Femoral Malversion: Development and Prevention

Femoral malversion (excessive femoral anteversion or femoral retroversion) is increasingly recognised as an important factor that may influence mechanical loads around the hip and development of both intra-articular and extra-articular pathologies. To develop effective prevention strategies, we must first understand what it is, what impact it has, and how it develops.
These are the topics we’ll be covering in this blog:
· The impact of femoral malversion
· Natural development and change in femoral version through growth
Defining femoral malversion: Excessive femoral anteversion or femoral retroversion
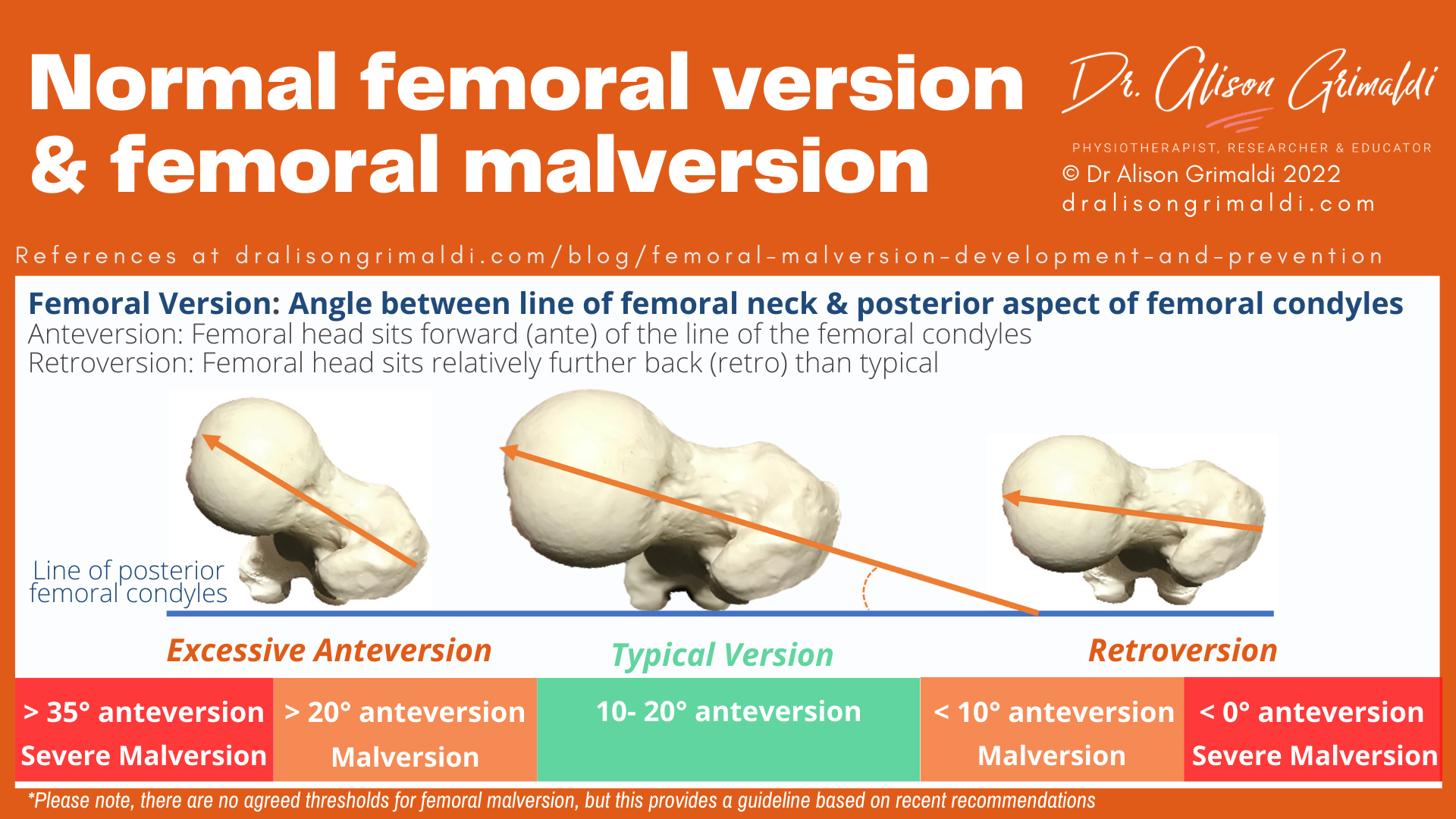
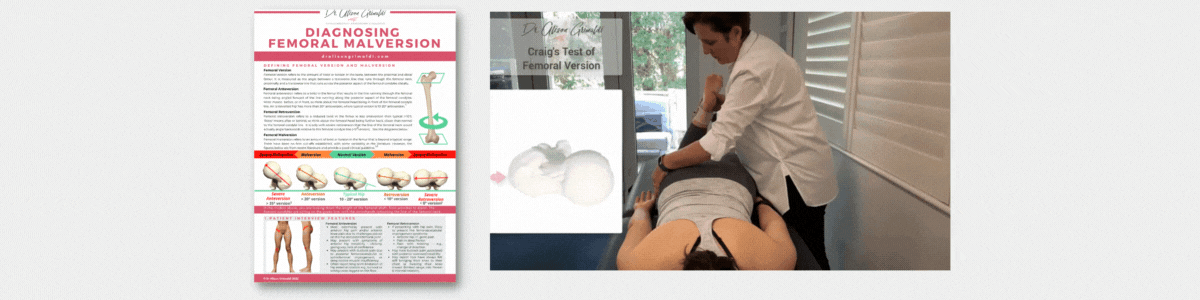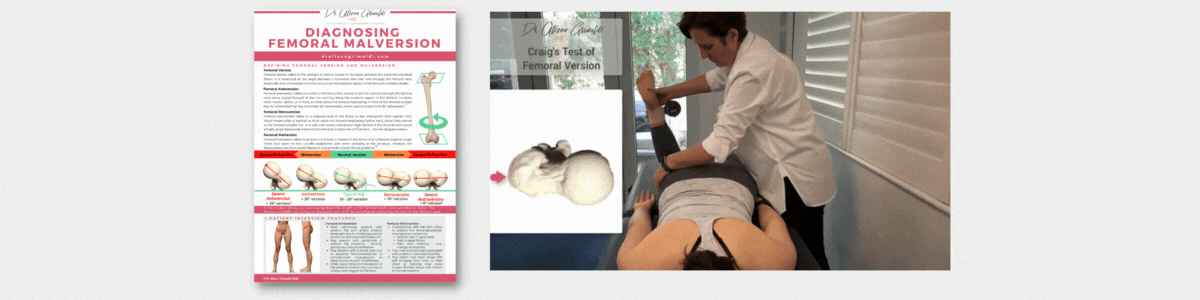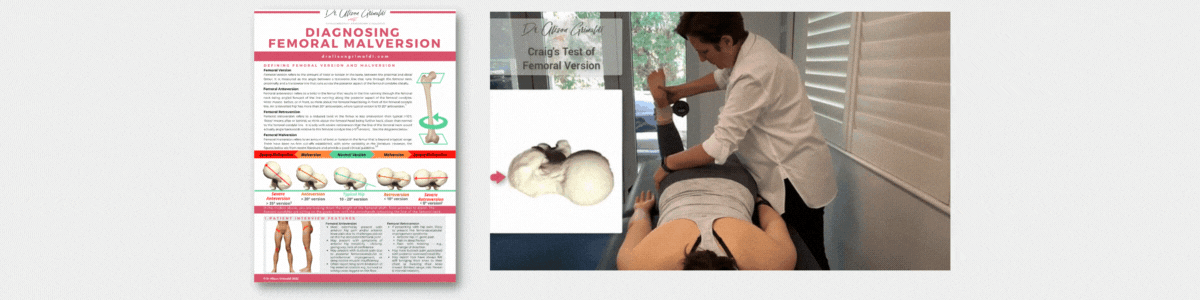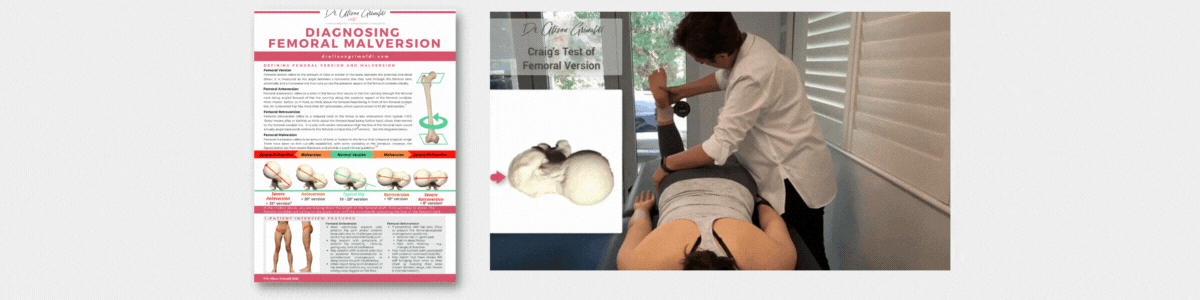
Femoral version refers to the normal torsion or twist we have in our femurs. Femoral version is measured as the angle between a line that bisects the femoral head and neck, and a line that runs across the posterior aspect of the femoral condyles at the back of the knee (see the graphic below).
The typical human femur is anteverted somewhere between 10 and 20 degrees. This means that when the femoral condyles are horizontal, the head and neck twists forward (anteriorly – ante) 10-20 degrees.
Malversion refers to a twist in the femur that is greater than or less than this typical range. There are no agreed cutoffs, but these are the most recently suggested normative values.1,2
Suggested threshold values for femoral version and malversion
· Excessive femoral anteversion: > 20° anteversion
· Severe femoral anteversion: > 35° anteversion
· Femoral retroversion (less anteversion than typical): < 10° anteversion
· Severe femoral retroversion: < 0° anteversion
Learn how to measure femoral version in my Video Library – available within Hip Academy
The impact of femoral malversion
The information below covers relationships between femoral malversion and various potential functional and pathological effects. However, it’s important to note that direct causation is difficult to establish, so consider these as associations that are subject to change depending on other concurrent factors.
Falls, fatigue and balance in children with excessive femoral anteversion
Children with increased femoral anteversion were found to fall four times more during running (60%), and three times more during fast walking (21.42%) than their healthy peers (14.28%, 7.14% respectively). These children also reported functional difficulties and fatigue with walking long distances and standing on one spot.3
A recent study of healthy children (age 10-15, 44% female) with increased femoral anteversion (mean 24°) found these children had significantly poorer balance in multiple parameters than peers with a mean 15° of anteversion.4
For some children, these impacts may have further implications in terms of increased risk of falls-related injury, reduced self-confidence and reduced engagement in physical activity.

Excess femoral anteversion and muscle function
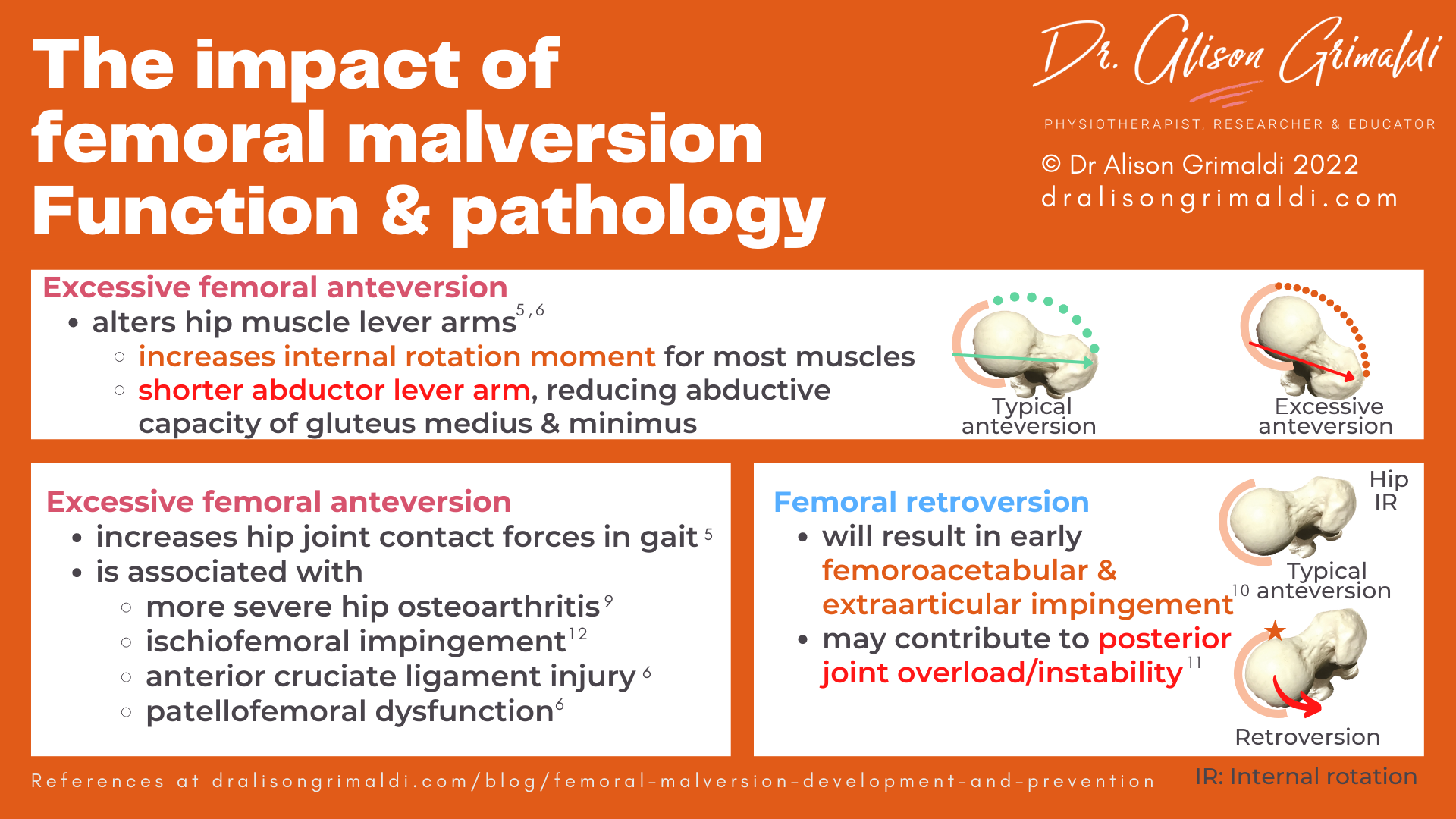
Higher femoral anteversion has an important influence on lever arm length of many hip muscles, with the most substantial impact on the hip abductors.5,6 Studies show a shorter abductor lever arm associated with higher femoral anteversion, thereby reducing abductive capacity of gluteus medius and gluteus minimus.
Most hip muscles also have a greater internal rotation moment and reduced external rotation movement in those with excessive femoral anteversion. This, together with the fact that internally rotating the hip helps restore the hip abductor lever arms,5 may contribute to the intoeing gait that is common in children with high degrees of femoral anteversion.
A common compensatory strategy for intoeing is external rotation of the tibia.7 This means that children with excessive femoral anteversion will not always be easily identifiable by intoeing gait.
Excess femoral anteversion and hip joint forces in gait
There is conflicting evidence when it comes to the relationship between femoral version and joint forces. A recent study of healthy adults found that higher femoral anteversion led to significantly higher anteromedial hip contact forces in gait, with the potential for altering risk of articular damage.5
Another study of adolescents reported that increased femoral anteversion does not lead to increased joint forces during gait.8 Both research groups noted that the impact was likely to be mediated by kinematic strategies and different muscle forces, a potential reason for variable results in relatively small cohorts (n ≈ 40).
So, femoral anteversion can potentially change joint forces, but it also depends on the way people move and how they use their muscles.
Femoral malversion and hip and knee pathologies
A recent systematic review and meta-analysis reported that excessive femoral anteversion may be a risk factor for more severe hip OA, independent of concurrent acetabular dysplasia. They also found a positive correlation between the amount of increased anteversion and severity of hip OA.9
There was not a strong correlation between femoral retroversion and development of OA.9 However femoral retroversion results in earlier femoroacetabular impingement, extra articular impingement10 and may contribute to increased risk of posterior hip instability.11 This is usually related to early anterior impingement, causing levering of the femoral head from the posterior acetabulum.
Increased femoral anteversion is also associated with ischiofemoral impingement with pathological signal changes in the quadratus femoris muscle and ipsilateral hip or buttock pain.12
At the knee, greater femoral anteversion angle is associated with increased risk of anterior cruciate ligament injury and patellofemoral dysfunction.6
Natural development and change in femoral version through growth
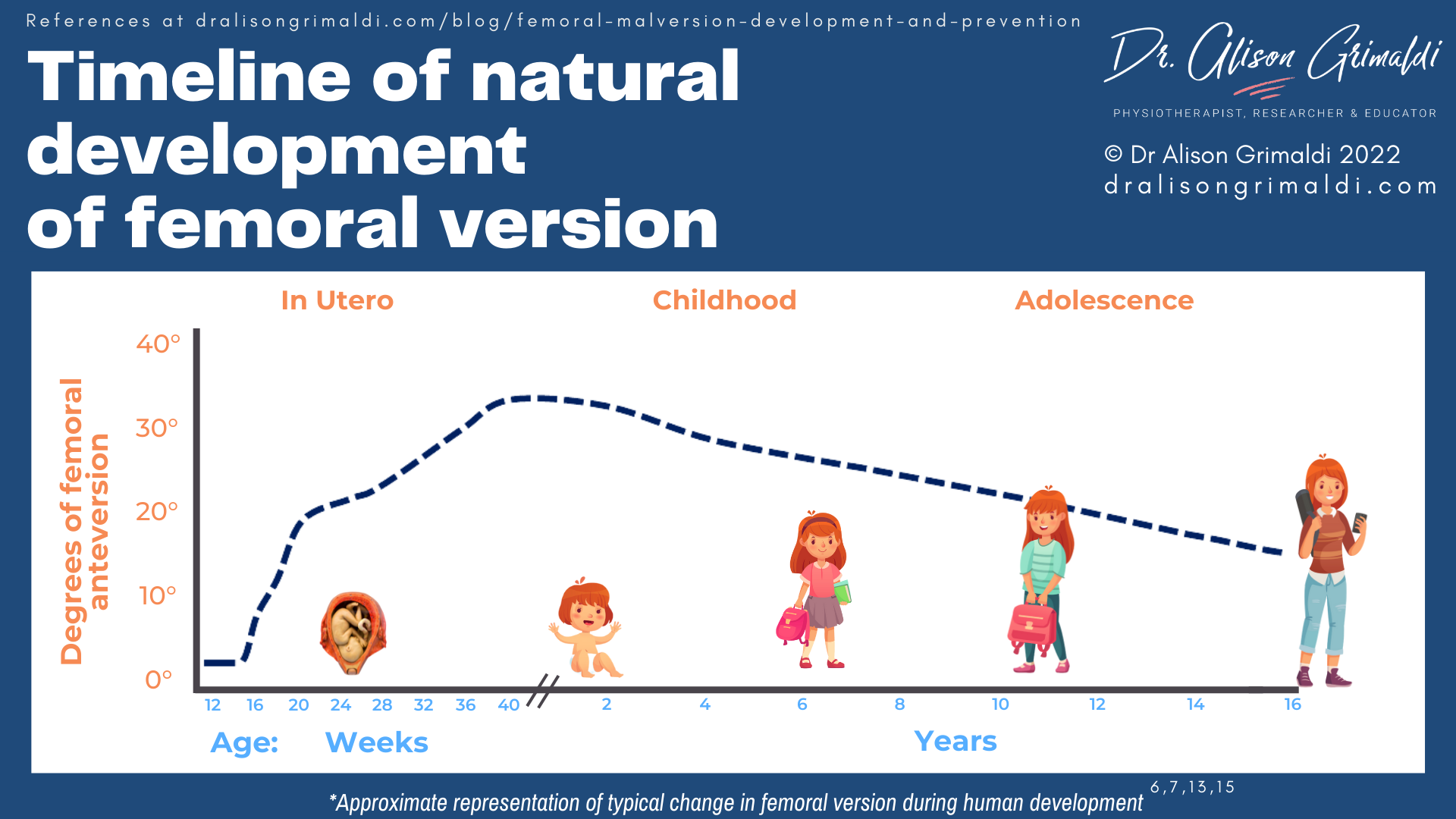
The course of the femur’s rotational development begins within the uterus. In early gestation, the human foetus has plenty of room to move and 0° of femoral version. From the second trimester, the confinement of the uterine walls begins imposing torsional loads on the limbs. The hips are forced into maximal flexion. Levering of the femoral shaft against the prominent anterior superior iliac spine has been hypothesized to create a torsional moment, resulting in femoral anteversion.12
Babies are born with 30-40° of femoral anteversion, gradually unwinding to around 15° in adulthood.12 During childhood and adolescence, a gradual decrease in anteversion of around 1.5° a year continues until growth is complete.6
Causes of excessive femoral anteversion and retroversion (femoral malversion)
Genetics and femoral version
Genetics is thought to play some role in the development of femoral version type, via a polygenetic influence on proximal femoral shape.13 There have been variable findings with regard to ethnicity, perhaps due to variation in measurement methods.
In a more recent CT study, no statistically significant differences were found between groups. However, almost 6% of African American males and females exhibited femoral retroversion, compared with only 0-2% of Caucasian and Hispanic participants.14
Sex differences in femoral version
While again there has been variation in findings, most studies report 2-8° higher angles of femoral anteversion in females compared with males. One suggestion is that this may be due to earlier closure of female growth plates, giving the femur less time to derotate.6
There may be other inter-related factors around muscle function and participation in weightbearing activities as we will explore below.

The influence of mechanical loading on development of femoral version
Mechanical loading appears to be a major player in changing femoral version both in utero and during childhood and adolescence.
Breech babies (born bottom first) are born with around 10° greater femoral anteversion than babies who have been in the head down position.15 For babies sitting bottom down in the mother’s pelvis, greater restriction of hip motion and pressure on the posterior femoral head and acetabulum is thought to create the higher levels of femoral anteversion.
Children with cerebral palsy (CP) are known to maintain much higher levels of femoral anteversion through growth – their femurs don’t tend to derotate. This suggests mechanical forces are highly significant in the normal femoral ‘derotation’ process that occurs through childhood.6
Weightbearing and femoral version
Reduced gravitational loading
So, what is the main factor maintaining femoral anteversion in children with CP? Is it the significant reduction in weightbearing activity, or the altered muscle forces?
It’s highly likely that these factors are linked, and both play a role. A recent lab-based study on immature rats demonstrated that reduced mechanical loading, achieved through hindlimb suspension during the growth phase, resulted in significantly higher angles of femoral anteversion. This suggests that weightbearing loads are not only important for development of bone density but also for bone shape development.
Differences in femoral anteversion between children with CP and normally developing children start to become evident at around 12 months of age.6 This is consistent with development of bipedal function. Most children start pulling to stand somewhere between 9 and 12 months, with typical onset of walking around 12 months.
While CP is an extreme example, lack of weightbearing activity also has the potential to impact on femoral growth in children without neurological deficits. It does raise the question:
Do reducing activity levels in our children put them at higher risk of maintaining excessive femoral anteversion and the impacts of this morphology?
Increased gravitational loading
At the other end of the gravity spectrum, obesity in adolescence is associated with reduced femoral version. Galbraith and colleagues reported a mean version angle of only 0.4° ± 13° in obese adolescents – representing relative retroversion.16 Carrying extra load against gravity appears to accelerate femoral ‘derotation’ during growth.
Femoral retroversion places greater shear force across the growth plate, increasing risks of epiphyseal slippage. This may be one of the key reasons why slipped capital femoral epiphysis is more common in obese adolescents.13
Type of sport and femoral version
A more recent study by Yadav and colleagues used finite element modelling to predict growth rate and growth direction of the proximal femur in response to various hip contact force scenarios.17 They found that femoral anteversion reduced more when the lateral hip contact force was similar or higher than the posterior hip contact force.
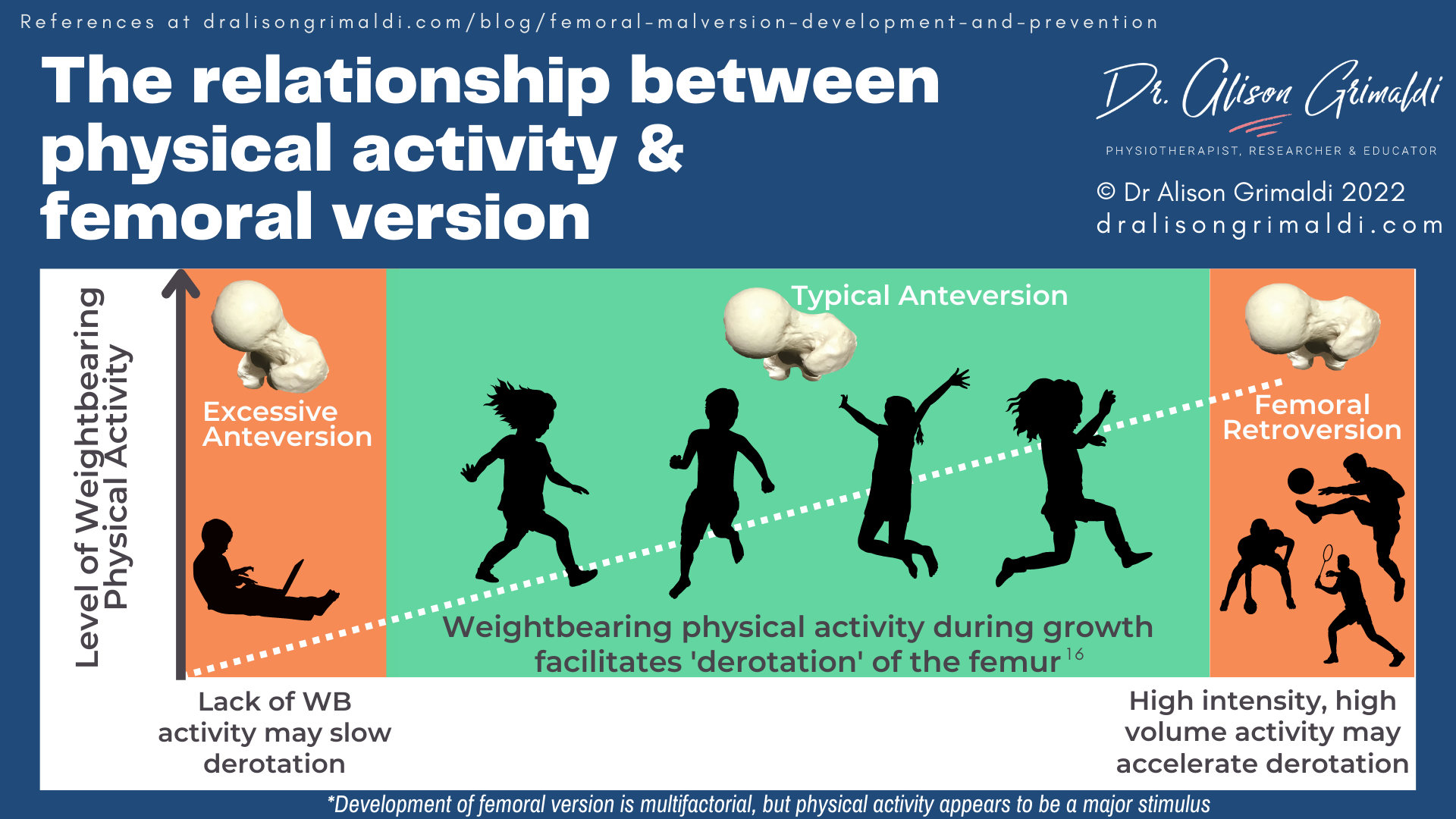
Physical activities that have more laterally than posteriorly oriented hip contact forces include many weightbearing activities such as walking, climbing and descending stairs, jumping and running.
Children with low physical activity levels or who participate in high volume water-based sports with low exposure to weightbearing loads, may be at greater risk of completing their growth with excess femoral anteversion.
At the other end of the spectrum, Yadav and colleagues suggest that performing these weightbearing activities at high volume and at high intensity, could be expected to accelerate femoral morphological changes.17 Young athletes playing high volume weightbearing sports may then complete their growth with relative femoral retroversion.
In my last blog, I talked about the relationship between high volume weightbearing sports and the increased risk of developing cam morphology. High volume ‘hip-heavy’ sports could possibly increase the chances of both cam morphology and femoral retroversion. The combination of both these morphologies will result in femoracetabular impingement earlier in hip flexion10 and internal rotation range.
Certainly not everyone with cam morphology has femoral retroversion, but the combination has been shown to increase the chances of early impingement.10 Lerch and coinvestigators also found significantly lower mean femoral version in those with symptomatic cam-type FAI compared with control participants.2
Muscle forces and femoral version
The effect of muscle forces on femoral version
The finding of excessive femoral anteversion in children with CP is not simply due to a lack of weightbearing, because ambulant children with CP have higher levels of femoral anteversion than non-walking children with CP.6 Healthy motor development and muscle forces must also play a role.17
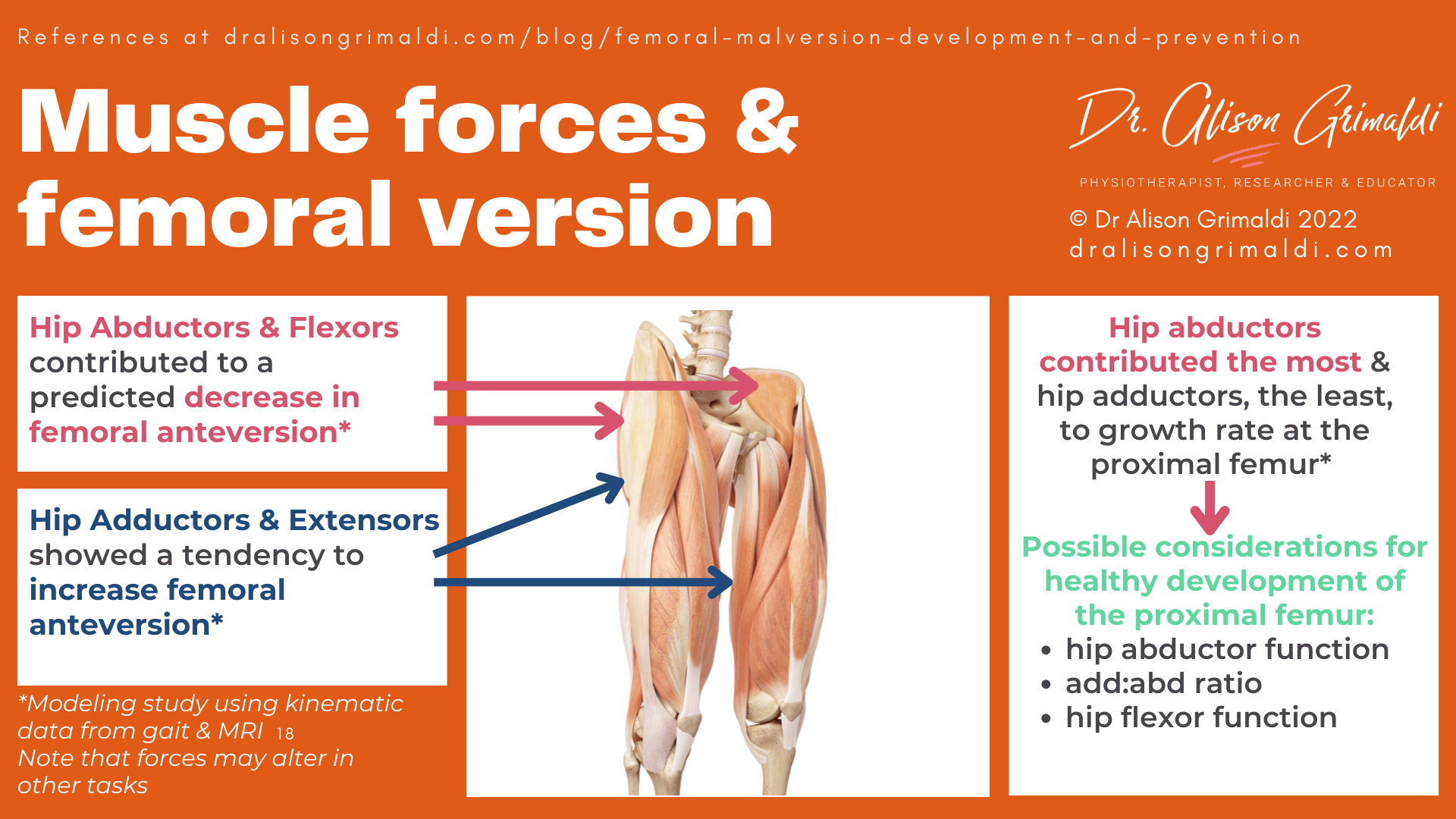
Yadav and colleagues used 3D kinematic data and MRIs to develop models that aimed to illustrate how different muscle groups’ activation during gait affects proximal femoral development in able-bodied children.18 They found that the hip abductors contributed the most, and hip adductors the least, to growth rate at the proximal femur.
While forces imposed by the hip abductors and flexors contributed to a predicted decrease in femoral anteversion, the hip adductors and extensors showed a tendency to increase femoral anteversion.18 This might explain how spasticity of the hip adductors in children with CP may contribute to maintenance of hip femoral anteversion, as previously suggested.
Antagonist strength ratio’s may be important in the developing femur. For example, higher hip adductor strength than abductor strength may favour femoral anteversion. The adductor:abductor ratio is something that is often used as an indicator of optimal muscle balance and possible resilience against groin injury. The optimal ratio for soccer players has been suggested to be in the range of 1.25 – 1.6, adductors stronger than abductors.19
While stronger adductors might reduce groin injury risk, in skeletally immature athletes this muscle imbalance in favour of the adductors could alter proximal femoral development.
According to Yadav, relative hip flexor and extensor loads may also play an important role.18 Hip flexor weakness or short hip flexors with poor ability to generate force through sagittal motion may favour femoral anteversion. Yadav sites research that found shorter hip flexors and higher femoral anteversion in female soccer players.20
This paper collected hip abductor muscle strength measures but not adductor strength, so the ratio in these players is unknown. They did report poor frontal plane femoro-pelvic control in a step-down task, which could suggest inadequate abductor function. In soccer players with presumably higher adductor strength, an imbalance in the adductor:abductor ratio may also have contributed to the lack of femoral ‘derotation’ and higher femoral anteversion.
Does ‘w sitting’ cause excessive femoral anteversion? The influence of sustained postures on femoral version
The answer to this question has not been resolved in scientific studies. Children with excessive femoral anteversion often tend to favour this position,21 but is the posture a cause or an effect of the excessive anteversion?
Sustained internal rotation has been shown to increase femoral rotation in immature rabbits - the longer the internal rotation position was sustained with splinting, the greater the femoral anteversion.22 Habitual w-sitting for long durations may for some children, over time, impose enough torsional load to slow the derotation process.
However, a healthy child who is moving in and out of this position regularly and engaging in plenty of weightbearing activity, is likely to simply grow out of this habit as their femurs naturally derotate.

Prevention of femoral malversion
The role of femoral malversion is only in recent times becoming more recognised. While we are now beginning to gain greater insights into the impact of femoral malversion, the scientific literature has not yet explored preventive strategies.
In the absence of scientific evidence then, we can use the information available to develop some biologically plausible strategies.
I have paired the key pieces of biological information with some suggested strategies for you in a free pdf download available below.
Download this FREE Resource on the Prevention of Femoral Malversion
Simply head to the link below to sign up to our mailing list and receive your free download, sent directly to your inbox. You can unsubscribe any time and your personal details will never be shared.
You can find heaps more information about assessing femoral version and managing femoral malversion in the courses and video technique video available within Hip Academy.

-
- A detailed examination of mechanisms of physical overload (morphology, movement, muscle) and impairments associated with anterior hip pain and groin pain, clinical diagnostic tests and management approaches.
- Including joint related-pain & bony impingement (intra & extra-articular), soft tissue-related pain and nerve-related pain.
- All Online Hip Courses
- eBook Series
- Growing How-to Video Library
- Growing PDF Resource Library
- Live Hip Academy Zoom Meetings - Additional exclusive lecture content
- Recordings of all previous meetings
- Hip Academy Forum
Check Out Some More Relevant Blogs
Another great Anterior Hip Pain blog

Anterior Hip Pain: Causes & Contributing Factors
Adequate consideration of individual causes and contributing factors is important for best outcomes.
References
- Frasson VB, Herzog W, Johnston K, Pauchard Y, Vaz MA, Baroni BM. Do femoral version abnormalities play a role in hip function of patients with hip pain? Clin Biomech (Bristol, Avon). 2022 Jul;97:105708.
- Lerch TD, Todorski IAS, Steppacher SD, Schmaranzer F, Werlen SF, Siebenrock KA, Tannast M. Prevalence of femoral and acetabular version abnormalities in patients with symptomatic hip disease: a controlled study of 538 hips. Am J Sports Med. 2018 Jan;46(1):122-134.
- Leblebici G, Akalan E, Apti A, Kuchimov S, Kurt A, Onerge K, Temelli Y, Miller F. Increased femoral anteversion-related biomechanical abnormalities: lower extremity function, falling frequencies, and fatigue. Gait Posture. 2019 May;70:336-340.
- Tuncer D, Gurses HN, Senaran H, Uzer G, Tuncay I. Evaluation of postural control in children with increased femoral anteversion. Gait Posture. 2022 Jun;95:109-114.
- De Pieri E, Friesenbichler B, List R, Monn S, Casartelli NC, Leunig M, Ferguson SJ. Subject-specific modeling of femoral torsion influences the prediction of hip loading during gait in asymptomatic adults. Front Bioeng Biotechnol. 2021 Jul 21;9:679360.
- Scorcelletti M, Reeves ND, Rittweger J, Ireland A. Femoral anteversion: significance and measurement. J Anat. 2020 Nov;237(5):811-826.
- Fabry G, Cheng LX, Molenaers G. Normal and abnormal torsional development in children. Clin Orthop Relat Res. 1994 May;(302):22-6. PMID: 8168306.
- Alexander N, Brunner R, Cip J, Viehweger E, De Pieri E. Increased femoral anteversion does not lead to increased joint forces during gait in a cohort of adolescent patients. Front Bioeng Biotechnol. 2022 Jun 6;10:914990.
- Parker EA, Meyer AM, Nasir M, Willey MC, Brown TS, Westermann RW. Abnormal femoral anteversion is associated with the development of hip osteoarthritis: A systematic review and meta-analysis. Arthrosc Sports Med Rehabil. 2021 Sep 2;3(6):e2047-e2058.
- Lerch TD, Antioco T, Boschung A, Meier MK, Schmaranzer F, Novais EN, Tannast M, Steppacher SD. Hip impingement location in maximal hip flexion in patients with Femoroacetabular Impingement with and without femoral retroversion. Am J Sports Med. 2022 Sep;50(11):2989-2997.
- Mofidi A, Sankar R, Kutty S, Kaar K, Curtin W. Traumatic dislocation of hip joint following low-velocity trauma, similarities to glenohumeral instability. Eur J Orthop Surg Traumatol. 2002 Jan;12(2):108-14.
- Dablan A, Oktay C, Çevikol C. Ischiofemoral Impingement syndrome: Effect of morphological variations on the diagnosis. Curr Med Imaging. 2021;17(5):595-601.
- Hogervorst T, Eilander W, Fikkers JT, Meulenbelt I. Hip ontogenesis: how evolution, genes, and load history shape hip morphotype and cartilotype. Clin Orthop Relat Res. 2012 Dec;470(12):3284-96.
- Koerner JD, Patel NM, Yoon RS, Sirkin MS, Reilly MC, Liporace FA. Femoral version of the general population: does "normal" vary by gender or ethnicity? J Orthop Trauma. 2013 Jun;27(6):308-11.
- Hinderaker T, Uden A, Reikerås O. Direct ultrasonographic measurement of femoral anteversion in newborns. Skeletal Radiol. 1994 Feb;23(2):133-5.
- Galbraith RT, Gelberman RH, Hajek PC, Baker LA, Sartoris DJ, Rab GT, Cohen MS, Griffin PP. Obesity and decreased femoral anteversion in adolescence. J Orthop Res. 1987;5(4):523-8.
- Yadav P, Fernández MP, Gutierrez-Farewik EM. Influence of loading direction due to physical activity on proximal femoral growth tendency. Med Eng Phys. 2021 Apr;90:83-91.
- Yadav P, Shefelbine SJ, Pontén E, Gutierrez-Farewik EM. Influence of muscle groups' activation on proximal femoral growth tendency. Biomech Model Mechanobiol. 2017 Dec;16(6):1869-1883.
- Griffin VC, Everett T, Horsley IG. A comparison of hip adduction to abduction strength ratios, in the dominant and non-dominant limb, of elite academy football players. Journal of Biomedical Engineering and Informatics. 2016; 2(1):109-118.
- Chiaia TA, Maschi RA, Stuhr RM, Rogers JR, Sheridan MA, Callahan LR, Hannafin JA. A musculoskeletal profile of elite female soccer players. HSS J. 2009 Sep;5(2):186-95.
- Lincoln TL, Suen PW. Common rotational variations in children. J Am Acad Orthop Surg. 2003 Sep-Oct;11(5):312-20.
- Wilkinson JA. Femoral anteversion in the rabbit. J Bone Joint Surg Br. 1962 May;44-B:386-97. doi: 10.1302/0301-620X.44B2.386. PMID: 14040263.