity to resist the force of gravity. Hyperlordosis may have a similar effect. Higher EMG levels and earlier recruitment of gluteus maximus have been reported during dynamic weightbearing activity in those with hyperlordosis.8 Higher levels of natural gravitational stimulus is likely one of the key reasons that those with a lordotic posture type generally have better gluteus maximus bulk. Higher levels of activation are of course only an issue if this becomes inefficient, fatiguing and painful - for example, high levels of tonic gluteal activity during quite standing associated with limited standing tolerance, pain and fatigue in the buttock and/or lower back.
In such cases, modifying underlying drivers of trunk forward lean or excessive anterior pelvic tilt, together with retraining habitual loading habits, may assist with reducing gluteal overactivity and any associated adverse effects.
Gluteal overactivity related to type of training
Type of training may in some circumstances also alter natural gluteal recruitment habits. We have evolved to be innately very efficient beings, programmed in optimal circumstances to use only what energy and levels of muscle activation are required to perform the desired task. When moving in a particular plane of motion, the muscles that have the best lever arm advantage will generally be primarily responsibly for creating that action. Other muscles play supportive roles, such as in reducing motion in other planes to optimise force transmission in the primary line of action.
For example, when performing a sagittal plane action such as a bodyweight bilateral squat or bridge, the gluteus medius, with primary function in the frontal plane, will be recruited at a relatively low level of around 20-30% of a maximal voluntary isometric contraction.9 The muscle segments and fibres responsible for this secondary control of femoral position will naturally change through sagittal range to allow efficiency and load sharing.

So, what is the rationale for placing bands around the knees and requesting high effort recruitment of frontal and axial plane muscles, during a sagittal plane task? Presumably to increase abductor/external rotator muscle recruitment with the aim of enhancing strength gains in these secondary muscles.
Is there proof that this is a superior manner to induce such changes? No.
Do we risk training the motor system to inefficiently over-recruit secondary musculature? Possibly
Do we increase risk of pain/injury due to excessive co-contraction and loss of normal load sharing-load sparing? Possibly
If the goal is to increase strength or hypertrophy of a target muscle, loading in its primary line of action is likely to allow greater force production and mechanostimulus. If the goal is to enhance functional capacity in a task such as a squat, there are many ways to increase task challenge while still maintaining relative efficiency – i.e. only using what you need, when you need it. Much further research is required to tease out and test all these assumptions. In the meantime, we should consider the multifaceted nature of the motor system and how we can best achieve a desired outcome, without inadvertently inducing an accompanying adverse effect.
Excess volitional recruitment
Along the same lines, we need to ensure we are also considering normal efficient function when we use conscious cues to upregulate muscle recruitment. I have seen many patients who have actually trained themselves to maintain tonic activity in their glutes, as this is what they had interpreted their health or exercise professional or 'Dr Google' to have recommended. Of course this is highly inefficient and may feed into many lumbopelvic-hip pain presentations. Wherever possible, if we can stimulate the recruitment we think necessary through body position, exercise selection and external cues, we may reduce the risk of these situations. Or, use conscious cues in early rehabilitation and reduce reliance on cues through rehabilitation and occupy the brain with other tasks to optimise feedforward motor planning.
Fear & Beliefs
As with gluteal underactivity, fears and beliefs can be potent drivers of gluteal overactivity. Overactivity in this case is most commonly related to fears and beliefs around stability of the sacroiliac or hip joints. Unhelpful beliefs around pelvic instability may drive gluteal upregulation and fears around stability of the hip joint may occur in those with acetabular dysplasia, ligamentous laxity or even lateral snapping hip. Many people believe that the ITB snapping across the greater trochanter is their hip dislocating or subluxing. Education and reassurance is key in our management plans.
In some cases of true structural deficiency the fears may have some basis, but our education needs to be thoughtful to avoid unnecessary stress, limitations in activity and quality of life. Our aim will be to optimise dynamic stability mechanisms but without inducing unhelpful rigidity and overload, which in itself may become painful and fatiguing.
Read more in last months blogs about the impact of unhelpful fears and beliefs.
The quest for Goldilocks Glutes
A summary of the considerations for understanding and managing gluteal overactivity:
- High levels of muscle recruitment in those with weakness and atrophy is likely related to small/lower numbers of muscle fibres – use targeted loading to hypertrophy those fibres for optimal efficiency.
- Consider lever arm disadvantage – compensate for morphological disadvantage by optimising other aspects such as size and strength.
- Use joint angle and gravitational loading to optimize gluteal efficiency.
- Reducing pain and addressing fears and unhelpful beliefs will help reduce excessive protective responses.
- Be mindful of the effects of volitional cues and exercise technique, not only on recruitment, but on efficiency and loading of associated structures.
- Decide on your goals and consider the best way to achieve them without inducing unintended adverse effects.
I hope the information in this 2-part blog series has been helpful and I wish you all the best in your quest for Goldilocks Glutes!
Been enjoying the content on this site?
Thank you for visiting this page. If you found the information valuable, I would appreciate your positive comments and 5-star review on my google page. If you have any other feedback you would like to provide, you can contact me here.
Learn more about hip muscle function, musculoskeletal loads and how we can optimise these in the rehabilitation of hip, groin and buttock pain. Multiple sessions to suit a wide range of timezones.
Anterior Hip & Groin Pain 29-30 May 2021 - Registrations close April 18th
Lateral Hip & Buttock Pain 12-13 June 2021 - Registrations close May 2nd
Sign up to our newsletter to receive updates on upcoming courses, news and special offers.
References



