Injections for hip pain: options, benefits, risks

There are a number of different injections for hip pain that may be offered for various reasons. While there can be meaningful benefits, it’s important to be aware of the limitations of what injections can provide and the inherent risks. For each individual, health professionals should consider the options, benefits and risks of injections for hip pain and discuss these with the patient in a shared decision-making process.
Injections for hip pain may be intra-articular (injected into the hip joint), or extra-articular – most commonly injected around tendons. Injections may be used for diagnostic purposes or to reduce hip pain and disability. With regard to therapeutic benefits, injections generally only provide short-medium term relief. When using injections for hip pain, education should therefore be included around optimising outcomes by pairing injection with more active styles of intervention such as exercise therapy and load management education.
Where in the management journey injections fit should also be closely considered. Injections are commonly offered in primary care as first-line management for hip pain, although this is not strongly supported by the evidence and may carry substantial risks. Let’s explore what we know to date.
Here are the primary topics we’ll be talking about in this blog:
Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.
General risks of injections for hip pain
Adverse events for hip injections range from mild to more severe events. Risks of injections for hip pain may be related to the substance injected, but infection or iatrogenic tissue damage may occur simply due to the process of inserting a needle into the hip joint or extra-articular soft tissues. These risks are low but do occur, so we will cover these first. Then we'll go on to discuss specific injections for hip pain - options, benefits and risks.
Options, benefits and risks of intra-articular hip injections
Various injections are used by health professionals in the diagnosis and management of hip joint related pain. The most common injections include local anaesthetics and corticosteroid injections, with more recent entry of viscosupplementation with hyaluronic acid, and platelet rich plasma injections. Let’s take a look at the indications, mechanisms, benefits and adverse issues associated with these hip injection options.
Local anaesthetic injections into the hip joint
Indications and benefits of intra-articular local anaesthetic injection into the hip joint
Intra-articular local anaesthetic injections for the hip are most commonly used for diagnostic purposes. This may be indicated where a surgical intervention is being considered. If there is no change in symptoms while the anaesthetic is active, other diagnoses and treatments may be considered, or the patient may be counselled that the chances of a good outcome from surgery are likely to be reduced.
One recent prospective study asked patients with suspected hip joint related pain to perform a battery of provocative functional tests (treadmill walking, lateral step down, agility box drill, hop tests) before and after an intra-articular local anaesthetic injection. Outcomes of 90 patients who subsequently underwent arthroscopic surgery were tracked over 12 months. Those who experienced less than 75% improvement in their pain during the battery of provocative functional tests experienced poorer outcomes that those who reported 75% or more improvement in symptoms during pre-operative testing.6
Local anaesthetic is also often added to intra-articular corticosteroid injection, to assess immediate effect of the intra-articular injectate.
For diagnostic purposes, it is important that the injectate is accurately placed within the hip joint and does not leak substantially outside the hip joint. Malposition or extravasation into extra-articular tissues will reduce diagnostic accuracy, as positive effect may be due to effects on extra-articular tissues. In around 15% of people the hip joint communicates with the psoas bursa,7 so an intra-articular anaesthetic injection may reduce pain associated with the psoas bursa.
Possible risks of intra-articular local anaesthetic injection into the hip joint
Scientific studies have shown that local anaesthetics such as lidocaine and bupivacaine are chondrotoxic – toxic to cartilage cells. Local anaesthetics can affect chondrocyte viability, inhibit matrix synthesis, and promote chondrocyte apoptosis (programmed cell death).
The extent of this impact varies depending on the specific local anaesthetic agent, concentration and exposure duration.
In general, it has been reported that:
- lidocaine and bupivacaine are most chondrotoxic
- greater concentrations of lidocaine and bupivacaine (i.e., 2% vs 1% and 0.5% vs 0.25%) are more toxic to chondrocytes, and
- greater exposure is more toxic.
Cartilage exposure to local anaesthetic for > 1 hour has shown to result in significant adverse effects on chondrocytes in vitro. The half-life of common local anaesthetics ranges from 1.6 - 3.5 hours, with bupivacaine having the longest half-life at 3.5 hours.8
Longer exposure times may also be related to an indwelling, intra-articular catheter which is sometimes left in the joint for a period to provide pain-relief post-operatively. This has the potential to create much greater cartilage toxicity that a single intra-articular injection.9,10 In fact, chondrolysis – complete destruction of joint cartilage – has been reported in some people after use of intra-articular local anaesthetic pain pumps following shoulder and knee arthroscopy.8
Furthermore, the effect of mixing injectates needs to be considered. The addition of corticosteroids to a local anaesthetic injection appears to worsen the chondrotoxic effects.9,10 This combination (LA-CSI) is common in intra-articular hip injections.
Based on current evidence, intra-articular local anaesthetics should be used judiciously, with lowest possible concentrations and exposure. Ropivacaine and mepivacaine have been recommended over bupivacaine and lidocaine as they are less toxic for cartilage.8

Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.

Corticosteroid injections into the hip joint
Indications, mechanisms and benefits of corticosteroid injection into the hip joint
Corticosteroid injections, also known as cortisone injections, are frequently used to manage pain and reduce inflammation in the hip joint. Corticosteroids, such as methylprednisolone or triamcinolone, have potent anti-inflammatory and immunosuppressive properties.11
Corticosteroids interrupt the inflammatory and immune cascade at several levels. They reduce vascular permeability, inhibit accumulation of inflammatory cells and prevent the synthesis and secretion of several inflammatory mediators such as prostaglandin and leukotrienes.11
Intra-articular injection of corticosteroid has traditionally been used more commonly in the management of hip osteoarthritis, but in recent years there seems to have been an increased use of injectables in younger patients with femoroacetabular impingement, dysplasia and labral tears.
Many studies have found short-term pain-relieving effects of corticosteroid injection for those with hip osteoarthritis. A recent systematic review and network meta-analysis on intra-articular hip injections reported that corticosteroids are the most effective hip injection in the short-term (1 month), but any benefit is usually lost in the medium to long term (3 months or greater).12
Another recent systematic review and network meta-analysis of RCTs that included placebo intra-articular saline injections, found that for both pain and functional outcomes of intra-articular injection for hip osteoarthritis, no intervention (including corticosteroid) significantly outperformed a placebo injection at up to 6 months. Interestingly, changes from baseline did surpass the minimal clinically important differences for both corticosteroid and placebo injection, which does reduce clarity around the mechanism of effect.13
A further systematic review and meta-analysis of non-operative outcomes for non-arthritic hip pain (e.g., femoroacetabular impingement syndrome, acetabular dysplasia, acetabular labral tear) found little evidence for intra-articular corticosteroid use in non-arthritic patients. They reported very low certainty evidence of reduced pain and improved function for up to 12 weeks.14
So, while there is evidence that intra-articular cortisone injections may assist in reducing pain and improving function for those with hip osteoarthritis, these effects are short-lived and need to be weighed against potential risks. The evidence for the use of intra-articular corticosteroids in those with non-arthritic hip pain is currently weak, with arguably greater concerns around the following adverse effects.
Possible risks of intra-articular corticosteroid injection into the hip joint
Scientific studies have reported several adverse effects of intra-articular corticosteroid injections, including cartilage damage, avascular necrosis and infection of the native joint and a subsequent prosthesis.
Corticosteroids, chondrotoxicity, avascular necrosis and rapidly destructive osteoarthritis
As with local anaesthetic injections, in vitro and animal in vivo studies have shown that corticosteroids have a toxic effect on cartilage cells, resulting in significant chondrotoxicity and cell death.15 The effect is even greater when the cortisone is paired with local anaesthetic,9,10 which is common in clinical practice. Corticosteroids are also toxic to bone cells and high dose oral steroids, or repeated intra-articular injections may increase the risk of avascular necrosis of the femoral head.
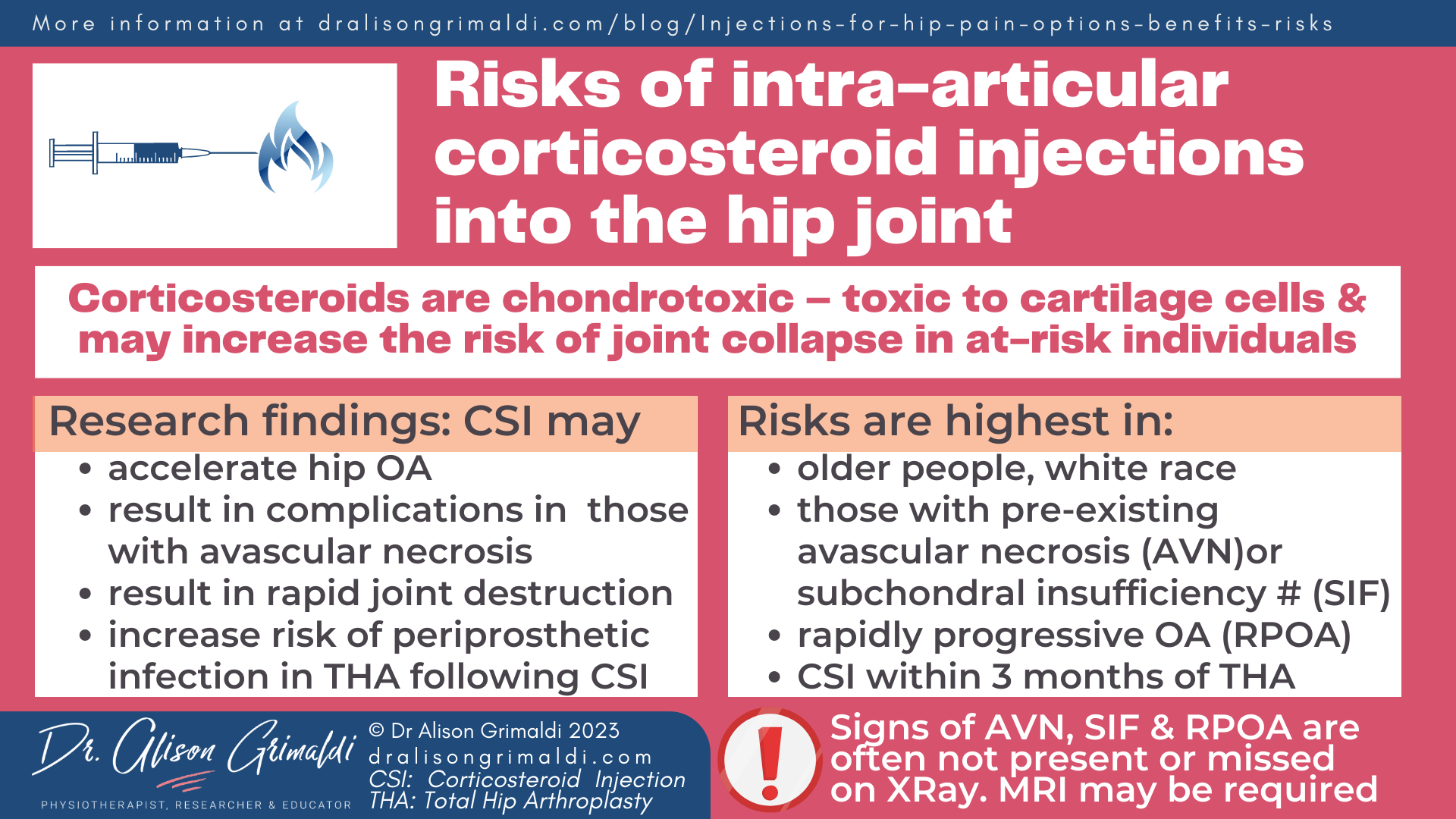
A study by Kompel and colleagues in 2019 caused concern when they reported four main adverse joint findings observed in patients following intra-articular corticosteroid injections of the hip: accelerated osteoarthritis progression (6%), subchondral insufficiency fracture (0.9%), complications of avascular necrosis (osteonecrosis) (0.7%), and rapid joint destruction, including bone loss (0.7%).16
Another 2019 study performed blinded reviews of repeat radiographs of patients who either had or had not had intra-articular hip cortisone injections. Progression of OA over 3-12 months was evident in 24% of those who had not had injection and 44% of those who had undergone cortisone injection. In addition, joint collapse occurred in only 1% of those without injection and 17% post injection.17
Kompel and colleagues found that serious adverse events after corticosteroid injection were more likely to occur in those with pre-existing avascular necrosis, subchondral insufficiency fracture or very early stages of rapidly progressive hip OA.16
Another recent retrospective study found that if those with pre-existing avascular necrosis and subchondral insufficiency fracture are excluded from analysis, patients treated with hip CSI did not have significantly higher rates of short-term hip OA progression or femoral head articular surface collapse.18
So, it seems that it is critical that patients with these pre-existing risk factors are picked up prior to intra-articular corticosteroid injection. Subchondral insufficiency fracture and osteonecrosis can sometimes be diagnosed by using radiography, although the changes may be subtle or not visible on Xray. These risk factors are therefore often unfortunately easily missed.
RISK FACTORS TO BE ON THE LOOKOUT FOR:
Those who are likely to be at risk of more severe adverse effects after intra-articular corticosteroid injection:
- older age, white race
- those with pre-existing avascular necrosis
- secondary to trauma & injury to blood supply – femoral neck # or dislocation
- non-traumatic insidious onset of pain, with possible history of
- long-term oral steroid use
- long-term alcohol abuse
- radiation treatments or chemotherapy
- other health conditions - blood disorders, autoimmune disorders, HIV etc
- those with pre-existing subchondral insufficiency fracture
- older adult with osteoporosis
- younger adult who is active
- acute pain, which gradually worsens for weeks without an identifiable incident
- ultrasound findings such as a larger-than-expected joint effusion, extensive intraarticular debris, or synovial thickening, indicating an active joint process
- those with a rapidly progressive form of osteoarthritis.16
SCREENING:
If pain is high enough to refer for CSI, an Xray or ultrasound may be warranted prior to the injection. If there is no -minimal joint change evident on XRay with high pain levels, an MRI may be indicated to rule out insufficiency fracture, and check for early indicators of rapidly progressive hip OA (joint effusion, synovitis, adjacent soft-tissue changes, subchondral bone marrow oedema). MRI is also helpful to better detect avascular necrosis (osteonecrosis) of the femoral head.
It is important that these risk factors are considered closely. Corticosteroids will interfere with bone healing, and decreased joint pain may allow increased weightbearing, together leading to possible bone and joint collapse in those with insufficiency fracture, avascular necrosis or rapidly progressive hip OA.
Corticosteroids and infection of the native or prosthetic hip joint
Intra-articular corticosteroid injections carry a risk of joint infection and septic arthritis, although this risk is very low with appropriate hygiene procedures and screening of patients with skin infections or predisposing dermatological conditions.
Of more concern is the possible increased risk of peri-prosthetic infection in those who have had a recent intra-articular cortisone injection pre-operatively. The immunosuppressive effects of corticosteroids may not only increase risk of infection, but also inhibit osteointegration of the cementless prosthesis early in the postoperative period.19
Peri-prosthetic joint infections +/- lack of osteointegration can be devastating, leading to early joint revision surgery with poorer outcomes and much higher rates of post-operative complications and higher costs.
Two 2023 systematic reviews with meta-analysis have both found that patients receiving pre-operative corticosteroid injections in the 3 months prior to total hip arthroplasty had a significantly higher risk of developing peri-prosthetic infection. Both recommended that patients requiring total hip replacement surgery should wait at least 3-months following intra-articular corticosteroid injection to reduce postoperative infection risk.20,21
This finding makes it even more important that patients are adequately screened for risk factors that may result in rapid joint destruction following corticosteroid injection. For those who do experience such adverse events, if a rapid progression to surgical joint replacement is required, they are then at additional risk of developing a peri-prosthetic infection.
Considering the potential for chondral damage and this devastating sequalae of events, it may be wise to first consider alternative interventions for joint related hip pain. When injections are used, careful screening for those with no-mild OA and pre-operative planning for those with later stage OA (no injection within 3 months of planned surgery) is advisable.
Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.
Viscosupplementation injections into the hip joint
Indications, mechanisms and benefits of Viscosupplementation injections into the hip joint
Viscosupplementation involves intra-articular injection of hyaluronic acid. Hyaluronic acid is a naturally occurring substance found in the synovial fluid of joints. It is a high-molecular-weight glycosaminoglycan that plays a key role in maintaining joint lubrication, and viscosity and shock-absorbing properties of synovial fluid.
In recent years, viscosupplementation has gained popularity as a treatment option for hip osteoarthritis and even in the management of hip joint related pain in younger individuals. Hyaluronic acid is produced either from harvested rooster combs or via bacterial fermentation in vitro.11 Common brand names include Durolane, Synvisc, Monovisc and Euflexxa.
Inflammation associated with osteoarthritis results in increased synovial membrane permeability to hyaluronic acid. Elevated levels of inflammatory cytokines, free radicals, and proteolytic enzymes in osteoarthritic joints also interfere with normal hyaluronic acid function and contribute to the progression of OA. These inflammatory processes then result in both reduced concentration and reduced molecular weight of naturally occurring hyaluronic acid.11
The fluid itself is viscous when injected and it is thought that viscosupplementation temporarily restores the viscoelastic properties and therefore the lubricating and shock-absorbing effects of the synovial fluid. Additional effects have been suggested, including reduction of synovial inflammation, protection against cartilage erosion and stimulus of endogenous hyaluronic acid production, although these effects are not well established.11
Hyaluronic acid also has 2 potential mechanisms for providing pain relief – an indirect mechanism via its anti-inflammatory properties and a direct effect through inhibition of nociceptors and synthesis of bradykinin and substance P.11
Despite the promise of these potential mechanisms of effect, the evidence is varied for hyaluronic acid with some studies reporting no effect and others reporting some positive gains in the short-medium term. A 2020 meta-analysis found that hyaluronic acid reduced pain more than a control injection (usually saline) at 1 and 3 months, but not at 6 months. Corticosteroid injection was more effective than hyaluronic acid at the 1-month time point.22
In terms of functional benefits, at 2 months post injection hyaluronic acid was superior to a control injection and equal to corticosteroid injection in terms of improvements in WOMAC scores. A 2023 review found injection protocols varied but overall, hyaluronic acid injections into the hip for osteoarthritis led to improvements in pain and to a lesser degree, function, and reduction in oral use of anti-inflammatories (very low to low certainty evidence).23
Effects are often more delayed than those seen with local anaesthetic and corticosteroid, generally expected to occur after a few weeks. However, improvements have been reported as early as 2 weeks and, in some cases, last up to 12-months post injection.23
Possible risks of intra-articular Viscosupplementation injections into the hip joint
Unlike local anaesthetics and corticosteroid, hyaluronic acid is not toxic for cartilage cells. It is safe for use in patients with osteoarthritis, with the only significant adverse effects reported being transient local reactions in the injected joint in 2% to 4% of people.11 However, sometimes corticosteroid is added to the hyaluronic acid injection. This will carry with it the risk associated with corticosteroid injection.

Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.
Platelet rich plasma injections into the hip joint
Indications, mechanisms and benefits of Platelet Rich Plasma injections into the hip joint
Platelet Rich Plasma (PRP) injections gained popularity quickly as a treatment modality in many different joints and soft tissues around the body. This popularity waned somewhat when systematic reviews showed little – no benefit and government funding was removed in different countries for this intervention. However, PRP continues to be a treatment option, even if privately funded, and there is some evidence for its usefulness in hip osteoarthritis.
PRP is prepared by extracting a small sample of the patient's blood and subjecting it to a centrifugation process to separate the platelets from other blood components. The resulting PRP solution contains a high concentration of platelets, growth factors, cytokines, and other bioactive molecules that are thought to facilitate tissue healing. One of the issues is that the literature includes a variety of different preparations or concentrations of different blood elements, making conclusions about PRP as a treatment more difficult.
Platelets play an important role in the healing process by initiating and coordinating tissue repair. When injected into an injured or degenerated area, it is hypothesized that the growth factors and other bioactive molecules released by platelets will promote cell proliferation, collagen synthesis, angiogenesis, and tissue regeneration, thereby accelerating healing and reducing pain and inflammation. Animal studies have shown positive bone and cartilage changes in response to PRP, but there is a lack of similar evidence in human participants.
Reviews of the evidence for PRP as a treatment for hip osteoarthritis reports limited evidence of:
- superior pain relief following PRP at 6 months compared with cortisone and hyaluronic acid
- positive effects on function (WOMAC) at 3 months, but only when combined with hyaluronic acid23
Overall, there is variability in procedures, PRP preparation and results, with a lack of clear and reproducible positive results. Despite the enticing promise of cartilage and bone healing, such effects have not yet been established and PRP is currently still not recommended in any guidelines for management of hip OA or hip related pain, due to the inadequate evidence regarding clinical efficacy.11,22,24
Possible risks of intra-articular Platelet Rich Plasma injections into the hip joint
PRP injections are generally considered safe, as they utilize the patient's own blood components. Only mild adverse events have been reported including temporary joint pain and swelling.11

Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.
Options, benefits and risks of extra-articular hip injections
Extra-articular injections are also used for diagnosis and management of various conditions around the hip, most commonly for treatment of tendinopathy or ‘bursitis’, peripheral neuropathies or muscular pain related to extra-articular impingement. As for articular pain, the most common injections are local anaesthetics and cortisone, with PRP a more recent entry.

Local anaesthetic injections into the extra-articular tissues of the hip
Indications and benefits of local anaesthetic injection for extra-articular hip pain
Local anaesthetic injections into the soft tissues around the hip joint are usually used for either diagnostic purposes or pain relief. Local anaesthetic injection for diagnostic purposes should be performed under image guidance, but as extra-articular injectate can travel a significant distant, interpretation may be limited.
As local anaesthetics are generally short-acting (1.6 – 3.5 hours), when used for pain relief they are commonly combined with a corticosteroid. Even when used primarily for diagnostic purposes, corticosteroid is often combined with the local anaesthetic in the interests of achieving a dual effect – diagnosis and pain relief. The potential benefits of such injections need to be weighed against possible adverse effects on tissue health.
Possible risks of local anaesthetic injection for extra-articular tissues
Injections of local anaesthetics around tendons are regularly employed to diagnose or treat tendon pain. Similar to the effect on cartilage cells, in vitro studies have demonstrated cytotoxic effects of local anaesthetics such as lidocaine and bupivacaine on tenocytes (tendon cells).8 Effects will once again be influenced by drug selection, concentration and exposure time.
As with chondrotoxic effects, the combination of local anaesthetic and corticosteroid is likely to have greater toxic effect on tendon tissues.
Zhang and colleagues suggested that to avoid associated side effects, drugs, concentrations and exposure times should be chosen carefully when using local anaesthetics, with 0.2% ropivacaine exerting the least toxic effects on tendons.8
Local anaesthetics also have a toxic effect on muscle cells, with greater damage again linked to higher concentrations and exposure. Lidocaine, ropivacaine, and bupivacaine have been linked with myotoxicity, with effect increasing from lidocaine to bupivacaine.8
The muscle cells closest to the injection are most effected - the sarcoplasmic reticulum dissolves and degenerates, and the myocytes demonstrate oedema and necrosis within a few hours. These effects on muscle cells are completely reversible, with regeneration complete within 3-4 weeks.8 However, repeat injections at regular intervals are provided in some interventionalist pain management approaches. This may mean the area is subjected to further myotoxic anaesthetic prior to tissue recovery. The adverse impact of such injection therapy is unclear.


Corticosteroid injections into the extra-articular tissues of the hip
Indications and benefits of cortisone injections for extra-articular hip pain
Cortisone injections are regularly prescribed for soft tissue conditions around the hip, most commonly gluteal tendinopathy and associated ‘trochanteric bursitis’ (the inverted commas are due to the fact that a true inflammatory process has not been established here), and proximal hamstring tendinopathy and associated ‘ischial/ischiogluteal bursitis’.
At the anterior hip, corticosteroid injections are commonly used to try to differentially diagnose iliopsoas related versus joint related pain, and for the management of iliopsoas related pain and iliopsoas bursitis. Injections are sometimes targeted at the bursa or infiltrated around the iliopsoas tendon or in some approaches, within the tendon sheath. Corticosteroid injections are also used if the rectus femoris direct or indirect tendons of origin are suspected as a source of pain.
Use of corticosteroid injection has also been described recently for treatment of pain and inflammation of the quadratus femoris muscle in those with extra-articular, ischiofemoral impingement.25
The other most common indication for corticosteroid injection is for neuropathic pain related to peripheral nerve impingement.
Around the hip, corticosteroid injections for neuralgia are most frequently provided for:
- sciatic nerve irritation in the deep gluteal space (deep gluteal syndrome or piriformis syndrome),
- pudendal neuralgia, usually impinged in the Alcock’s canal,
- meralgia paraesthetica, associated with the lateral femoral cutaneous nerve, and
- entrapment or irritation of other smaller nerves in the groin or lower abdominal region – iliohypogastric, ilioinguinal, genitofemoral nerves.
While for many of these conditions, the evidence is only in the form of case studies/series or technique descriptions, there is a reasonable body of evidence assessing the usefulness of corticosteroid injections in management of gluteal tendinopathy.
Efficacy of Corticosteroid Injections for Gluteal Tendinopathy or Greater Trochanteric Pain Syndrome
The findings of various studies are consistent that people with gluteal tendinopathy or GTPS are likely to experience at least some benefit from corticosteroid injections (CSI) in terms of pain reduction and associated functional improvements, with greatest effect in the short-term. CSI has been shown to be superior to usual care and wait-and-see in both the short and long term, when pain severity and function are measured.26,27
However, CSI did not provide benefits over wait-and-see for Quality of Life (QOL) in either the short or longer term, or at 12 months when a global rating of change (GROC) was collected.26 One study also showed that for pain intensity, there was no significant difference between CSI and a placebo saline injection in either the short term (4 weeks) or longer term (6 months).28
When compared against a contemporary education and exercise (EDX) approach in the LEAP randomised clinical trial, EDX was significantly more successful than CSI in both the short and long term, as measured with a global rating of change score. Pain severity and constancy (% of time pain was present in the last week) in the short term, and pain constancy in the longer term were lower for the EDX group.26
QoL was also significantly more improved for the EDX group compared with the CSI group in the short and long term. So, it appears that even though CSI may still have some longer term effects on pain severity, people’s QoL and global improvement remains inferior compared to those who undertake a load management and exercise plan.26
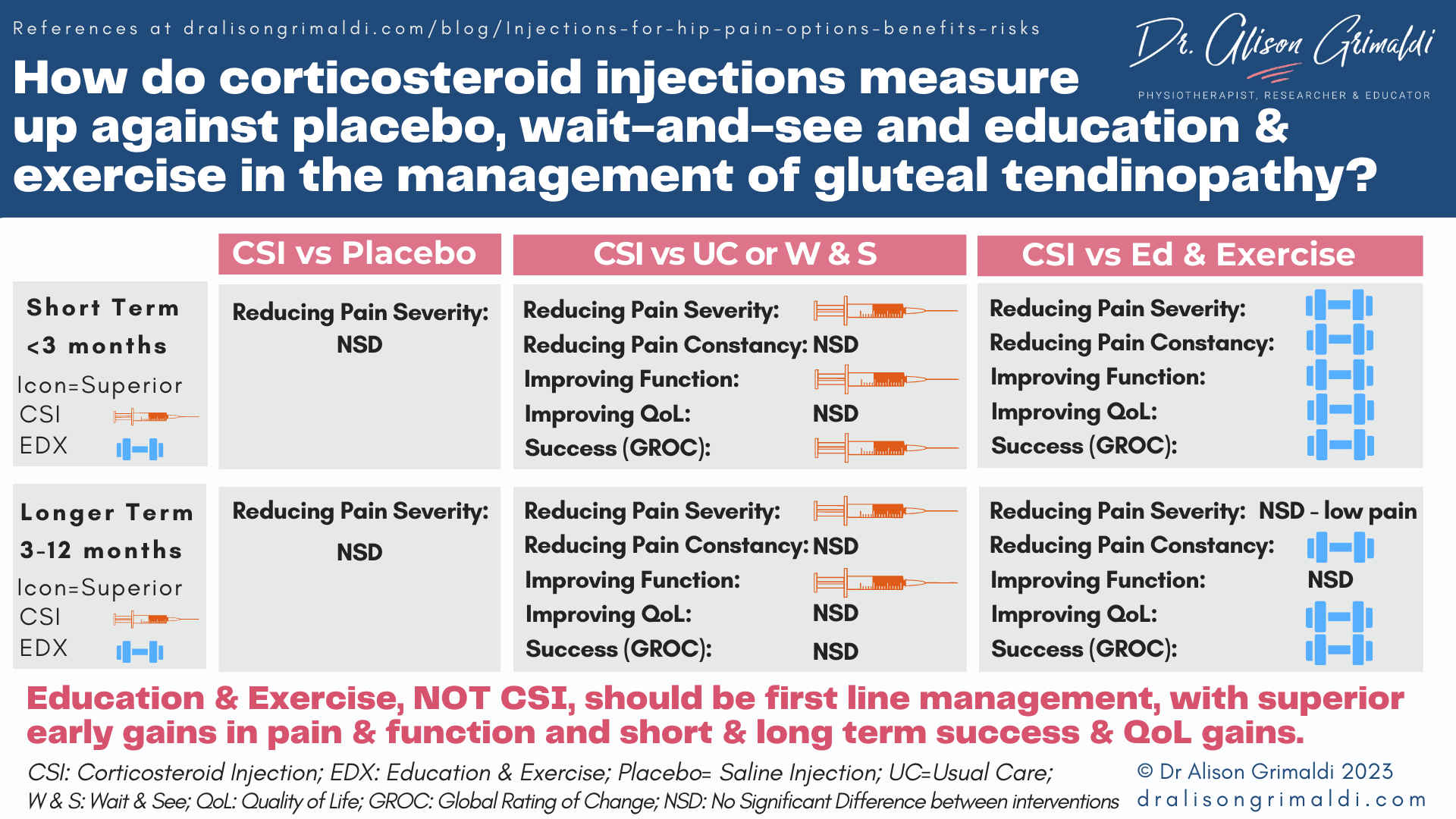
In clinical practice, the effect of corticosteroids is generally short-lived and the benefits need to be weighed up against the potential adverse effects of this potent pharmacological agent.
Possible risks of cortisone injection for soft tissues of the hip
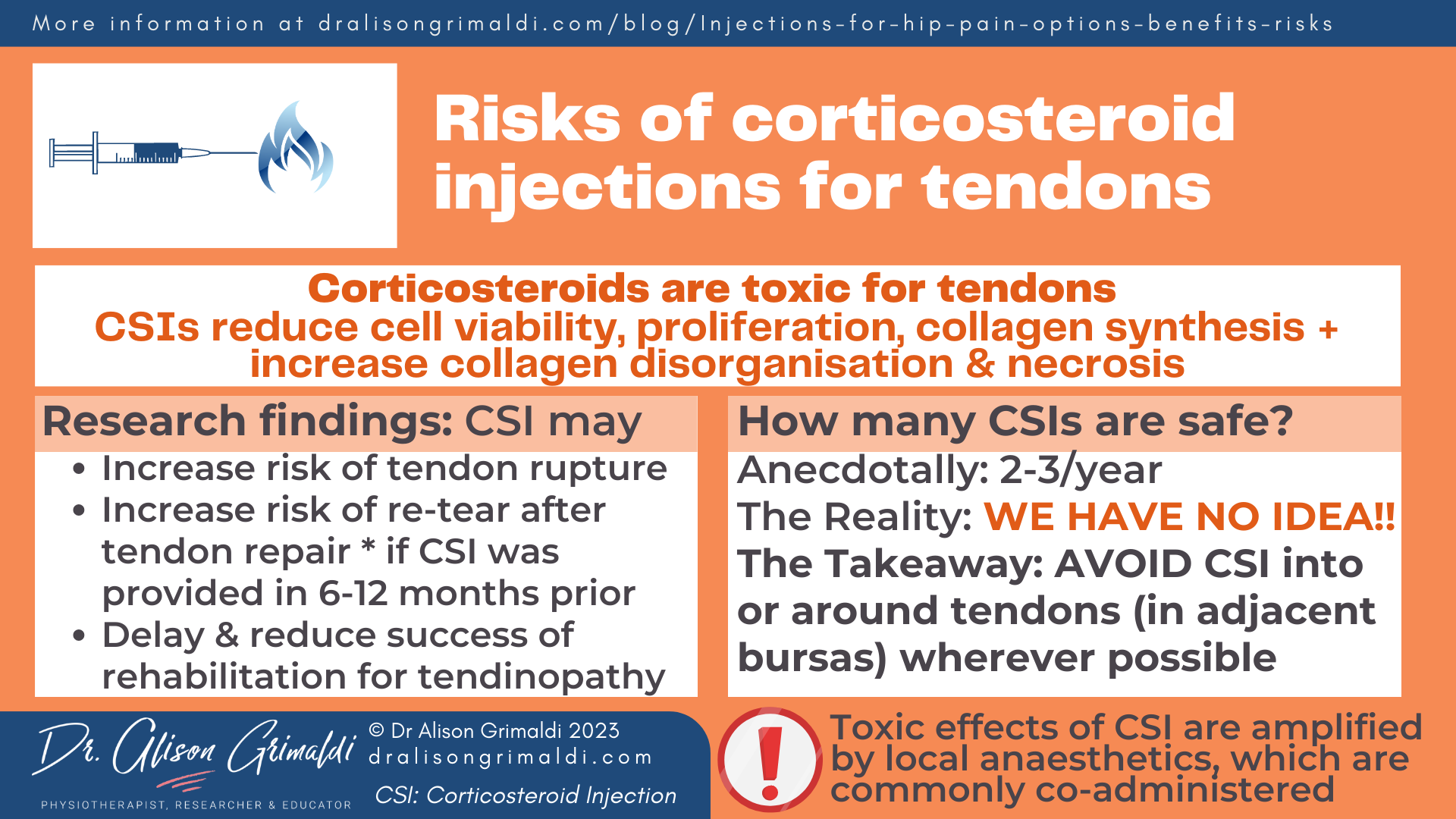
Corticosteroids are toxic for tendon cells, with potential for adverse effects on tendon health, associated with reduced cell viability, cell proliferation and collagen synthesis, as well as increased collagen disorganisation and necrosis.29 Corticosteroids are also commonly paired with local anaesthetic which is also tenotoxic, adding to these effects.
These adverse effects on mechanical properties and cellular function of tendons may contribute to the poorer long-term outcomes reported from cortisone injection, even when paired with a superior active intervention.
Such impacts may also reduce the effects of an otherwise superior exercise-based intervention. In community general practice, CSI is commonly prescribed alongside a referral for physical therapy for patients with gluteal tendinopathy. The assumption is that the CSI will reduce pain to allow more effective rehabilitation, but in fact the opposite may be true – CSI may delay or reduce outcomes from a successful active intervention.30
There is no evidence currently to support this suggestion in hip tendinopathies, but for a similar upper limb tendinopathy at the lateral elbow, adding CSI to the active intervention resulted in delayed and poorer outcomes than the exercise intervention alone.30
This may be related to a mix of the biological (reduced tissue health) and psychological/behavioural effects. Rapid pain relief following a corticosteroid-local anaesthetic injection often appears to result in reduced compliance to both load management and exercise plans. This may contribute to poorer outcomes and a return for further injections… and so the spiral may begin.
Corticosteroid injection, tendon rupture and risk of failed non-surgical and surgical interventions
In the scientific literature, there is currently no available evidence that has closely examined the relationship between corticosteroid injection, tendon rupture and risk of failed non-surgical and surgical interventions for gluteal or proximal hamstring tendinopathies.
In surgical studies for gluteal tendon repair, participants have usually had multiple corticosteroid injections pre-surgery. Not surprising, right? If they have failed a rehabilitative program or have only been offered or opted for a passive-therapy-only management plan, they will almost certainly be offered CSI at least once, and usually multiple times before surgery is considered.
This is understandable, but there is a chicken or egg question here. What was the first-line management – CSI or education and exercise? If CSI was offered first, or with rehab, did this CSI limit ability to achieve a patient acceptable symptom state, resulting in return for further CSI, further increasing chances of tissue deterioration and reducing chances of success of conservative care?
Does this lead to a downward spiral of tissue disrepair and dysfunction that for some, may end in tendon disruption and a surgical intervention. Could abstinence from CSI have reduced the risk of such a downward spiral?
And does that poor tissue health entering into surgery reduce chances of good surgical outcomes, or increase the risk of re-tear of tendon repair? This is unknown for hip tendon repair, but for rotator cuff repair, one systematic review found that preoperative CSIs increased the risk of revision surgery when administered within 6-12 months of rotator cuff repair. Revision rates were highest when patients received 2 or more injections in the year prior to surgery.
This remains an issue of contention, along with key question that underlies all of this uncertainty: ‘how much cortisone is safe’? The general anecdotal answer from our medical colleagues is ‘2-3 a year’, but the truth is, no one really knows how much is safe. The safety threshold is likely to be different for different people and different stages of pathology, but we have no adequate guidelines to provide patients with evidence-based advice about how much is safe.
For management of gluteal tendinopathy at least, we have clear, high-quality evidence that an education and exercise approach is superior to a corticosteroid injection. Taking this fact together with the uncertainty regarding safety of CSI and possible adverse impacts on outcomes of rehab, my strong recommendation is – education and exercise first!
Repeated injections into soft tissue for tendon, muscle or nerve related pain may also result in fat necrosis and muscle atrophy.
Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.

Platelet Rich Plasma injections into the extra-articular tissues of the hip
Indications and benefits of platelet rich plasma injections for hip tendinopathy
The efficacy of PRP for management of tendinopathy has been investigated but limited evidence exists for gluteal tendinopathy or GTPS. For tendinopathy overall, the effects have been reported to be generally positive, although study designs, low sample sizes and wide variation in PRP preparation methods makes interpretation of the evidence difficult.32
One study comparing the effects of leucocyte-rich PRP and corticosteroid injections for PRP found that PRP provided statistically important clinical improvements compared with corticosteroid injections at 12 weeks, but there was no control group and both groups were provided with a home program of advice and exercise.33 The cohort was followed for 24 months, but no longer as an RCT. Those who did not have positive outcomes from the CSI were offered PRP after 12 weeks. Limited evidence currently suggests that PRP may be more efficacious than CSI in the medium to long term. However, without a control group and with a self-directed education and exercise program, it is unclear whether this effect would be greater than simply providing the advice and self-directed exercise program or a ‘wait-and-see’ approach.
A recent systematic review for interventions for proximal hamstring tendinopathy found no high or moderate quality evidence for platelet-rich plasma injection, again leaving its role as uncertain.34
Further evidence is required to clarify the role PRP should play in the management of hip tendinopathies and at which stage PRP may be most appropriately used.
Possible risks of platelet rich plasma injections for hip tendinopathy
In human studies, adverse reactions have been reported to be mild and infrequent. PRP does not have the disadvantage of the toxic effects of local anaesthetics and corticosteroids. However, there is still a lack of complete understanding of the variability of cellular responses induced by differing preparations of PRP and at different stages of tendon pathology.
One in vivo study showed that one form of PRP (leukocyte-rich PRP) may be harmful to tendon stem cells.35 A recent review of in vitro studies and in vivo animal models assessing the effects of PRP in tendons reported that L-PRP has some potential positive effects on tendon healing compared to a control, but this seems time dependant – assisting in early stages of tendon healing but potentially detrimental in later stage tendon healing.36
These animal models involve inducing surgical or chemical damage to a tendon, so it is difficult to know whether this truly represents the processes occurring within a tendinopathic tendon in humans. Much further research is required to understand if and at what stage PRP can be recommended in the management of hip tendinopathies.
Last thoughts ...
What's the bottom line then? Hate to be repetitive but, EDUCATION & EXERCISE FIRST!
While local anaesthetics may have diagnostic use, these medications are cytotoxic and needle placement may involve ionising radiation. It is our responsibility as health professionals to ensure we have the best possible skills for clinical diagnosis, to avoid unnecessary diagnostic injections (which are not always highly accurate).
Corticosteroids, particularly when combined with local anaesthetic (which is common), are toxic to all our musculoskeletal tissues. In my opinion, these should not be offered as first line management for joint or soft-tissue related hip pain. We do not know how much is safe, and those at risk of more devastating adverse reactions are easily missed. So let's err on the side of caution and absolutely minimise use of corticosteroid injections.
Viscosupplementation and PRP have enticing potential benefits at a biological level, but in-vivo evidence in humans and clear evidence of clinical effect is still lacking. Further research is required before these can be widely recommended. Patients should be aware of the evidence to assist them to make an informed decision and weight up their risks - which are arguably lower than corticosteroid or even local anaesthetic injections.
Let's watch the research evolve!
Discover our Lateral Hip & Buttock Pain Course
If you enjoyed this blog, you might like to take the online course on Lateral Hip & Buttock Pain - 6 hours of guided online video content. Examine various joint-related, soft tissue-related and nerve-related conditions associated with lateral hip and buttock pain, their mechanisms, associated impairments, clinical diagnostic tests and management approaches. To learn more, take the lateral hip and buttock pain online course, or join me in an online or practical lateral hip and buttock pain workshop.
Have you heard about Hip Academy?
RECENT HIP ACADEMY MEETING TOPIC:
Injectables for the Hip - Helpful or Harmful?
A little about our recent live Hip Academy meeting, where we chatted about Injectables for the Hip, and if they are helpful or harmful.
The lecture included:
- General risks of hip injections
- Indications, mechanisms of action & potential risks of
- intra-articular hip injections
- extra-articular hip injections - focus on tendons
- Local anaesthetics, corticosteroids, viscosupplementation & PRP

Enjoy the benefits of a world class educational Hip Program, specifically designed by Dr Alison Grimaldi to help improve your knowledge surrounding the Hip and Pelvis, and become an expert in your field + Get access to all previous member meeting recordings!
Meetings from 2023:
- Ligamentum Teres Injury - Relevance, Recognition & Rehabilitation
- The Power of Pelvic Tilt
- Injectables for the Hip - Helpful or Harmful?
- Ask Me Anything Session
- Member Case Sharing Event
Meetings from 2022:
- Rehabilitation considerations for hip arthroscopy
- Prehab & rehab following total hip arthroplasty
- The Hip & Pelvic Floor - Recognising & co-managing dysfunction
- Member Case Sharing Event
Meetings from 2021:
- Welcome & Dashboard Tour
- Deciphering Hip X Rays
- Preventing & Managing Gluteal Overactivity - Helping 'Hip Grippers'
- Lumbar vs Local - Tips for Differential Diagnosis of Buttock Pain
- Member Case Sharing Event

Enjoy the benefits of a world class educational Hip Program, specifically designed by Dr Alison Grimaldi to help improve your knowledge surrounding the Hip and Pelvis, and become an expert in your field + Get access to all previous member meeting recordings!
Check Out Some More Relevant Blogs
- Diraçoğlu D, Alptekin K, Dikici F, Balci HI, Ozçakar L, Aksoy C. Evaluation of needle positioning during blind intra-articular hip injections for osteoarthritis: fluoroscopy versus arthrography. Arch Phys Med Rehabil. 2009 Dec;90(12):2112-5. doi: 10.1016/j.apmr.2009.08.137. PMID: 19969177.
- Zhang M, Pessina MA, Higgs JB, Kissin EY. A vascular obstacle in ultrasound-guided hip joint injection. J Med Ultrasound. 2018 Apr-Jun;26(2):77-80. doi: 10.4103/JMU.JMU_8_17. Epub 2018 Jun 12. PMID: 30065523; PMCID: PMC6029204.
- Mezian K, Ricci V, Mittal N, Novotný T, Chang KV, Özçakar L, Naňka O. Ultrasound-guided injection of the hip: Cadaveric description for the lateral approach. PM R. 2022 Dec 14. doi: 10.1002/pmrj.12932. Epub ahead of print. PMID: 36515662.
- Liou H, Long J, Kransdorf M, Schmieder S. CT-guided quadratus femoris injection for ischiofemoral impingement. Eur Radiol. 2023 Jun;33(6):3956-3960. doi: 10.1007/s00330-023-09497-0. Epub 2023 Mar 14. PMID: 36917261.
- Goeller A, Pogarell T, May MS, Uder M, Dankerl P. Evaluation of CT-Guided ultra-low-dose protocol for injection guidance in preparation of MR-Arthrography of the shoulder and hip joints in comparison to conventional and low-dose protocols. Diagnostics (Basel). 2021 Oct 4;11(10):1835. doi: 10.3390/diagnostics11101835. PMID: 34679533; PMCID: PMC8534975.
- Haws BE, Condidorio CG, Adler KL, Giordano BD. Diagnostic intra-articular injection with provocative functional testing predicts patient-reported outcomes following hip arthroscopy: a prospective investigation. J Hip Preserv Surg. 2022 Jun 25;9(3):158-164. doi: 10.1093/jhps/hnac025. PMID: 35992032; PMCID: PMC9389908.
- Hirji Z, Hunjun JS, Choudur HN. Imaging of the bursae. J Clin Imaging Sci. 2011;1:22. doi: 10.4103/2156-7514.80374. Epub 2011 May 2. PMID: 21966619; PMCID: PMC3177464.
- Zhang K, Li M, Yao W, Wan L. Cytotoxicity of local anesthetics on bone, joint, and muscle tissues: a narrative review of the current literature. J Pain Res. 2023 Feb 27;16:611-621. doi: 10.2147/JPR.S398329. PMID: 36875687; PMCID: PMC9983438.
- Piper SL, Kramer JD, Kim HT, Feeley BT. Effects of local anesthetics on articular cartilage. Am J Sports Med. 2011 Oct;39(10):2245-53. doi: 10.1177/0363546511402780. Epub 2011 Apr 22. PMID: 21515808.
- Lemos SE. Editorial Commentary: Periarticular and intra-articular injections may do the right thing for patients' pain but may be the wrong thing for their articular cartilage: Be careful. Arthroscopy. 2022 Jun;38(6):1996-1998. doi: 10.1016/j.arthro.2022.03.003. PMID: 35660190.
- Ayhan E, Kesmezacar H, Akgun I. Intraarticular injections (corticosteroid, hyaluronic acid, platelet rich plasma) for the knee osteoarthritis. World J Orthop. 2014 Jul 18;5(3):351-61. doi: 10.5312/wjo.v5.i3.351. PMID: 25035839; PMCID: PMC4095029.
- Zhao Z, Ma JX, Ma XL. Different intra-articular injections as therapy for hip osteoarthritis: a systematic review and network meta-analysis. Arthroscopy. 2020 May;36(5):1452-1464.e2. doi: 10.1016/j.arthro.2019.09.043. Epub 2020 Jan 7. PMID: 31919027.
- Gazendam A, Ekhtiari S, Bozzo A, Phillips M, Bhandari M. Intra-articular saline injection is as effective as corticosteroids, platelet-rich plasma and hyaluronic acid for hip osteoarthritis pain: a systematic review and network meta-analysis of randomised controlled trials. Br J Sports Med. 2021 Mar;55(5):256-261. doi: 10.1136/bjsports-2020-102179. Epub 2020 Aug 22. PMID: 32829298.
- Probst DT, Sookochoff MF, Harris-Hayes M, Prather H, Lipsey KL, Cheng AL. what is the rate of response to nonoperative treatment for hip-related pain? a systematic review with meta-analysis. J Orthop Sports Phys Ther. 2023 May;0(5):1-21. doi: 10.2519/jospt.2023.11666. PMID: 36892224; PMCID: PMC10176100.
- Wernecke C, Braun HJ, Dragoo JL. The effect of intra-articular corticosteroids on articular cartilage: a systematic review. Orthop J Sports Med. 2015 Apr 27;3(5):2325967115581163. doi: 10.1177/2325967115581163. PMID: 26674652; PMCID: PMC4622344.
- Kompel AJ, Roemer FW, Murakami AM, Diaz LE, Crema MD, Guermazi A. Intra-articular corticosteroid injections in the hip and knee: Perhaps not as safe as we thought? Radiology. 2019 Dec;293(3):656-663. doi: 10.1148/radiol.2019190341. Epub 2019 Oct 15. PMID: 31617798.
- Simeone FJ, Vicentini JRT, Bredella MA, Chang CY. Are patients more likely to have hip osteoarthritis progression and femoral head collapse after hip steroid/anesthetic injections? A retrospective observational study. Skeletal Radiol. 2019 Sep;48(9):1417-1426. doi: 10.1007/s00256-019-03189-x. Epub 2019 Mar 6. PMID: 30840099.
- Abraham PF, Varady NH, Small KM, Shah N, Beltran LS, Kucharik MP, Martin SD. Safety of intra-articular hip corticosteroid injections: a matched-pair cohort study. Orthop J Sports Med. 2021 Oct 25;9(10):23259671211035099. doi: 10.1177/23259671211035099. PMID: 34722784; PMCID: PMC8549476.
- Gerhardt MB, Robinson S. Editorial Commentary: Intra-articular Injection for Osteoarthritis - Is It Hip or Not? Arthroscopy. 2020 May;36(5):1465-1467. doi: 10.1016/j.arthro.2020.03.029. PMID: 32370907.
- Avila A, Do MT, Acuña AJ, Samuel LT, Kamath AF. How do pre-operative intra-articular injections impact periprosthetic joint infection risk following primary total hip arthroplasty? A systematic review and meta-analysis. Arch Orthop Trauma Surg. 2023 Mar;143(3):1627-1635. doi: 10.1007/s00402-022-04375-8. Epub 2022 Feb 12. PMID: 35150302.
- Albanese J, Feltri P, Boffa A, Werner BC, Traina F, Filardo G. Infection risk increases after total hip arthroplasty within 3 months following intra-articular corticosteroid injection. a meta-analysis on knee and hip arthroplasty. J Arthroplasty. 2023 Jun;38(6):1184-1193.e2. doi: 10.1016/j.arth.2022.12.038. Epub 2022 Dec 30. PMID: 36592824.
- Probst DT, Sookochoff MF, Harris-Hayes M, Prather H, Lipsey KL, Cheng AL. What is the rate of response to nonoperative treatment for hip-related pain? a systematic review with meta-analysis. J Orthop Sports Phys Ther. 2023 May;0(5):1-21. doi: 10.2519/jospt.2023.11666. PMID: 36892224; PMCID: PMC10176100.
- Zhao Z, Ma JX, Ma XL. Different intra-articular injections as therapy for hip osteoarthritis: a systematic review and network meta-analysis. Arthroscopy. 2020 May;36(5):1452-1464.e2. doi: 10.1016/j.arthro.2019.09.043. Epub 2020 Jan 7. PMID: 31919027.
- Berney M, McCarroll P, Glynn L, Lenehan B. Platelet-rich plasma injections for hip osteoarthritis: a review of the evidence. Ir J Med Sci. 2021 Aug;190(3):1021-1025. doi: 10.1007/s11845-020-02388-z. Epub 2020 Oct 5. PMID: 33015749.
- Liou H, Long J, Kransdorf M, Schmieder S. CT-guided quadratus femoris injection for ischiofemoral impingement. Eur Radiol. 2023 Jun;33(6):3956-3960. doi: 10.1007/s00330-023-09497-0. Epub 2023 Mar 14. PMID: 36917261.
- Mellor R, Bennell K, Grimaldi A, Nicolson P, Kasza J, Hodges P, Wajswelner H, Vicenzino B. Education plus exercise versus corticosteroid injection use versus a wait and see approach on global outcome and pain from gluteal tendinopathy: prospective, single blinded, randomised clinical trial. Br J Sports Med. 2018 Nov;52(22):1464-1472. doi: 10.1136/bjsports-2018-k1662rep. PMID: 30385462.
- Wang Y, Wang K, Qin Y, Wang S, Tan B, Jia L, Jia G, Niu L. The effect of corticosteroid injection in the treatment of greater trochanter pain syndrome: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2022 May 21;17(1):283. doi: 10.1186/s13018-022-03175-5. PMID: 35598025; PMCID: PMC9123821.
- Nissen MJ, Brulhart L, Faundez A, Finckh A, Courvoisier DS, Genevay S. Glucocorticoid injections for greater trochanteric pain syndrome: a randomised double-blind placebo-controlled (GLUTEAL) trial. Clin Rheumatol. 2019 Mar;38(3):647-655. doi: 10.1007/s10067-018-4309-6. Epub 2018 Sep 28. PMID: 30267357.
- Dean BJF, Lostis E, Oakley T, Rombach I, Morrey ME, Carr AJ. The risks and benefits of glucocorticoid treatment for tendinopathy: a systematic review of the effects of local glucocorticoid on tendon. Semin Arthritis Rheum. 2014;43:570–576. doi: 10.1016/j.semarthrit.2013.08.006. Epub 2013 Sep 26.
- Coombes BK, Bisset L, Brooks P, Khan A, Vicenzino B. Effect of corticosteroid injection, physiotherapy, or both on clinical outcomes in patients with unilateral lateral epicondylalgia: a randomized controlled trial. JAMA. 2013;309(5):461–469. doi: 10.1001/jama.2013.129.
- Cimino AM, Veazey GC, McMurtrie JT, Isbell J, Arguello AM, Brabston EW, Ponce BA, Momaya AM. Corticosteroid injections may increase retear and revision rates of rotator cuff repair: a systematic review. Arthroscopy. 2020 Aug;36(8):2334-2341. doi: 10.1016/j.arthro.2020.04.044. Epub 2020 May 8. PMID: 32389769.
- Miller LE, Parrish WR, Roides B, Bhattacharyya S. Efficacy of platelet-rich plasma injections for symptomatic tendinopathy: systematic review and meta-analysis of randomised injection-controlled trials. BMJ Open Sport Exerc Med. 2017;3(1):e000237. doi: 10.1136/bmjsem-2017-000237.
- Fitzpatrick J, Bulsara MK, O'Donnell J, Zheng MH. Leucocyte-rich platelet-rich plasma treatment of gluteus medius and minimus tendinopathy: a double-blind randomized controlled trial with 2-year follow-up. Am J Sports Med. 2019 Apr;47(5):1130-1137. doi: 10.1177/0363546519826969. Epub 2019 Mar 6. PMID: 30840831.
- Nasser AM, Vicenzino B, Grimaldi A, Anderson J, Semciw AI. Proximal Hamstring Tendinopathy: A Systematic Review of Interventions. Int J Sports Phys Ther. 2021 Apr 2;16(2):288-305. doi: 10.26603/001c.21250. PMID: 33842025; PMCID: PMC8016446.
- Zhang L, Chen S, Chang P, Bao N, Yang C, Ti Y, Zhou L, Zhao J. Harmful effects of leukocyte-rich platelet-rich plasma on rabbit tendon stem cells in vitro. Am J Sports Med. 2016 Aug;44(8):1941-51. doi: 10.1177/0363546516644718. Epub 2016 May 16. PMID: 27184544.
- Liu X, Li Y, Shen L, Yan M. Leukocyte and Platelet-Rich Plasma (L-PRP) in tendon models: a systematic review and meta-analysis of in vivo/in vitro studies. Evid Based Complement Alternat Med. 2022 Dec 15;2022:5289145. doi: 10.1155/2022/5289145. PMID: 36569346; PMCID: PMC9780014.














